One of the most serious complica-tions after glaucoma filtering surgery is infection. The presence of a filtering bleb poses a continuing risk of infection over a patient's lifetime.1-5 It is critical to be able to differentiate between blebitis and bleb-associated endophthalmitis because of differences in initial management, treatment and prognosis.
Blebitis describes a distinct clinical entity consisting of an isolated bleb infection with varying degrees of anterior segment inflammation, without vitreous involvement.1 It may represent a limited form or early stage of endophthalmitis.1 The progression of blebitis into endophthalmitis has been documented.6-7 Blebitis and endophthalmitis may thus represent a continuum of infection and this distinction has become an increasingly common management problem for ophthalmologists.8
The incidence of isolated blebitis is not well known. A retrospective study of 239 eyes reported an episode of blebitis in 2 percent with average follow-up of 2.7 years (range, 0.3 to 7.3).2 The study demonstrated significant morbidity related to trabeculectomy with mitomycin. In the series, one of every 100 patients developed endophthalmitis each year and 4 percent of patients developed a bleb-related complication consisting of a bleb leak, blebitis or endophthalmitis. The study reported that the incidence of the above bleb-related complications continues at a fairly constant rate over time. At five years, up to 23 percent of patients who have undergone trabeculectomy with mitomycin might develop one of these complications.2
 |
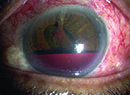
| A patient with blebitis illustrating the classic "white on red" appearance. A small hypopyon is present but there is an absence of vitreous cells,differentiating this from endophthalmitis. |
Presentation
Prodromal signs and symptoms have been identified days or weeks before the diagnosis of blebitis or endophthalmitis is made. These include browache, headache, external eye inflammation or infection such as blepharitis or conjunctivitis.7 One must always maintain a high index of suspicion and pay careful attention to any complaints in patients who have undergone trabeculectomy.
Patients with blebitis generally present with symptoms of redness, photophobia, tearing, pain, blurry vision, discharge, lid swelling, irritation and/or itching. In a small series of blebitis, patients had been symptomatic for one to four days (median, two days).12 On exam, eyes have the typical "white on red" appearance, which is an opalescent bleb (milky, white translucent appearance due to a mucopurulent infiltrate or hypopyon within the bleb) against a background of diffuse conjunctival injection.13 Anterior chamber reaction is variable, ranging from a quiet anterior chamber to the presence of keratic precipitates or a frank hypopyon. In a retrospective review of 12 eyes with blebitis, anterior chamber reaction varied from no reaction to 0.5-mm hypopyon.12 Most importantly, the vitreous is clear. Seidel testing is often positive.
In contrast, patients with endophthalmitis have more rapidly progressive presentations, often with worsening pain, redness and decreasing visual acuity over a period of hours.6,13 Endophthalmitis can occur years after the initial filtering surgery. The defining feature of endophthalmitis is the presence of vitritis.
Risk Factors
Risk factors for bleb-related infections may include the use of antifibrotic agents in conjunction with filtering surgery. The use of 5-fluorouracil and mitomycin-C has increased the success rate of trabeculectomy, however it leads to thinner, cystic and avascular blebs, which may be more susceptible to the transconjunctival migration of bacteria through the bleb.6
 |
| Figure 2. This patient with blebitis presented two years after trabeculectomy with a history of redness, itching and discharge in the affected eye for two days. Her vision was unchanged and she was noted to have a bleb leak on examination. Note the inferior location of the bleb, which carries a greater risk of bleb-associated infection. |
Late-onset bleb leaks are a significant risk factor for bleb-related infection.4 Seidel testing should be performed on all ischemic, thin-walled blebs and patients who are noted to have lower than previous intraocular pressures. In a retrospective review of 12 eyes with blebitis, the mean intraocular pressure at the time of diagnosis was significantly lower than preinfection IOP (7.3 ± 5 mmHg vs. 11.2 ± 3.5 mmHg).12
The true incidence of bleb leaks is difficult to determine since they are often asymptomatic. Since late-onset bleb leaks are a significant risk factor for infection, closure of the leaks may be warranted in selected cases.4
Other risk factors that have been identified include inferior bleb location, recurrent bacterial conjunctivitis, severe blepharitis, dry eye, younger age,2 the use of releasable sutures,17 and combined trabeculectomy and phacoemulsification.18 Contact lens use may also increase the risk of infection.
In a case-control study of 23 patients with bleb-associated endophthalmitis and 69 controls, 26 percent had a previous episode of blebitis. The mean time interval between the treated episode of blebitis and the subsequent development of endophthalmitis was nine weeks.5 Thus it is important to follow patients who have had blebitis closely after the resolution of the blebitis since they are still at significant risk of developing bleb-associated endophthalmitis. Diabetes mellitus was also statistically significantly associated with endophthalmitis in this study.
Treatment
Outpatient treatment of blebitis has been shown to be efficacious.12 The patient should be observed in the office for several hours to reassess the anterior chamber reaction and ensure the absence of vitreous involvement. In addition, if the patient is unable to instill the drops at the required frequency or follow-up is in question, he should be hospitalized. The patient must be instructed to return to the office if, despite treatment, symptoms worsen at home. The clinician must evaluate the patient's ability to adequately self-treat at home and weigh this against the possibility of a poor outcome without aggressive therapy. Hospitalization should be considered in select cases.
Aggressive treatment of blebitis affords a much better prognosis for visual recovery. In a retrospective study,1 14 patients developed a bleb infection one month to 22 years after trabeculectomy. All patients received hourly topical therapy which consisted of fortified gentamicin sulfate (15 mg) and fortified cefazolin sodium (50 mg/ml). Patients were hospitalized and alternating drops were instilled every 30 minutes for the first 24 hours. Intravenous antibiotics were also given to the majority of patients.
With the advent of fluoroquinolones, a more recent survey of the American Glaucoma Society members reported that 51 percent use fluoroquinolones alone in the initial management of isolated blebitis. Twenty-three percent used fluoroquinolones in combination with one or two other topical antibiotics such as a trimethoprim-polymixin combination or aminoglycoside. Ten percent of responding glaucoma specialists used a fluoroquinolone in conjunction with a fortified antibiotic such as an aminoglycoside, vancomycin or cephalosporin.
Most treat on an outpatient basis with only 6 percent routinely using an oral antibiotic for blebitis. Topical corticosteroids are used by 62 percent once improvement of the blebitis is noted or once topical antibiotic therapy is well-established. There is no consensus regarding obtaining conjunctival cultures at initial diagnosis of blebitis.8 Even among glaucoma specialists, management of blebitis varies and it is important to evaluate each case on an individual basis. When in doubt, it is better to treat more aggressively than not enough given the potentially devastating outcome.
Cases in which the vitreous is not well-visualized or in which the diagnosis of isolated blebitis is in doubt should be treated for potential endophthalmitis. Patients with presumed endophthalmitis should be promptly referred to our retina colleagues for appropriate treatment, which may include vitrectomy and intravitreal and subconjunctival injection of antibiotics in addition to topical therapy. Due to the different pathogenesis and organisms involved in post-trabeculectomy endophthalmitis, it is important not to extrapolate the results of the Endophthalmitis Vitrectomy study to these patients.6
Outcomes
Blebitis has a good prognosis, with return to preinfection visual acuity and intraocular pressure in most cases.6,13 Blebitis typically responds to therapy within 24 to 48 hours, both clinically and symptomatically.12 Most patients in one study noted a marked improvement in pain with rapidly improving anterior chamber reaction and conjunctival injection within 24 to 48 hours of the initiation of therapy.1 In contrast, the majority of patients with bleb-associated endophthalmitis lose four or more lines of visual acuity. In a retrospective study of 33 patients with bleb-associated endophthalmitis who underwent pars plana vitrectomy and intravitreal antibiotics, the visual outcome in the majority of cases was in the count fingers to light perception range.6
Bleb-related infection is a serious complication of glaucoma filtering surgery. It can be associated with filtration failure and loss of visual acuity. The clinical outcome is dependent upon early detection and aggressive treatment. Clinicians should alert their patients to the signs and symptoms of infection and they should be instructed to contact the clinician immediately if they develop any redness, irritation, pain, brow ache, discharge or visual disturbance in the affected eye.
Patients with bleb leaks must be followed closely since bleb leakage is a significant risk factor for infection, with consideration of surgical revision in late, chronic or recurrent bleb leaks. Blebitis is differentiated from bleb-associated endophthalmitis by the lack of vitreous involvement.
Once the diagnosis of blebitis is made, aggressive therapy and close observation are imperative since progression to fulminant endophthalmitis is possible. Blebitis usually responds to topical and/or subconjunctival antibiotics, without the need for intravitreal injections.15 One treatment approach for blebitis might be the use of an hourly topical fluoroquinolone with a second fortified antibiotic in more severe cases or for those at higher risk (such as history of recurrent bleb-associated infections or monocular status). Topical steroids may be instituted cautiously once the blebitis shows clear improvement in order to aid in preservation of bleb function.
Close observation of patients with blebitis for the development of vitritis is critical. Patients should be closely followed even after resolution of the blebitis since a prior episode of treated blebitis places the patient at increased risk for bleb-associated endophthalmitis.5 In addition, progression from blebitis to culture-positive endophthalmitis has been documented in the literature.6-7 This supports the position that blebitis may be a precursor to endophthalmitis, thus representing a continuum of the disease process. If bleb-associated endophthalmitis is suspected, prompt referral to a retina specialist is recommended for a possible vitrectomy and intravitreal antibiotics.
In a survey of glaucoma specialist members of the AGS, respondents would often treat blebitis as a potential case of endophthalmitis, especially in cases of severe anterior chamber reaction including fibrin. This is not surprising given the potentially devastating effects of endophthalmitis.8 It is critically important to educate patients of the lifelong risk of infection associated with trabeculectomy. A high index of suspicion and attention to the early signs and symptoms of bleb-related infections can help prevent the potentially devastating consequences of a delayed diagnosis of bleb-associated infection.
Dr. Grewal, a fellowship trained glaucoma specialist, is in private practice.
1. Brown RH, Yang LH, Walker SD, et al. Treatment of bleb infection after glaucoma surgery. Arch Ophthalmol 1994;112:57-61.
2. DeBry PW, Perkins TW, Heatley G, et al. Incidence of late-onset bleb-related complications following trabeculectomy with mitomycin. Arch Ophthalmol 2002; 120:297-300.
3. Mochizuki K, Jikihara S, Ando Y, et al. Incidence of delayed onset infection after trabeculectomy with adjunctive mitomycin C or 5-fluorouracil treatment. Br J Ophthalmol 1997;81:877-883.
4. Soltau JB, Rothman RF, Budenz DL et al. Risk factors for glaucoma filtering bleb infections. Arch Ophthalmol 2000;118:338-342.
5. Lehmann OJ, Bunce C, Matheson MM, et al. Risk factors for development of post-trabeculectomy endophthalmitis. Br J Ophthalmol 2000;84:1349-1353.
6. Ciulla TA, Beck AD, Topping TM, et al. Blebitis, early endophthalmitis, and late endophthalmitis after glaucoma-filtering surgery. Ophthalmology 1997; 104:986-995.
7. Poulsen EJ and Allingham RR. Characteristics and risk factors of infections after glaucoma filtering surgery. J of Glaucoma 2000;9:438-443.
8. Reynolds AC, Skuta GL, Monlux R, et al. Management of blebitis by members of the American Glaucoma Society: a survey. J of Glaucoma 2001;10:340-347.
9. Kattan HM, Flynn HW Jr, Pflugfelder SC, et al. Nosocomial endophthalmitis survey. Current incidence of infection after intraocular surgery. Ophthalmology 1991;98:227-238.
10. Greenfield DS, Suner IJ, Miller MP, et al. Endophthalmitis after filtering surgery with mitomycin C. Arch Ophthalmol 1996;114:943-949.
11. Higginbotham EJ, Stevens RK, Musch DC, et al. Bleb-related endophthalmitis after trabeculectomy with mitomycin C. Ophthalmology 1996;103:650-656.
12. Chen PP, Gedde SJ, Budenz DL, et al. Outpatient treatment of bleb infection. Arch Ophthalmol 1997; 115:1124-1128.
13. Ayyala RS, Bellows AR, Thomas JV, et al. Bleb infections: clinically different courses of "blebitis" and endophthalmitis. Ophthalmic Surg and Lasers 1997; 28:452-460.
14. Ormerod LD, Becker LE, Cruise RJ, et al. Endophthalmitis caused by the coagulase-negative staphylococci. 1. Disease spectrum and outcome. Ophthalmology 1993;100:715-723.
15. Kangas TA, Greenfield DS, Flynn HW Jr, et al. Delayed-onset endophthalmitis associated with conjunctival filtering blebs. Ophthalmology 1997;104:746-752.
16. Katz LJ, Cantor LB, Spaeth GL. Complications of surgery in glaucoma: early and late bacterial endophthalmitis following glaucoma filtering surgery. Ophthalmology 1985;92:959-963.
17. Burchfield JC, Kolker AE, Cook SG. Endophthalmitis following trabeculectomy with releasable sutures [letter]. Arch Ophthalmol 1997;114:766.
18. Belyea DA, Dan JA, Lieberman MF, et al. Midterm follow-up results of combined phacoemulsification, lens implantation, and mitomycin-C trabeculectomy procedure. J Glaucoma 1997;6:90-98.