Cierra Maffei and Daniel Dewey-Mattia
Andover, Mass.
Drug delivery to the anterior and posterior segments is hampered by numerous barriers, including the tear film, the three layers of the cornea and the sclera. Consequently, only about 5 percent of a topically administered drug enters the anterior segment. Even when drugs are injected subconjunctivally or directly into the vitreous, they face obstacles such as the heterogeneity of the vitreous, and often require frequent outpatient visits.
In order to solve, or at least mitigate, some of these issues, several new delivery and sustained- release systems are in development that aim to help treatments come closer to reaching zero-order kinetics (the constant release of drug over time) and thereby increase safety and reduce the requisite frequency of administration. Some of the most promising new technologies include bioadhesives, drug-infused contact lenses and ocular inserts for anterior ocular afflictions, as well as particulate injections and ocular implants for posterior segment diseases.
Anterior Solutions
• Bioadhesives. Alterations to drug formulation (i. e., pH- and viscosity-adjusting agents such as polyvinyl alcohol and methylcellulose) are known to have some effect in prolonging residence time in the cul-de-sac, but other, more intricate addenda can increase contact time, leading to enhanced drug transport.1 Bioadhesives may either bind to the surface of epithelial tissue or form a mucous coating. They establish contact by thoroughly wetting the surface, and possibly increase contact by inducing edema of the corneal epithelium and conjunctiva. Through these actions, the bioadhesive penetrates the intracellular spaces of the tissue, creating a greater exposed surface area.1 The bioadhesive polymers most common to ophthalmic drug development include hydroxypropyl methylcellulose (HPMC), carboxymethylcellulose (CMC) and polyacrylic acid (PAA) derivatives, as well as hyaluronic acid (HA). The last polymer is naturally present in the vitreous body and in low concentrations in aqueous humor.1 HA may also increase dwell time on the ocular surface via its affinity to the surface cell adhesion molecule CD44 expressed on the epithelium.
Use of bioadhesives has been shown to enhance and sustain drug delivery of various compounds, including using sodium hyaluronate solutions to aid pilocarpine absorption in dry-eye patients2 and using CMC to increase ocular concentration of timolol in glaucoma patients.3
• Contact lenses. Lenses used in conjunction with drugs are another potential way to extend drug contact with ocular tissues in order to increase bioavailability. Because of the proximity of a contact lens to the target tissues, researchers have been looking for possible ways to capitalize on this relationship since the seminal papers of Herb Kaufman, MD, on drugs and soft contact lenses in the early 1970s.4 The theory of successful extended delivery from the contact lens depends upon the introduction of drug into the lens, the maintenance of lens transparency despite drug loading, maintenance of the surface characteristics of the lens and good oxygen transmissibility. Techniques investigated to integrate drugs and contact lens materials include soaking contact lenses in a drug, as well as more complex techniques such as creating a hollow cavity between two "slices" of lens material and devel-opment of nanocapsules for integration into the contact lens polymeric matrix.5 Vistakon Pharmaceuticals is currently developing a novel anti-allergy contact lens with ketotifen. The use of collagen shields as bandage lenses has also been investigated for short-term drug delivery capabilities.6
• Ocular inserts. As we discussed briefly in the December 2009 column, ocular inserts for prolonged drug release are also available, and fall into either soluble or insoluble categories. The theory behind soluble inserts is that gradual drug release via interaction between the polymeric matrix and the tear film will make removal unnecessary. Insoluble inserts are more commonly associated with constant-rate release, but do require removal once the device is empty of drug.7
One example, Lacrisert (Aton Pharma)—a rod-shaped, soluble hydroxy propyl cellulose ocular insert—is placed in the inferior cul-de-sac with an applicator. Over the course of the day, the insert dissolves via tear film mixing to provide prolonged polymeric release.8 A study sponsored by Aton Pharma and presented at the 2009 meeting of the Association for Research in Vision and Ophthalmology discussed the effects of Lacrisert when used in a study of 30 contact lens wearers. After four weeks of dosing with Lacrisert, subjects demonstrated significant improvements in dryness and grittiness compared to baseline. A significant improvement from baseline tear-film breakup time was observed and mean ocular surface staining decreased significantly from baseline. (Curwen SJ, et al. IOVS 2009;50:ARVO E-abstract 4661)
Ocular inserts for delivery of oxytetracycline have also been investigated. The cylindrical rods were designed for insertion at the superior or inferior conjunctival fornix; testing demonstrated oxytetracycline concentrations sufficient for antimicrobial action lasting for several days.9 A non-biodegradable insert available in the 1970s, pilocarpine-loaded Ocusert Pilo (Alza Pharmaceuticals), was designed to be placed either in the upper or lower culde- sac for glaucoma, but was costly and had ejection problems.10 Disadvantages of inserts can include a lack of sufficient tears to allow for dissolution, and the po tential for discomfort.
The Posterior Segment
• Injectable microparticles and nanoparticles. Since no topical medication has been approved for posterior segment diseases, intravitreal, subconjunctival, sub-Tenon's and juxtamacular injections have become the primary treatments. Ideally, a drug injected into the posterior segment will spread uniformly throughout the vitreous and have a steady release profile. However, due to the lack of homogeneity of the vitreous and the presence of numerous gradients—including the oxygen, protein, vitreal flow and pressure gradients—significant variability in drug concentration is often observed at the target site. These injections usually require frequent visits in order to maintain efficacy.
These problems have led investigators to develop new forms of drug delivery to the posterior segment that provide a longer duration of action and spread more uniformly throughout the vitreous. One such alternative is the use of small polymer-encapsulated drugs called nanoparticles or microparticles, as well as lipid membrane encapsulated drugs known as liposomes. These delivery systems can assist in stabilizing the active form of a drug, increase halflife, increase drug absorption due to a slower elimination rate and reduce the risk of toxicity by decreasing peak concentrations.8 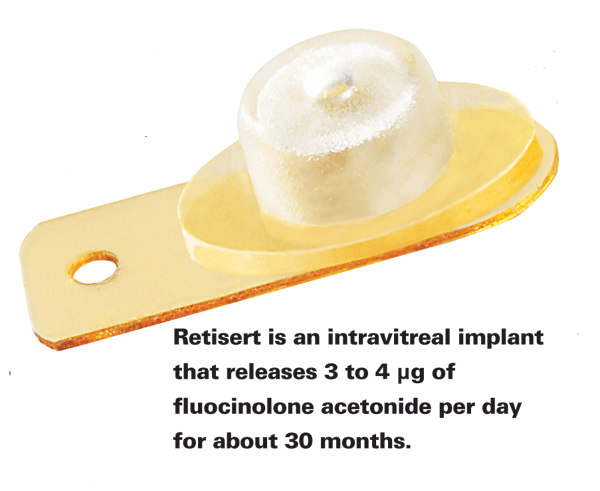
Injectable nanoparticles (1 to 1,000 nm in diameter) and microparticles (1 to 1,000 ìm ) can be made of a uniform polymer-drug combination, known as nanospheres or microspheres, in which the drug is spread equally throughout a polymer matrix; they can also be in the form of nanocapsules and microcapsules, in which the active agent is surrounded by a polymer capsule and released through pores. In both types of particulate systems, the speed of polymer biodegradation is the primary factor affecting the rate of drug release.11 These polymer systems can encapsulate almost any type of drug, eliminating the solubility issues of liquid injections. However, a problem with nanoparticles and microparticles is that they are heavier than the vitreous and tend to sink to the bottom of the posterior segment once injected, leading to an unequal distribution of drug.
Microparticles and nanoparticles are currently in preclinical testing for delivering prolonged gene therapy to the retina. Gene-based drugs such as fomivirsen (Vitravene, Novartis)—currently approved as an intravitreal injection for the treatment of CMV retinitis—may provide even longer-lasting treatment if encapsulated. Also in development is a unique type of nanoparticle called polyion complex (PIC) micelles, which are laser-activated in a process known as photochemical internalization: The process uses light to transfer DNA into cells.12 In a rat model of choroidal neovascularization, PIC micelles successfully produced transgene ex pression of anti-angiogenic factors.12
• Liposomes. Aside from encapsulation within a polymer, drugs can also be delivered inside microscopic phospholipid bilayers known as liposomes. Because of their affinity for cell membranes, liposomes can more easily bind to cell surfaces and facilitate drug transfer. Hydrophilic and hydrophobic drugs can both be delivered using liposomes, and preclinical research has shown that they can effectively transfer genes into the rat retina.13 A Phase II study investigating the safety and efficacy of liposomal vincristine injection (Marqibo, Hana Biosciences) for the treatment of metastatic uveal melanoma is currently ongoing. The liposome formulation may provide a slower, more consistent release, and may therefore prove more effective than currently available agents.
• Implants. Conceptually, intravitreal implants are intended to provide sustained drug release to the posterior segment, outlasting both solution and particulate injections. They are surgically inserted into the vitreous, typically at the level of the pars plana, and are generally classified as either biodegradable or non-biodegradable. Non-biodegradable implants provide a more controlled drug release compared to biodegradable implants, but require a second surgical procedure for their removal. On the other hand, biodegradable implants don't require surgical removal, but often have a final, uncontrolled burst in their profile.
Implants have several advantages over other types of drug delivery, including more consistent levels of drug release, a smaller quantity of drug needed for treatment, and avoidance of the pulse effect. As with solution and particulate systems, however, they also can cause unequal drug distribution due to vitreous heterogeneity and placement of the implant peripheral to the retina, done in order to avoid interference with the visual field. Implants also carry the risk of infection following insertion, as well as a risk of conditions caused by prolonged drug exposure.
There are currently two FDA-approved sustained-release corticosteroid implants. The first is a non-biodegradable implant which releases 0.59 mg of fluocinolone acetonide (Retisert, Bausch & Lomb) for a duration of approximately 30 months and is indicated for the treatment of chronic non-infectious posterior uveitis. The implant, however, is associated with a high frequency of corticosteroid-in - duced side effects including cataract formation in almost all phakic eyes and increased IOP, usually requiring pharmacologic or surgical intervention.14 Another more recently approved corticosteroid implant releases 0.7 mg of dexamethasone (Ozurdex, Allergan) through a biodegradable polymer that slowly breaks down to lactic and glycolic acid over a period of one to three months. The dexamethasone implant is indicated for the treatment of macular edema associated with retinal vein occlusion, and is also associated with in creased rates of IOP elevation.
A third non-biodegradable implant, containing 4.5 mg of the antiviral drug ganciclovir (Vitrasert, Bausch & Lomb), is approved for the treatment of cytomegalovirus retinitis in patients with AIDS. The implant is designed to work over a period of six to eight months, at which point the implant may need to be removed and replaced depending on the infection's course.
Numerous sustained-release, ocular drug delivery systems are either available or in development to provide an increased duration of action and reduce the need for frequent administration. These new technologies are especially useful for individuals faced with chronic eye diseases, such as dry eye and uveitis, but are also valuable for those unresponsive to more conventional therapies such as topical drops or intravitreal injections. With several new systems undergoing testing, many advances await in the field of ocular drug delivery.
Dr. Abelson, an associate clinical professor of ophthalmology at Harvard Medical School and senior clinical scientist at Schepens Eye Research Institute, consults in ophthalmic pharmaceuticals. Ms. Maffei and Mr. Dewey-Mattia are medical writers at Ora Inc. in Andover.
1. Kaur IP, Smitha R. Penetration enhancers and ocular bioadhesives: Two new avenues for ophthalmic drug delivery. Drug Dev Ind Pharm 2002;28:4:353-69.
2. Snibson GR, Greaves JL, Soper ND, et al. Precorneal residence times of sodium hyaluronate solutions studied by quantitative gamma scintigraphy. Eye (Lond) 1990;4(Pt 4):594-602.
3. Kyyronen, K, Urtti A. Improved ocular/systemic absorption ratio of timolol by viscous vehicle and phenylephrine. IOVS 1990;31:9:1827-33
4. Kaufman HE, Uotila MH, Gasset AR, et al. The medical uses of soft contact lenses. Trans Am Acad Ophthalmol Otolaryngol 1971;75:2:361-73.
5. Gulsen D, Chauhan A. Ophthalmic drug delivery through contact lenses. Invest Ophthalmol Vis Sci 2004;45:7:2342-7.
6. Higaki S, Myles ME, Loutsch JM, Hill JM. Corneal collagen shields for ocular drug delivery. In: Mitra AK, ed. Ophthalmic Drug Delivery Systems, v. 130. New York: Marcel Dekker, 2003. Pp. 309-334
7. Saettone MF, Salminen L. Ocular inserts for topical delivery. Adv Drug Deliv Rev 1995;16:95-106.
8. Del Amo EM, Urtti A. Current and future ophthalmic drug delivery systems. A shift to the posterior segment. Drug Discov Today 2008;13:3-4:135-43.
9. Johnston TP, Dias CS, Mitra AK. Mucoadhesive polymers in ophthalmic drug delivery. In: Mitra AK, ed. Ophthalmic Drug Delivery Systems, v. 130. New York: Marcel Dekker, 2003.
10. Chun DK, Shapiro A, Abelson MB. Ocular Pharmacokinetics. In: Albert DM, Jakobiec FA, eds. Principles and Practice of Ophthalmology, 3rd ed. Canada: Elsevier, 2008; v. 1.
11. Csernus VJ, Szende B, Schally AV. Release of peptides from sustained delivery systems (microcapsules and microparticles) in vivo. A histological and immunohistochemical study. Int J Pept Protein Res 1990;35:6:557-65.
12. Tamaki Y. [Novel approach for management of age-related macular degeneration--antiangiogenic therapy and retinal regenerative therapy]. Nippon Ganka Gakkai Zasshi 2007;111:3:232-68.
13. Masuda I, Matsuo T, Yasuda T, Matsuo N. Gene transfer with liposomes to the intraocular tissues by different routes of administration. Invest Ophthalmol Vis Sci 1996;37:9:1914-20.
14. Ramchandran RS, Fekrat S, Stinnett SS, Jaffe GJ. Fluocinolone acetonide sustained drug delivery device for chronic central retinal vein occlusion: 12-month results. Am J Ophthalmol 2008;146:2:285-91.



