Surgeons who perform refractive surgery have often been viewed as being on the cutting edge, but it doesn't mean they can't be cautious when they have to be. That's the case with this month's National Panel Report on refractive surgery. In it, surgeons report that the average thickness of their LASIK flaps is decreasing, and that most of them are altering their practice patterns based on the threat of ectasia.
Those are just a few of the results from this month's report. In it, 31 surgeons, or 6 percent of the 500-surgeon sample, responded.
LASIK and Flaps
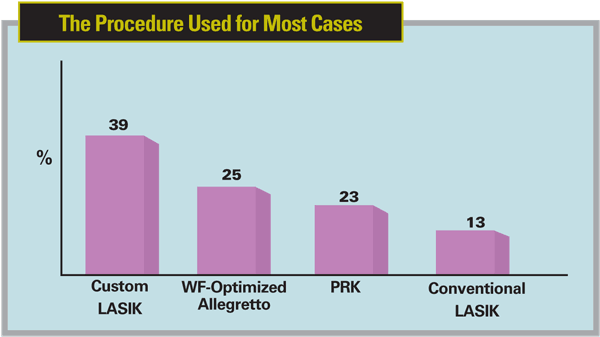
LASIK is still the dominant procedure among our panelists, with 77 percent of the surgeons saying it's the procedure they use for most of their cases. The rest choose PRK. Breaking down the LASIK responses, 39 percent choose custom LASIK, 25 percent use wavefront-optimized LASIK with the Alcon Allegretto and 13 percent prefer conventional LASIK. For making their flaps, 43 percent of the respondents use a femtosecond laser, with the rest using a microkeratome.
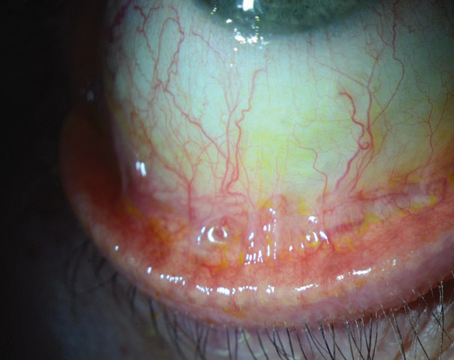
Of the surgeons who perform surface ablation, all of them say the use mitomycin-C prophylactically to stave off haze and regression. "We use mitomycin-C on all cases where there has been previous corneal surgery—PRK, Intacs, CK, PKP or LASIK," says a
When surgeons have to perform a LASIK enhancement, 57 percent say they lift the flap and ablate the stromal bed, while 43 percent avoid performing another LASIK and instead ablate the flap. No one advocates recutting a LASIK flap. "Never recut a flap," avers Andrew Caster, MD, of

A surgeon from
As many surgeons are experiencing in their own practices, LASIK volume has decreased an average of 33 percent for 46 percent of the respondents to the survey. Volumes stayed level for 26 percent of the surgeons, while 26 percent say it's increased for them by an average of 16 percent.
In terms of the bottom line, here are the average prices and costs the panelists report for their refractive surgeries:
• average charge per eye for LASIK: $2,257;
• average increase in price for custom LASIK over conventional: $233
• average facility fee paid for LASIK: $603;
• average charge per eye for PRK: $1,850;
• average charge per eye for clear lens exchange/intraocular lens implantation: $4,800.
Ectasia Concerns
For their initial LASIK, surgeons seem to be gravitating toward thinner flaps as a hedge against ectasia risk. The surgeons report an average flap thickness of 121 µm. This thickness has been steadily decreasing since 2007, when surgeons said they were shooting for, on average, flaps of 130 µm.
"I usually leave a stromal bed of at least 300 µm vs. 250 µm," says

Ninety-two percent of the panelists also say that the extra attention that's been paid to ectasia has affected the way they approach potential refractive-surgery patients.
"I focus more on ectasia during the informed consent process," says a surgeon from
Many surgeons say this conservative approach takes the form of performing more surface ablation, and saving some of the tissue that would be ablated with LASIK.
"I perform PRK on patients whose corneas are under 500 µm in thickness," says

Preferred Procedures
Surgeons were also asked how they would approach patients with certain refractive errors. Here's how they responded for different patient presentations:
• -3 D myope.Custom LASIK was the most popular choice for this type of patient, and it was chosen by 62 percent of panelists. A quarter chose PRK and 12 percent chose conventional LASIK. "Custom LASIK easily solves the problem," says Frank Rosenbaum, MD, of
A surgeon from
• -6 D myope.Custom LASIK is still the most popular option for this level of correction, with 62 percent of the surgeons saying they prefer it. Twenty-three percent would do surface ablation and 15 percent like conventional LASIK.
"My treatment of choice for this patient is PRK with the Allegretto Custom Wave," says Dr. Palumbo.
• -11 D myope.For the high myope, 60 percent of the surgeons say the best procedure is probably a phakic intraocular lens. Thirteen percent think clear-lens extraction/IOL implantation is the way to go, 13 percent like PRK, 6 percent would do custom LASIK and 6 percent would choose LASEK.
"LASIK is too invasive in the cornea for this patient," says
• +2 D hyperope.For the low hyperope, 60 percent say that LASIK would be the best procedure, 20 percent like PRK and 20 percent recommend clear lens extraction. "LASIK works well with low hyperopes," says Dr. Seltzer. However, Dr. Palumbo thinks the surface is the place to be. "PRK is controlled and safe," he says. "And I'm guided by past accuracy and results with it." But a surgeon from RO
1. Caster AI, Friess DW, Schwendeman FJ. Incidence of epithelial ingrowth in primary and retreatment laser in situ keratomileusis. J Cataract Refract Surg 2010;36:1:97-101.