Most technologies currently used to correct inadequate vision produce changes in the eye. The brain, however, is an equally important part of the visual system. A new treatment developed in Singapore appears to take advantage of neural plasticity—the brain's ability to learn and change—to improve contrast sensitivity at the level of the visual cortex.
The NeuroVision system, currently FDA-approved for the treatment of amblyopia in individuals nine years or older, is a non-invasive, patient-specific computerized treatment that forces the patient to identify fine details in visual stimuli. Data from clinical studies suggests that contrast sensitivity can be significantly improved by the treatment. (The treatment bears no relation to so-called "eye relaxation" techniques.)
Training the Visual Cortex
The NeuroVision system consists of a series of training sessions in which patients sit in a darkened room about five feet in front of a computer monitor that displays a series of visual perception tasks. (In Asia many patients go to vision centers for each session, but the treatment can also be done on a home computer.) When treating amblyopia, the strong eye is covered with special glasses.
A typical task involves identifying which of two images flashed on the screen contains a gabor patch. (See example, facing page.) As treatment continues, the gabor patch becomes harder and harder to see. Once the viewer begins to make mistakes, it becomes easier to see; when answers are correct again, it becomes harder. This appears to improve the brain's ability to identify small image parts and correctly integrate contours and edges.
After each session, the relevant information is uploaded to a data center where treatment for the next session is customized. The initial two sessions determine individual visual needs; after that, the level of difficulty of each session is based on the subject's progress.
Sessions generally last about 30 minutes, with two to four sessions per week, depending on the amount of visual impairment and pace of progression. The company recommends 45 sessions for treating amblyopia and 30 sessions for low myopia.
Getting Results
According to the company, the majority of improvement is usually seen in the first 15 sessions; the rest aid in retention. After every five treatment sessions, a doctor checks visual acuity to monitor the individual's progress; if a patient doesn't show improvement after 12 consecutive sessions, treatment is terminated.
A spokesman for NeuroVision notes that patients who do the treatment directly through the company are guaranteed to improve by at least two lines or they pay only a minimum service charge. However, patient selection criteria are important. The eye being trained must be better than 20/100 BCVA so the patient can see the stimuli, and strabismus must be less than 8 D, with no double vision.
In most cases, improvement is noticed within 10 sessions. In the clinical trial for amblyopia, the improvement was maintained after two years with no further sessions, except for adults with strabismus who continued to favor the other eye. Those patients needed periodic sessions to maintain the improvement.
"Doing this treatment is like 'photoshopping' the brain," says Donald Tan, deputy director of the Singapore National Eye Center and the Singapore Eye Research Institute, and associate professor of ophthalmology at the National University of Singapore. "If you have a blurred photograph, digital processing techniques can now sharpen the image artificially. The computer takes the image and breaks it up into pixels. Instead of a black, white and gray area, the software decides that this gray should really be black and this gray should really be white. This treatment trains the brain to do the same thing."
Promising Data
NeuroVision appears to have potential in a number of areas:
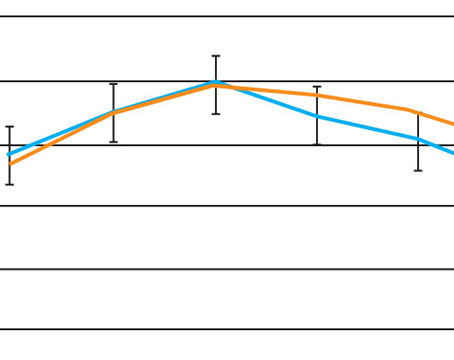
• Amblyopia. In a prospective, randomized, double-masked study conducted in Israel for the FDA involving 44 amblyopic patients, mean visual acuity improved more than 80 percent (2.5 lines); all ages showed improvement.1 (See chart, facing page.) A placebo group that received a bogus treatment showed no improvement. Pre-trial testing found that amblyopic individuals had significant contrast sensitivity loss in the higher spatial frequencies. The treatment raised high-frequency perception to within the normal range, as defined in the American National Standards Institute contrast charts developed by Arthur Ginsburg, MD. The improvement persisted after two years.
The FDA gave NeuroVision 510(K) approval for treating amblyopia based on this study.
• Low myopia. Like amblyopes, most myopic individuals have diminished contrast sensitivity. A pilot study conducted at the Singapore Eye Research Institute used the NeuroVision treatment to address low myopia (-1.5 D or less, with astigmatism up to 0.75 D) in 165 patients. Ninety-two percent gained one line or more; 73 percent gained two lines or more; 38 percent gained three lines or more; and 14 percent gained four lines or more (average improvement in both eyes). A full-scale, randomized, controlled trial is currently under way.
• Post-LASIK. Post-LASIK patients who completed the NeuroVision treatment because they were not satisfied with their post-surgery vision have also shown significant improvement in contrast sensitivity. Alain Leneveu, CEO of NeuroVision, notes that most current refractive procedures undermine contrast sensitivity. "In many cases the brain becomes confused because the data from the eyes has changed," he says. "In this situation, the brain may interpret faint signals as noise, and cut them off. We're just training the brain to distinguish what's noise and what isn't."
Challenges Ahead
August L. Reader III MD, FACS, who practices at the California Pacific Medical Center in San Francisco, isn't convinced. "The Israeli study is intriguing, but I'm still a little skeptical because this study was partly funded by NeuroVision," he says. "The fact that the FDA gave it 510(K) approval is significant, but more independent trials of the unit need to be done."
Dr. Reader notes that the treatment will tend to remind ophthalmologists of the "vision therapy" that some optometrists promote. "The fact that it sounds similar isn't going to help them," he points out. "They need to get some good studies done by ophthalmologists if they want to generate support in the MD community."
Motivation Counts
Mr. Leneveu notes that, unlike LASIK, NeuroVision does require serious effort on the part of the subject —but this can be an advantage. "We had a success rate of 80 percent during clinical trials," he notes. "But in the commercial environment, we have close to 90-percent success. People who pay for the service are really motivated—they're willing to work to achieve better vision."
Although the FDA-approved amblyopia treatment is currently available from Medical Services Options (201-670-9999), a spokesman for the company says that they won't begin a U.S. marketing campaign until they also have FDA approval for treating low myopia.
Currently, doctors can purchase an in-office station (including one day of training) for $3,500, or can have patients contact MSO directly. (Patients are required to do the program with their doctor providing periodic exams.) MSO charges patients $2,000 for a full treatment, plus $350/month to rent a computer station, or $1,000 to buy the station outright.
For more information about NeuroVision, visit neuro-vision.com.
1. Polat U, Ma-Naim T, Belkin M, Sagi D. Improving vision in adult amblyopia by perceptual learning. Proc Natl Acad Sci USA. 2004;101:17:6692-7. Epub 2004 Apr 19.