Today, most glaucoma treatment focuses on reducing intraocular pressure. We know, however, that glaucoma is a complex disease that has been related to numerous causes and may eventually be treatable in multiple ways (such as via neuroprotection).
One potential avenue for glaucoma treatment and prevention is nutrition. Though data is limited at this point, there is evidence that nutritional factors, including the presence of antioxidants, can have a significant effect on the development of eye diseases.1–5 Recently, two studies have produced new data that suggests a connection between diet and glaucoma progression.
The Fruit and Vegetable Factor
Both of the recent studies drew their patient data from the cohort of women (aged 65 and older) who participated in the Study of Osteoporotic Fractures, a multicenter longitudinal study designed to follow women enrolled at clinics around the United States to see what factors might be associated with these injuries.6,7 The SOF study design included monitoring diet, exercise and quality of vision, all of which can influence the rate of osteoporotic fractures.
Anne L. Coleman, MD, PhD, professor of ophthalmology in the Jules Stein Eye Institute of the David Geffen School of Medicine at the University of California Los Angeles and professor of epidemiology in the UCLA School of Public Health, was lead author of one study that was recently published in the American Journal of Ophthalmology.8 The object of her study was to see whether specific nutrients might account for an apparent association between glaucoma risk and fruit and vegetable consumption, and to investigate potential links between glaucoma risk and antioxidants, calories, fat, protein, and carbohydrates obtained from natural food sources.
Dr. Coleman's interest in this subject was sparked, in part, by data from the Age-Related Eye Disease Study showing a link between nutrition and age-related macular degeneration. She also was inspired by data from an earlier study that suggested that vitamin E might be influencing the progression of glaucoma—even though the authors of that study chose not to claim that their data demonstrated such a link.9 "That data gave me the impetus to pursue this with a different group of subjects," she says.
In fact, her study found much stronger associations between nutrition and glaucoma than the earlier study. She notes that this could be explained in part by differences between the two studies, such as an older-aged, all-female sample in Dr. Coleman's study, and the earlier study's reliance on a subject's self-report that he or she had glaucoma. Her study analyzed data from 1,155 women, of whom 8.2 percent (95 women) were diagnosed with glaucoma. Participants' consumption of fruits and vegetables was assessed using the Block Food Frequency Questionnaire. The data showed:
• Glaucoma risk was decreased 69 percent in women who consumed at least one serving per month of green collards and kale compared with those who consumed fewer than one serving per month.
• Glaucoma risk was decreased 64 percent in women who consumed more than two servings per week of carrots compared with those who consumed fewer than one serving per week.
• Glaucoma risk was decreased 47 percent in women who consumed at least one serving per week of canned or dried peaches compared with those who consumed fewer than one serving per month.
Dr. Coleman is quick to point out the limitations of her study. "We used a cross-sectional sample, which means we can't be sure which came first: the different diet or the disease," she notes. "It's possible that people changed their diet to include more fruits and vegetables after they were told they had glaucoma. However, some of the women in our database who had glaucoma were unaware of it before our study, making that scenario less likely.
"It's also possible that people who tend to eat fruits and vegetables have a healthier lifestyle," she continues. "They may tend to exercise more, and cardiovascular exercise is beneficial for lowering eye pressure. That's why our study looked at individual nutrients as well." Dr. Coleman also notes that her study didn't control for socioeconomic status. "People with a higher socioeconomic status probably eat a greater variety of fruits and vegetables, which can be expensive," she says. "And how does intraocular pressure affect this potential connection? If your pressure is 40 mmHg, eating all the fruits and vegetables in the world may not prevent damage to your optic nerve. That could even be true with a pressure in the mid-20s. With so many factors that could interact, it's difficult to sort out.
"In any case," she concludes, "studies like mine need confirmation via large-scale, randomized, prospective studies."
Focusing on African Americans
A second nutrition-related study that also drew data from the Study of Osteoporotic Fractures was conducted by JoAnn A. Giaconi, MD, assistant clinical professor of ophthalmology at the Jules Stein Eye Institute at UCLA. Like Dr. Coleman, Dr. Giaconi was intrigued by data from studies such as AREDS. "Other studies have also shown that oxidative stress damages retinal ganglion cells in vitro, and that antioxidants, added in vitro, can prevent some of that damage," she notes. "We wanted to see if we could find a connection between nutrition and glaucoma at the clinical level." Her father, a cardiologist, always adjusted the family's diet in response to nutrition studies when she was growing up, contributing to her curiosity about the connections between diet and health.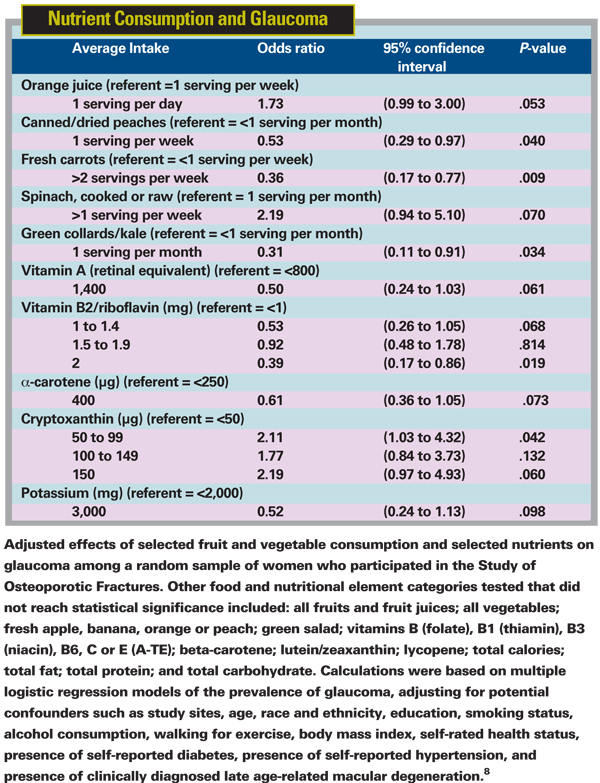
Dr. Giaconi explains that Dr. Coleman's random sample taken from the study of osteoporotic fractures included a small number of African-American women. It turned out that some of the connections between glaucoma and diet seemed stronger in that subgroup. Consequently, Dr. Giaconi decided to examine the data from all of the eligible African-American women in the osteoporosis study. "Glaucoma affects African Americans disproportionately," she points out. "They have more glaucoma, it's a lot more severe at the time of diagnosis, and they're much more likely to go blind from it. Also, we know that some systemic hypertension medications seem to work better in blacks than in whites, so this seemed like a potentially valuable avenue to explore."
Dr. Giaconi's data included 584 black women; 13 percent (77 women) had glaucoma in at least one eye. [Giaconi JA, et al. IOVS 2008;49; ARVO E-abstract 5453]. The data showed:
• Three or more servings per day of all fruits or fruit juices decreased the odds of glaucoma by 79 percent compared to consuming less than one serving per day.
• Eating more than two servings per week of fresh oranges and peaches was associated with less glaucoma risk.
• Eating more than one serving per week of green collards or kale decreased the odds of glaucoma by 57 percent compared to 1 serving per month or less.
• There was a protective trend for glaucoma in those eating more fruit or fruit juices (p=0.029), fresh oranges (p=0.012), fresh peaches (p=0.002), spinach (p=0.041), and green collards or kale (p=0.006).
• Higher intakes of some nutrients were also associated with decreased risk: vitamin A (p=0.015); folate (p=0.049); a-carotene (p=0.022); ß-carotene (p=0.038); and lutein/zeaxanthin (p=0.041).
Dr. Giaconi notes that it's dangerous to draw too many conclusions from the nutrition-related data that has been found so far. "My study was an exploratory study," she says. "The data clearly show associations, but we can't say for sure that the difference in diet caused the difference in glaucoma risk. Did eating more collard greens reduce the likelihood of developing glaucoma, or is there something else about the individuals who eat more collard greens that makes them less likely to develop glaucoma? Maybe those individuals exercise more. Maybe they grew up in a different environment. Maybe they metabolize nutrients differently. We can't claim that the association is causal, but I believe the association is worth pursuing further."
Contradictory Results
Interestingly, some of the associations found in Dr. Giaconi's study and Dr. Coleman's studies disagreed. For example, Dr. Giaconi's data indicated that in her sample of African-American women, eating more than two servings per week of fresh oranges was associated with lowered glaucoma risk, as was eating more spinach. In contrast, Dr. Coleman's study found an increased risk of glaucoma associated with consumption of orange juice (statistically significant) and fresh oranges or spinach (not statistically significant).
Asked about this, Dr. Coleman notes that the studies based their data on very different samples, even though they were taken from the same cohort. "Dr. Giaconi's sample was 100-percent African-American women; ours was largely Caucasian," she says. "Of course, it's unclear whether ethnicity accounts for the different associations that turned up. And if the differences are real, are they genetic, environmental or cultural?"
"Many factors could be influencing these outcomes," agrees Dr. Giaconi. "Dr. Coleman has noted that people who drink a lot of orange juice might be taking more medications and therefore sicker people at baseline. Or the orange juice difference could be an aberrant statistical anomaly. It's certainly not conclusive, and it would be a mistake to scare people away from drinking orange juice because of this one piece of data."
Dr. Coleman says it is possible that the associations that were found in both studies might apply to most women, regardless of race. "But that's a big assumption, and you need to use caution," she adds. "For example, suppose there's a gene associated with an increased risk of glaucoma, and this gene doesn't activate if a person eats more kale. If a woman doesn't have that particular gene, eating kale might be a waste of time for her as regards her risk of glaucoma. This is all speculation, and points to the need for more research."
Dr. Giaconi also notes that the way food is prepared may confound the issue even further. "For example, the carotenoids, which are vitamin-A derivatives found in tomatoes and squash and other bright red or orange vegetables, are much more easily absorbed by the body once the food is crushed and cooked in oil," she explains. "Uncooked, the nutrients are tightly bound to the plant matter. Cooking in oil frees them up for easier digestion. Our two studies found opposite trends associated with eating carrots; perhaps one group tends to cook carrots while the other prefers them raw."
Talking to Patients
Although a connection between glaucoma and nutrition seems likely given these results, Drs. Coleman and Giaconi are cautious about making recommendations to patients. Dr. Coleman says she simply recommends that her patients eat more fruits and vegetables. "Doing so may indeed be protective for glaucoma, but it's definitely protective for the heart and helps to prevent cancer and other diseases," she notes. "I think all physicians should recommend that their patients live healthier lifestyles. You never know what will motivate a patient to actually make positive changes. If concerns about heart disease or cancer don't do it, maybe the possibility of avoiding glaucoma will. It's also possible that no clinician has ever advised them to eat fruits and vegetables because they have no risk factors for heart disease, for instance.
"On the other hand, it's too early to recommend eating or avoiding specific foods or nutrients," she says. "Our study found a slightly negative association between glaucoma and eating spinach, but spinach is good for macular degeneration. So I'm not going to tell a patient to avoid spinach."
Dr. Giaconi believes there's nothing wrong with suggesting that patients change their diet, as long as no claims are made about preventing glaucoma as a result. "When glaucoma patients ask me whether there's anything else they can do to help their glaucoma, I tell them to come to their follow-up visits and take their medications every day, but I also mention that a diet full of fruits and vegetables is a good thing," she says. "Even if it doesn't improve your vision or stop the glaucoma, there are a lot of other benefits, such as for your heart, and potentially positive effects for patients with diabetes or cancer. A better diet should improve the health of the blood vessels, and they nourish the optic nerve, so this kind of dietary change certainly isn't going to hurt."
Dr. Giaconi notes that patients see supplements in the store—many on the market because of the AREDS data—and wonder whether they should be taking them to help with their glaucoma. "I tell them I think they're better off getting the right nutrition through their diets," she says. "Supplements cost money, and there's no proven benefit for glaucoma."
What's Next?
Drs. Coleman and Giaconi are both working on follow-up studies. "We're looking at the blood levels of vitamins and antioxidants in patients with and without glaucoma," says Dr. Coleman. "This is another association study; we want to see whether people who say they aren't taking vitamins show a difference in nutrient blood levels compared to those who say they are.
"For example," she continues, "we're trying to confirm associations such as those that seem to exist between glaucoma and higher levels of cryptoxanthin or vitamin C, or lower levels of riboflavin. Such a finding would provide some support for recommending specific nutrients in a patient's diet.
"Unfortunately, blood levels don't always correlate with what a person is eating, for many possible reasons," she notes. "The nutrients may be metabolized quickly or be unstable, they may not reside in the blood serum that you're testing, or the nutrient in question may be gone from the food by the time the food is consumed. Riboflavin, for example, is often added to food products, but light can cause it to break down. So it's possible that the nutrient isn't even making it into the body. Of course, even if the associations are confirmed, we'll still need to follow up with a randomized trial."
Dr. Giaconi says she'd like to examine the dietary impact of other foods monitored in the osteoporosis study, such as berries. "Some of these contain high levels of flavenoids and other potentially beneficial components," she observes. (She adds that an excellent source of information about nutrients and their impact on health can be found at the Linus Pauling Institute's
"All of these studies are still exploratory," she says. "We're still in the early stages of this research. But right now the public has a huge level of interest in eating better and finding ways to take fewer medications. Improving your eye health through diet is relatively inexpensive, and being able to do so would benefit both individuals and the health-care system in this country and around the world. And of course, if we can show that diet really can slow down or prevent glaucoma progression, far fewer people will lose their vision."
1. Veach J. Functional dichotomy: glutathione and vitamin E in homeostasis relevant to primary open-angle glaucoma. Br J Nutr 2004;91:809–829.
2. Maher P, Hanneken A. Flavonoids protect retinal ganglion cells from ischemia in vitro. Exp Eye Res 2008;86: 366–374.
3. Lucius R, Sievers J. Postnatal retinal ganglion cells in vitro: protection against reactive oxygen species (ROS)-induced axonal degeneration by cocultured astrocytes. Brain Res 1996;16:56–62.
4. West AL, Oren GA, Moroi SE. Evidence for the use of nutritional supplements and herbal medicines in common eye diseases. Am J Ophthalmol 2006;141:157–166.
5. Robert R. Neuroprotection: Is it already applicable to glaucoma therapy? Curr Opin Ophthalmol 2000;11:78–84.
6. Cummings SR, Nevitt MC, Browner WS, et al. Risk factors for hip fracture in white women. Study of Osteoporotic Fractures Research Group. N Engl J Med 1995;332:767–773.
7. Cauley JA, Lui LY, Ensrud KE, et al. Bone mineral density and the risk of incident nonspinal fractures in black and white women. JAMA 2005;293:2102–2108.
8. Coleman AL, Stone KL, Kodjebacheva G, Yu F, Pedula KL, Ensrud KE, Cauley JA, Hochberg MC, Topouzis F, Badala F, Mangione C ; Study of Osteoporotic Fractures Research Group. Glaucoma Risk and the Consumption of Fruits and Vegetables Among Older Women in the Study of Osteoporotic Fractures. Am J Ophthalmol 2008;145:1081–1089.
9. Kang JH, Pasquale LR, Willett W, et al. Antioxidant intake and primary open-angle glaucoma: a prospective study. Am J Epidemiol 2003;158:337–346.



