Fusarium fungus resides in soil and on plants, primarily in tropical and subtropical climates, and infections are typically seen in agricultural workers of these regions.1 However, aberrations in this pattern do occur, and in fact the atypical incidence of Fusarium keratitis in northern regions of the United States provided some of the early red flags in this country during the recent outbreak.
The opportunistic filamentous fungus Fusarium can cause a variety of infections in humans: keratitis; endophthalmitis; otitis media; onychomycosis; cutaneous infections; pulmonary infections and endocarditis. Most commonly, Fusarium solani is reported as the culprit of ocular infections, and, unfortunately, this fungus is relatively intractable when it comes to treatment. Fungal infections tend to be resistant to drugs and penetrate deeper into the cornea than other types of infections. The best chance at overcoming these obstacles is a rapid and persistent dosage of an effective anti-fungal medication.
Identification & Treatment
In an analysis of the identification and treatment of Fusarium keratitis, the recent increase in cases has primarily confirmed our standard of care, with an emphasis on early identification. This hinges on a high index of suspicion; keep in mind that there is no such thing as a rare disease, only a disease looked for rarely. To that end, eye care practitioners' heightened awareness of this disease will aid early diagnosis and limit the progression of future cases. The later the diagnosis, the greater the possibility for the disease to become more difficult to control without sequelae, particularly considering Fusarium's tendency to move deeper into the cornea to penetrate Descemet's membrane.
A fungal ulcer can sometimes appear similar to bacterial keratitis in initial presentation. Early signs and symptoms include redness and irritation, which can precede a visible infiltrate by several days. Tearing, discharge, photophobia, decrease in visual acuity and anterior chamber reaction can also occur with fungal keratitis. The infiltrate can vary in morphological features: either a central or peripheral location is possible, as is a deep stromal infiltrate beneath the epithelium. Hypopyon may be present, though typically less so than in bacterial keratitis.
In obtaining a culture, care must be taken to scrape thoroughly and penetrate deeply enough, beyond any superficial epithelial healing, to the location of the infection. Culturing of lenses, lens cases and the tips and caps of lens solution containers will also provide useful information regarding the presence of fungus and its possible reservoir leading to its contamination of the eye. One retrospective study found lens case contamination accompanied Fusarium keratitis in all patients for whom lens case culture results were available.2
A topical ophthalmic antifungal, such as natamycin ophthalmic solution (Natacyn, Alcon), is the treatment of choice, often coupled with repeated corneal scrapings to assure tissue penetration of the drug.3
Origins of the 'Perfect Storm'
Experts now think that the recent Fusarium outbreak was the result of a confluence of several different factors that created a perfect environment for infection.
Contributing problems included the combination of ingredients in the MoistureLoc lens-care system, including a new disinfectant called alexidine and polymers that worked against this disinfectant by coating Fusarium and protecting it from eradication. The polymer film surrounding the fungus may have allowed it to persist in otherwise inhospitable environments, such as the disinfectant-containing solution, lens-solution bottles or bottle caps. In addition, Bausch & Lomb has indicated that this chemical interaction was compounded by poor lens hygiene practices by some contact lens wearers, such as topping the solution in lens cases rather than entirely emptying and refilling them, not changing solution on a daily basis and inadequate cleaning and replacement schedules for lens cases.
Water evaporation, in a situation where the solution is allowed to sit for prolonged periods of time, may have allowed for increased concentrations of the polymers, coating of the fungus, and an increased likelihood of that fungus persisting in solution and potentially reaching the eye by way of the contact lens.
Interestingly, increases in Fusarium's overall prevalence and shifts in the distribution of pathological fungi may add another layer of clouds to this perfect storm.
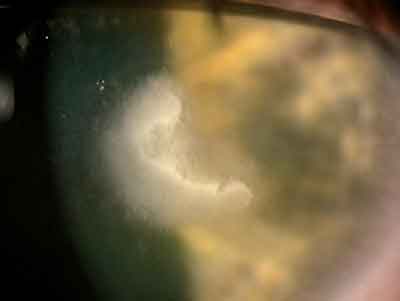 |
| The incidence of Fusarium infections appears to be increasing. Ron Melton, OD, and Randall Thomas, OD, MPH |
Research analyzing ocular fungal infections in China from 1989 to 2000 indicates a shifting trend in the types of fungus implicated in ocular infection. Fusarium infections increased from 53.6 percent of cases between 1989 and 1994 to 60.2 percent from 1995 to 2000. Concurrently, the percentage of Aspergillus decreased from 22.3 percent to 15.1 percent during the same time periods.4 A study of the spectrum of fungi in ocular disease at Wills Eye Hospital in Philadelphia analyzed data from before the current outbreak (1991 to 1999) and found Fusarium was the most commonly implicated pathologic fungus, a change from prior studies in non-tropical regions.
Hygiene & Lens Care
Lens-care hygiene, coupled with the chemical interactions occurring in the solution, increased these individuals' susceptibility to infection and can be implicated as part of the problem in the blossoming amount of Fusarium keratitis cases. As practitioners, we must take care not to blame the patient; clearly, infections result from numerous contributing factors. Instead, we must emphasize the positive steps individuals can take to minimize risk. Lens-care hygiene is perhaps the most readily improvable part of the equation leading to microbial keratitis. Habits including overnight lens wear as well as infrequent lens cleaning are under scrutiny, and some are even rethinking the safety of multipurpose cleaning solutions.
Good hygiene practices require patient education and adherence. Take measures to ensure thorough, proper patient instruction on lens care, cleaning regimens and hygiene. This may even include a reminder system of contacting new contact lens wearers. This contact could be by telephone or mail, or by the use of a diary to be checked at a follow-up visit, similar to those used in clinical trials to document compliance, to give patients a sense of accountability and ensure they continue to carry out the good lens-care practices learned in the office.
Maintaining close contact with lens wearers over the long term continues to be important also, and this can be an opportunity to check on lens-care practices, and jolt patients out of poor habits they may have fallen into between visits. Equally important is instruction to patients not to delay seeking medical care as quickly and early as possible in the event of a possible infection.
The Future of Lens Care
Though the explanation of several contributing factors appears plausible, some questions remain, including why other regions of the globe receiving the MoistureLoc solutions did not also experience similar outbreaks and why Fusarium has also been found in other contact lens solutions.
An absolutely definitive answer to the precise cause of the Fusarium keratitis outbreak may never be found. In fact, epidemiologists do not speak in terms of cause and effect, but rather contributing factors and increased risk. However, without question, the Fusarium outbreak highlights the importance of a global reporting network that would help catch an outbreak as it begins.
The rarity of Fusarium keratitis meant that small increases in its occurrence were sometimes not considered noteworthy in just one office, city or region. However, these minute changes can add up to something more substantial, and awareness of them may come earlier in the future if a wider pool of data is examined.
|
A second aspect of the problem is having accurate baseline levels of incidence to which we can refer. Our ability to detect changes in occurrence of a given disease relies upon the known, historical level of cases. Several such studies of Fusarium keratitis have been conducted to determine how frequently its incidence is connected to contact lens wear. For example, Miami's Bascom Palmer Eye Institute noted that 27 percent of Fusarium keratitis cases were connected to contact lens wear (eight of 30 cases). However in 2005, this percentage increased to 50 percent (18 of 36 cases), and jumped to 82 percent in the first three months of 2006.
The recent Fusarium outbreak suggests that numerous variables converged to create a perfect storm with damaging effects. The fact remains that more cases of Fusarium are out there, and all those risk factors could collide again. We never know when a disease that's considered nearly non-existent or thought to be a problem only on distant shores may suddenly appear in our own backyard.
Dr. Abelson, an associate clinical professor of ophthalmology at Harvard Medical School and senior clinical scientist at Schepens Eye Research Institute, consults in ophthalmic pharmaceuticals.
Ms. Fink is a medical writer with ORA Clinical Research & Development in North Andover.
1. Doczi I, Gyetvai T, Kredics L, Nagy E. Involvement of Fusarium spp. in fungal keratitis. Clin Microbiol Infect 2004;10:9:773-6.
2. Alfonso E, Cantu-Dibildox J, Munir W, et al. Insurgence of fusarium keratitis associated with contact lens wear. Arch Ophthalmol 2006;124:7: 941-947.
3. Thomas PA. Fungal infections of the cornea. Eye 2003;17:8:852-62.
4. Sun XG, Zhang Y, Li R, Wang ZQ, et al. Etiological analysis on ocular fungal infection in the period of 1989-2000. Chin Med J 2004;117:4:598-600.
5. Tanure MA, Cohen EJ, Sudesh S, et al. Spectrum of fungal keratitis at Wills Eye hospital, Philadelphia Pennsylvania. Cornea 2000;19:3:307-12.



