Rhein Medical introduces the new Brown Triple Post Speculum (Stainless Product # 8-08164, Titanium Product #05-7105), developed in coordination with Reay H. Brown, MD. The blade design prevents lashes from overlapping the drape, and the special central posts prevent lids and lashes from rotating into the surgical field. The special fenestrated blades improve exposure and access to superior surgical approaches by supporting and elevating the middle of the lids, the company says. The speculum improves assess and visualization of the superior cornea by creating an oval separation of the lids, preventing drape obstruction, and it is ideal for all anterior and posterior segment surgery. The instrument is reusable, autoclaveable, made in the 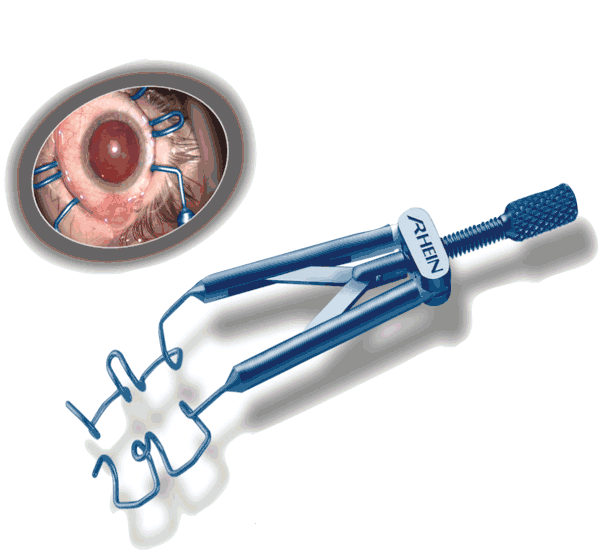
Ocusoft: Study Shows TetraVisc to Be A More Economical Alternative
Ocusoft reports that a recent company study comparing the topical anesthetic effects of its TetraVisc Forte, tetracaine hydrochloride 0.5%, and Akten, lidocaine hydrochloride 3.5% (Akorn), demonstrated the same anesthetic efficacy at a fraction of the cost.
Formulated with higher viscosity, TetraVisc Forte increases corneal contact time, im-proves pain levels in post-operative patients and is an affordable alternative to traditional ophthalmic anesthetics, the company says. Available in convenient multi-dose 5-mL dropper bottles and single unit-of-use 0.6-mL bottles, TetraVisc Forte increases efficiency in the operating room or the clinic. For information or a trial evaluation, call 1 (800) 233-5469 or visit ocusoft.com.
New Landolt C Chart for ETDRS
Landolt C optotype charts are acknowledged as one of the most reliable pediatric acuity tests. Results are comparable to the original Snellen and many more recently designed pediatric acuity optotype tests are measured against the Landolt C figures.
Richmond Products provides a family of four Landolt charts, offering a choice of near-point and distance versions. The distance Landolt C charts can be wall-mounted or used with various illuminated cabinet types.
For example, the new Landolt C chart (shown here) is used at 13 feet (4 meters) and is designed for use with any standard ETDRS cabinet or may be wall-hung. ETDRS Optotypes on this chart are positioned in 14 proportionally spaced, geometric progression lines. Line sizes range from 20/200 to 20/12.5 (6/60 to 6/3.7) and are labeled for Snellen equivalents at 20 feet and 4 meters, decimal, LogMar, actual size at 13 feet (4 meters) and letter size. Chart size is 24.5 x 25.5 inches (62w x 65 cm).
For information, call Richmond Products at (505) 275-2406 or visit richmondproducts.com.
New Functionalities in Eyemaginations Luma 1.3
Eyemaginations has re-leased the latestversion of its software for eye-care practitioners, LUMA version 1.3. The new version includes 12 new and enhanced ocular presentation topics including: Amblyopia Overview and Treatment Options; Blepharitis Overview; Retinal Vein Occlusion Overview; Fundus Photography Overview; HD Lenses; Lattice Degeneration Overview; Multifocal IOL (General); Multifocal IOL (Design I and II); Optical Coherence Tomography; and Wide Angle Retinal Imaging.
Version 1.3 also includes new functionalities, many of which were implemented based on client feedback:
• New anatomy perspectives within the Exam Advisor feature will enable the practitioner to use Blood Vessels, Visual Pathway and Head–Front View as different angles.
• To ease the user experience, the
• Lastly, the user now has more control of functionality within the Media Player. Enhanced video controls and closed captions serve to improve the patient's visual experience, the company reports.
For information, call 1 (877) 321-5481, e-mail info@eyemaginations.com or visit luma.eyemaginations.com.
Pearls from the Deep
Anita Nevyas-Wallace, MD
Protecting the Zonule Is Not Difficult And Is Well Worth the Trouble.
Avoiding traction on the zonule is desirable even when we believe the zonule to be robust, and is especially important when zonular abnormality is suspected, as in pseudoexfoliation. There are opportunities to protect (or damage) the zonule in each step of a cataract procedure:
• Starting capsulorhexis. Using a curved, very sharp cystotome allows puncture of the anterior capsule without pulling on the zonule, and it creates a triangular flap that is easy to grasp with capsulorhexis forceps. You can keep your cystotomes extra sharp by touching them up yourself with a fine sharpening stone.
• "Loosening" of the nucleus. A safe way to mobilize the nucleus is with hydrodissection of cortex from capsule; direct (non-dissection) techniques for loosening the nucleus stress the zonule. Aim the fluid stream upward at the inside surface of the anterior capsule. Once the nucleus spins freely, hydrodelineate between epinucleus and nucleus to create an epinuclear shell, which will protect the capsule during phacoemulsification.
• Pre-chopping. Avoid any pre-chop technique that uses the zonule for counter-traction. When the nucleus is so soft that the pre-chopper sinks in easily, its insertion does not stress the zonule. Otherwise, maneuver a sustainer behind the nucleus for counter-traction, or skip pre-chopping.
• During phacoemulsification. When you first enter the nucleus, to chop or to create a groove, be sure to use enough phaco power that there is no movement or depression of the lens-bag complex.
• During I/A. "Vacuuming" the capsule risks both zonular damage and capsular tearing. The stellate striae of the posterior capsule that appear when capsule is aspirated suggest that the zonule is being tugged as well. Even if the incarceration is corrected before the capsule actually tears, the brief traction on the zonule is sufficient to tear zonular fibers.
• To clean the capsule safely. Rely on irrigation rather than aspiration. Create a sideport for a chamber maintainer, in addition to the one you create for manipulation. Late in phacoemulsification, but before removal of the epinuclear shell, place a sandblasted anterior chamber maintainer hooked up to a second bottle. This provides surge protection and permits several useful maneuvers:
• At the start of I/A. While the assistant attaches the tubing to the I/A handpiece, use a 25-ga. cannula on a 3 cc syringe to "hydrodissect" between the cortex and the undersurface of the anterior capsule. Start subincisionally, then sweep nearly 360 degrees. Unlike peeling the cortex from the capsule by pulling on it with the I/A tip, this technique allows the attachment between cortex and capsule to be severed without using the zonule for counter-traction.
Once the cortex is well-loosened, use the cannula to aspirate it. Be sure that the syringe is not completely empty when you start to aspirate cortex, so that you will be able to create reflux if you need to.
• At the end of I/A. To clean the fornices of the bag, while the chamber maintainer is running, use a curved sandblasted 27-ga. cannula (Nevyas-Wallace Cortex Aspiration Cannula, Katena) to do two things. For safe removal of adherent cortical strands from the posterior capsule, direct a stream of cannula irrigation at the strands, and use the sandblasted part of the cannula to gently touch strands while irrigating. The idea is to liberate them, not to aspirate them directly from the capsule. The sand-blasting at the tip is helpful as an adjunct to the primary maneuver of irrigation, especially when teasing adherent cortical strands away from the posterior capsule.
For safe removal of cortex from the equator of the bag, direct a stream of cannula irrigation into the bag's fornix to fluff and/or liberate the cortex, and then aspirate it from the rhexis edge. Often, a bag that appears free of cortex turns out, on forniceal irrigation, to have been harboring quite a bit.
The author has no financial interest in any product mentioned.



