As surgeons consider new options to replace trabeculectomy, canaloplasty has attracted attention as a viable alternative. Canaloplasty is a non-penetrating glaucoma procedure that reduces intraocular pressure by opening—and holding open—Schlemm's canal; it requires no bleb or external device. The canal is uncovered via a scleral flap and intubated with a specialized cannula (iScience Interventional,
After the tip of the cannula emerges, a 10-0 prolene suture is tied to it; the cannula is then withdrawn, leaving the suture in its place. Tying off the suture provides tension that holds the canal open. (A high-resolution ultrasound system is available to help the surgeon visualize Schlemm's canal during the procedure.)
We asked two experts to talk about the current status of the procedure and the issues surrounding it.
Catching on Slowly
Manfred R. Tetz, MD, director of Spreebogen
"Canaloplasty evolved from the technique of viscocanalostomy," he explains. "Both techniques are designed to reestablish outflow through Schlemm's canal and collector channels. For whatever reason, only a few surgeons worldwide adopted the original viscocanalostomy technique from Professor Robert Stegmann, who invented it many years ago. Ever since, we've been a relatively closed group because the technique requires a great love of detail.
"Unlike viscocanalostomy, canaloplasty involves not just dilating Schlemm's canal at the site of the incision, but dilating it 360 degrees and putting a tension suture in," he continues. "However, this was very easily adopted by those of us who have been doing Schlemm's canal surgery for a long time. Other surgeons have to get used to the surgical steps involved in finding and entering Schlemm's canal and putting the catheter into the canal."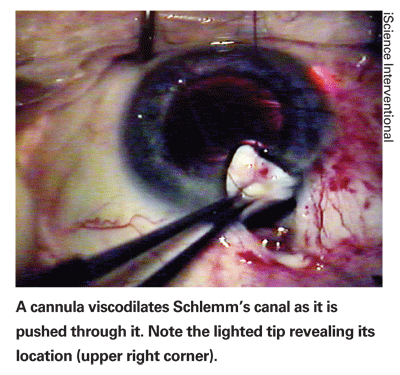
"Canaloplasty really isn't that difficult, although some Americans think it is," says Richard A. Lewis, MD, a cataract surgeon and glaucoma specialist practicing in
However, Dr. Lewis admits the procedure has a learning curve, and his own results have definitely improved with experience. "I'm quicker and my outcomes seem to be better," he says. "A lot of it, of course, is patient selection. Patients who have had previous trabeculectomies with scarring in the canal are not good candidates, and the angle has to be open. On the other hand, some patients can't have a bleb because they wear contact lenses, or have dry eye, or for cosmetic reasons. Those are ideal patients for this procedure."
Current Clinical Results
Drs. Lewis, Tetz and fellow researchers recently published one-year results from a prospective (but not randomized) study of canaloplasty involving surgeons in the
Dr. Lewis notes that the learning curve involved with the procedure probably prevented the results from being even better. "The more you do the procedure, the better your outcomes," he says. "Unfortunately, we couldn't start off with experienced doctors."
Dr. Lewis now has about 40 patients at 18 months. "Their results continue to hold," he says. "We haven't had long-term drift or failure yet. If you have success the first month, I suspect you're likely to have long-term success."
"Our longest follow-up now is approaching two years," says Dr. Tetz. "Those patients are still at their low postop pressure level, and they still have very low need for medication.
"This is similar to what I've seen with my viscocanalostomy patients," he continues. "Those who have reached the one month follow-up with their canal still functioning well are very likely to continue. The highest risk of failure occurs when late scarring is intense; with viscocanalostomy some patients drop out between months three and seven. But after a year the eye seems to have forgotten that you did the surgery."
Dr. Tetz notes that viscocanalostomy was often criticized for not reducing pressure sufficiently. He says the results with canaloplasty are significantly better. "I followed a series of 201 viscocanalostomy eyes for more than three years, and the average pressure was in the 16.5-mmHg range," he says. "With canaloplasty pressures are averaging in the 13.7- to 14-mmHg range. That's an additional 3 mmHg of pressure reduction."
Dr. Tetz says the reason for the difference may be the support provided by the canaloplasty suture. "With viscocanalostomy, once the pressure inside the eye slowly increases again, you may get a partial collapse of Schlemm's canal, making access to some of the collector channels more difficult," he explains. "When you put the suture in during canaloplasty, the canal can't collapse so easily. We don't see so many ups and downs in pressure, even over a 24-hour period."
Shortening the Learning Curve
"It's true that the learning curve affects outcome data in clinical trials like the current multicenter one," says Dr. Tetz. "Surgeons at the three German sites involved in the clinical trial have been doing viscocanalostomy for quite a while, and our results are somewhat better than the initial results from the
Asked how long it might take an average surgeon to learn the procedure, Dr. Tetz replies that this is like asking how long it will take to learn to ice skate. "Some people skate after an hour," he says. "Others have trouble for months. But overall, it shouldn't take the average surgeon too long."
Dr. Tetz says a key to mastering the procedure is to learn the details by studying the instructional videos that are available. "If you learn from experienced surgeons, you'll shorten the learning curve," he says. "With this approach you can learn the technique well within 30 or 40 procedures. If you think you can just plunge ahead because you know how to do a trabeculectomy, the road to success will be very long."
One aspect of the procedure that some surgeons are concerned about mastering is knowing when the suture is tight enough. Dr. Lewis admits that it can be tricky to judge this. "Getting the right tension currently depends on your surgical experience and skill," he admits. "The company is working on an alternative way of achieving a prescribed tension, but that's still in the future."
Dr. Tetz agrees that experience helps, but adds that you can look for indications that the tension is ideal using high-resolution ultrasound during the procedure. "You want to see that the suture has made a slight indentation toward the inside of the anterior chamber when you're putting your locking knot on your three-loop primary knot," he says.
Dr. Tetz notes some similarities to doing interrupted suture keratoplasty. "In that situation you do a triple or quadruple sling knot," he says. "Then you tighten it, so it's just the three slings lying there. Then you put one knot on top and have exactly the force that is needed to make one single four knot. That's usually good enough to get the tension right. But this is largely done by feel. No one doing keratoplasty with single interrupted sutures can tell you exactly how he's doing it."
Complications: It's All Relative
Asked about complications associated with canaloplasty, Dr. Tetz notes that the subject is tricky, because some effects of the surgery that would be considered complications under other surgical circumstances are desirable when performing canaloplasty—a non-penetrating procedure.
One of those effects is relative hypotony. "With viscocanalostomy, 10 or 20 percent of patients may have a very low postop pressure, even down to zero," he says. "But unlike other procedures, this will be a pressure of zero with a deep chamber. Zero with a flat chamber is a catastrophe. Zero with a deep chamber is normal, at least in this situation.
"The other effect that's normal with these procedures is a small regurgitation of blood into the anterior chamber," he continues. "Pressure in the episcleral veins pushes a little blood backwards through small openings into the chamber. As many as 10 to 20 percent of eyes will show microhyphemas in the early postoperative days. Again, this is normal. In fact, even a transient cystoid macular edema is normal if the pressure is between zero and five.
"I tell my patients that if they don't see well during the first five or six days, that's normal," he says. "I want to see this effect, because it means that your postop results are going to be better than if your pressure is immediately at 17. In fact, I like to see at least a third or more of my patients reach the zero to 5 mmHg range, because this is followed by better outcomes." He adds that it takes five to seven days for the pressure to go back up to the low teens.
Dr. Tetz says that complication rates will therefore depend how you define a complication. "If you count a pressure below 8 mmHg as a complication, or a hyphema as a complication, then the complication rate is around 25 percent," he says. "But when you're performing canaloplasty these are good signs, not problems."
As far as other complications such as anterior synechiae or fibrin exudation, Dr. Tetz says he seldom sees them in viscocanalostomy or canaloplasty. "Fibrin exudation occurs less than 1 percent of the time," he says. "Transient peripheral choroidal detachment occurs between 1 and 3 percent of the time, depending on which study you're looking at. Occasionally you see local bleeding under Descemet's membrane, which can be counted as a complication. And in the early part of surgery if you're trying to find Schlemm's canal you may rupture Descemet's window. If that happens, you're basically converting the procedure into a trabeculectomy."
In terms of long-term complications, Dr. Tetz says that out of his roughly 1,400 patients who have undergone either canalostomy or canaloplasty, the only complication he's seen is two patients whose pressure has hovered consistently between 5 and 8 mmHg. "Once in a while they may experience a mild episode of cystoid macular edema," he notes. "If that occurs I put them on one drop of steroid per day and the pressure goes up to 10 mmHg."
Points In Its Favor
Drs. Tetz and Lewis both see canaloplasty as having multiple advantages over other options. One of those advantages is how well it works in combination with cataract surgery.
"Canaloplasty seems to produce very good results in combined surgery or pseudophakic patients," notes Dr. Lewis. "Brad Shingleton's recent study [not yet published] showed a really good pressure drop. And the combination surgery is no more difficult than doing a trabeculectomy or Ahmed valve at the same time. However, canaloplasty avoids all of the complications you get with trabeculectomy. There's no bleb. You're not at the mercy of the scarring that happens after surgery, and there's no need to use mitomycin."
Dr. Tetz agrees, noting that he usually combines canaloplasty with cataract surgery. "You get an additional positive effect," he says, "and it's 100 percent better than trabeculectomy in this situation. You find no fibrin, no flat chambers, no synechiae. You get a lower pressure, but the chamber remains deep."
In general, Dr. Lewis says part of the appeal of canaloplasty for him is that it's a more physiologic approach to outflow than some of the alternatives. "It doesn't permanently alter the anatomy of the eye," he says. "I find that the most appealing of all its characteristics. It doesn't prevent or obviate any other surgery. You can always convert it to putting an Ahmed or Baerveldt implant in at some later date."
Dr. Tetz says he believes canaloplasty is a good choice as a replacement for trabeculectomy. "Overall, the pressure results of viscocanalostomy are comparable to those of trabeculectomy without mitomycin," says Dr. Tetz, "but with a much lower risk of postoperative complications and much less intense care required immediately postop. So far, the results of canaloplasty are even better."
1. Lewis RA, von Wolff K, Tetz M, Korber N, Kearney JR, Shingleton B, Samuelson TW. Canaloplasty: Circumferential viscodilation and tensioning of Schlemm"s canal using a flexible microcatheter for the treatment of open-angle glaucoma in adults: Interim clinical study analysis. J Cataract Refract Surg 2007;33:7:1217-1226.



