Once a device gets out of the laboratory and into surgeons' offices, it may work differently than expected. In some ways it will be better, while in others it may be less effective. After working with the Pulsion FS femtosecond laser (Intralase, Irvine, Calif.) for the past six months, I've gotten to know its nuances. And, though it may not be perfect in all areas of LASIK flap making, if I had to do it all over again I'd still choose to use it. Here are the pros and cons of this relatively new device.
Making the Cut
Basically, the Pulsion uses a femtosecond laser, instead of a keratome, to make a flap.
To use the laser to make the incision, I first program it with the desired flap diameter and depth. The maximum diameter you can program is 9.5 mm, though the company recommends 9.2 mm. I use a 9.4-mm flap.
I mark the center of the patient's visual axis with a Sinskey hook and gentian violet and place a suction ring on the eye. My assistant activates the suction.
On the computer screen, there's a small white circle in the center that represents the center of the applanation plate. I center the yellow crosshairs directly over the gentian violet mark. I can then make small adjustments with the computer to make sure I'm aligned on the visual axis. I then dock a cone that's attached to the laser onto the ring to achieve applanation and begin making the flap. As the flap is created, bubbles form across the cornea, allowing me to track the laser's progress. When the interface cut is finished, the laser makes the side cut, leaving a hinge and creating the flap.
 |
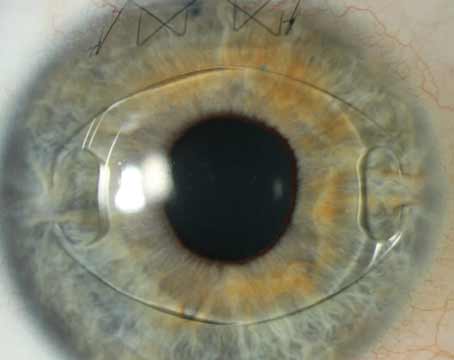
| The flap edge may be visible post-LASIK, but the flap itself is very adherent. |
It's also possible for air to come up through the epithelium in a very shallow flap that can lead you to abort the case and return later. It doesn't cause harm to the visual axis, though.
Clinical Impressions
Overall, the learning curve is about 300 cases. The main challenges in cresting this curve include recognizing when you should abort versus when you should just stop and restart, such as when you break suction.
Fortunately, after using the Intralase for 800 cases over the past six months, buttonhole flaps and abrasions have ceased being the concerns they were with our previous microkeratome. I can also treat corneas with basement membrane dystrophy and can make thinner flaps for patients with high refractive errors, in whom I need as much corneal tissue as possible. It's also easier to center the flap on the visual axis than it was with the microkeratome, and I have flexibility in where I put the hinge. The hinge can be placed superiorly, nasally or temporally.
• What could be improved. From a clinical point of view, using the Pulsion increases the length of my cases. With our previous microkeratome, we could do 10-12 cases per hour, now we do five or six. It's also important to keep in mind that you're working with two lasers, so there's a risk that, if one goes down, you'll have to cancel all the day's surgeries.
There are also issues revolving around docking the laser cone with the suction ring, and getting very good centration can occasionally be challenging. Just as with a mechanical microkeratome, you have to have the suction ring centered as your first starting point. If that's not centered, then the flap is likely to be decentered, as well. The suction time has increased from about 25 seconds with our previous microkeratome to about 1 min. 45 sec.
 |
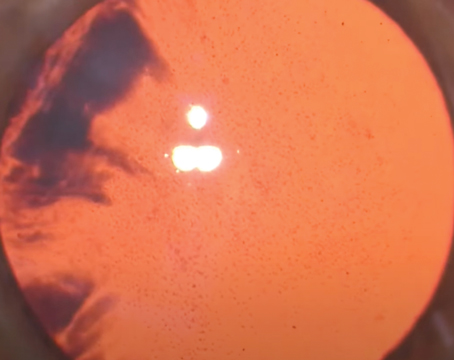
| By tracking the laser's progress, you can tell whether you have to abort and re-try. |
Aesthetically, some of my comanaging doctors have commented that they can see the edge of the flaps in Pulsion-flap patients, and that they don't like their appearance as much as microkeratome flaps. I, however, think the Intralase flaps are cosmetically acceptable. What's more, when I return to lift a flap for an enhancement, I've found these flaps to be even more adherent than those produced mechanically, which I think is beneficial in the long run.
• Handling enhancements. You have to be careful when making a flap with the Pulsion on patients who've previously had RK or LASIK. RK patients need an easy lift. If it's not gentle, you can tear the radial incisions as you peel the flap back. In LASIK patients, it's best to stay about 40 µm away from the interface, either shallower or deeper in the cornea.
Myths and Realities
Before the Pulsion came out, there was a lot of discussion about what it could and couldn't do. Now, as I approach 1,000 cases with it, I'm in a better position to weigh in on these claims. Here are some femtosecond myths, followed by the realities:
• "First morning acuities are blurrier than surgeries done with microkeratomes." We haven't found this to be true. We have as many 20/20 outcomes with the Pulsion as we did with our microkeratome.
• "The surface isn't as smooth as it is with a blade." I think that if your Pulsion is calibrated properly, you get just as good a surface as you do with a microkeratome.
• "The enhancement rate greatly decreases." I haven't really been doing it long enough to verify this. However, I can't see much difference in enhancement rates between the laser and the microkeratome.
• "Pachymetry isn't possible, due to the bubbles the laser creates in the interface." This isn't a problem. We place patients in another room until the interface bubbles that are created by the construction of the flap resolve. We can then bring them back and do a pachymetry reading both before and after we lift the flap without difficulty.
• "Flaps are always within ± 15 µm of the intended thickness." This isn't always the case. Though we program the laser to make a 100-µm flap, we have gotten flaps that range from 90 µm thick to 184 µm.
• "The 'manhole cover' sidewall of the flap will result in less flap slippage." Experience hasn't borne this out, because it's not the sidewall cut that holds the flap in position, but rather the endothelial pump. The flap isn't rigid enough for the sidewall cut to be a factor.
• "There's a much lower rise in intraocular pressure with the suction ring." Actually, our experience has been that the patient's vision goes black during the treatment, so the suction pressure must be exceeding the systolic pressure in the central retinal artery.
Ultimately, I have been pleased with the Pulsion. Even though it's not perfect, no technology is. As a LASIK surgeon, I find that it performs in the situations that count. I use a former patient, done with a mechanical microkeratome, as an example: This patient had a very small orbit, and when the microkeratome cut was made, she only had a 3-mm flap that bisected her pupil. This small flap caused problems that took a full year and a half to resolve. If I never see another too-small flap again, it will be worth using the Pulsion.
Dr. Wright is in private practice.