According to researchers in
Included in this retrospective, multicenter, observational case series were 20,013 patients from nine cataract surgery centers in seven states. Inclusion criteria: topical anesthesia; clear corneal incision; uncomplicated phacoemuslification with an intraocular lens in the bag and treatment with preoperative and postoperative fourth-generation fluoroquinolones. Exclusion criteria: intraoperative complications; concurrent glaucoma or posterior segment surgery; wound leak requiring suturing at the end of the procedure; or delayed wound leak after surgery.
Participating surgeons performed 20,013 uncomplicated surgeries. Of these, 16,209 (81 percent) received topical gatifloxacin and 3,804 patients (19 percent) were treated with topical moxifloxacin as anti-infective prophylaxis. A total of 14 patients experienced endophthalmitis, an overall rate of 0.07 percent. Analysis found no statistically significant difference in infection rate between centers (p>0.5). The average age for patients with endophthalmitis was 65.7 years (range, 37 to 85 years). There were 10 females (72 percent) and four males (28 percent). Visual acuity at presentation ranged from 20/50 to light perception.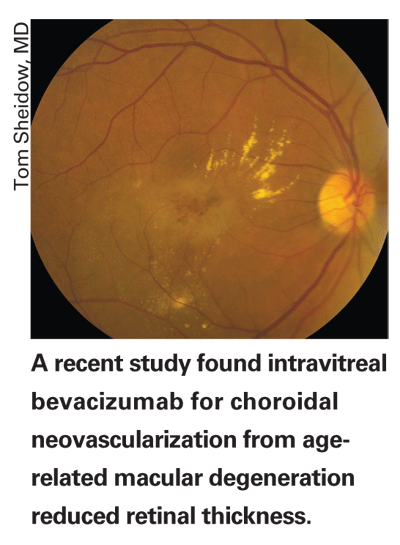 There were nine (0.06 percent) endophthalmitis patients in the gatifloxacin group and five (0.1 percent) in the moxifloxacin group, a non-statistically significant difference. In 10 of the patients, vitreous culture results were positive. Coagulase-negative Staphylococci, followed by Streptococci, species were the most commonly isolated organisms in the culture-positive patients.
There were nine (0.06 percent) endophthalmitis patients in the gatifloxacin group and five (0.1 percent) in the moxifloxacin group, a non-statistically significant difference. In 10 of the patients, vitreous culture results were positive. Coagulase-negative Staphylococci, followed by Streptococci, species were the most commonly isolated organisms in the culture-positive patients.
A number of factors such as wound integrity on postoperative days, the sterility of the instruments and possible poor patient compliance were not taken into consideration. Nor was it possible to obtain patient demographics linked to individual surgery outcomes, such as gender, ethnicity, age and so forth.
Given the low incidence of endophthalmitis, larger case studies may reveal an advantage to the use of fourth-generation fluoroquinolones or other anti-infective agents. And considering the variety of pre- and postoperative regimens among cataract surgeons, it is possible that more frequent dosing of an anti-infective agent may affect the rate of postop infection.
(Ophthalmology 2007;114:686-691)
Moshirfar M, Feiz V, Vitale AT, Wegelin JA, Basavanthappa S, Wolsey DH.
Intravitreal Bevacizumab Reduces Retinal Thickness in CNV
Intravitreal bevacizumab for choroidal neovascularization from age-related macular degeneration results in a rapid decrease in OCT-measured retinal thickness in a majority of cases, according to researchers in
The group reviewed all patients treated with intravitreal bevacizumab for CNV from AMD with visual acuity greater than 20/320 over a two-year period. OCT data recorded included central macular thickness and the presence or absence of cystic intraretinal fluid, subretinal fluid or pigment epithelial detachment at the time of initial injection, at one-week, one-month and three-month intervals, as well as at the end of follow-up.
Fifty-four eyes of 51 patients treated with intravitreal bevacizumab for CNV from AMD were identified. A total of 178 injections were performed; mean number per eye was 3.3. Mean number of days of follow-up was 138 with 91 percent of patients having at least 90 days of follow-up. Seventy percent of patients had undergone previous treatment for CNV. Combined treatment with photodynamic therapy was provided in 20 percent of cases at the initial intravitreal injection.
OCT data for all patients revealed an initial mean thickness of 362 µm, which was decreased at one week to 278 µm (p=0.001), 235 µm at one month (p<0.0001), 238 µm at three months (p=0.0004) and 244 µm for the end of follow-up (p<0.0001). Cystic retinal edema, subretinal fluid and pigment epithelial detachment resolved in the majority of cases, but PED frequently took longer to resolve. Initial mean VA was 20/125 (logMAR 0.8) and final mean VA was 20/100 (logMAR 0.7; p=0.03). There was no difference in OCT or VA outcomes (p=0.62 and p=0.28, respectively) between previously treated and treatment naïve patients. There was no difference in OCT or VA outcomes (p=0.67 and p=0.21, respectively) between patients who received combination therapy and those who received monotherapy with intravitreal bevacizumab. No systemic or ocular adverse events were recorded.
The short-term results, the small size and the lack of a control preclude definite conclusions. Also, OCT data were not routinely obtained in all patients at all visits for various reasons. Refractions were not done and so VA measurements may be underestimated. Adverse events were self-reported only by patients. Follow-up time was limited since the drug has been used in this manner for only a short time.
The researchers suggest further studies, particularly in light of the quality of life improvements that are now more attainable for patients and the formidable financial impact on AMD management these drugs might have.
(Retina 2007; 27:432-438)
Goff MJ, Johnson RN, McDonald HR, Ai E, Jumper JM, Fu A.



