Given the widespread occurrence of glaucoma and the popularity of refractive surgery, it's inevitable that the two would intersect. Yet the issues surrounding performing refractive surgery on glaucoma patients are seldom discussed, perhaps The reason may be, in part, that glaucoma specialists have an understandable tendency to focus on the vision-threatening disease and worry less about the patient's refractive error.
Recently, I surveyed 100 glaucoma surgeons and 100 corneal refractive surgeons to get a sense of their perspective on offering refractive surgeries such as LASIK and PRK to patients who either were diagnosed with glaucoma or were in danger of developing it. What I found was something of a disconnect between the two groups. If the patient was a glaucoma suspect, two-thirds of the glaucoma specialists said they'd recommend refractive surgery if the patient wanted it; three-quarters of the cornea specialists agreed. But when the hypothetical patient was already diagnosed with glaucoma, 80 percent of the glaucoma specialists said they would not recommend refractive surgery. In contrast, almost half of the cornea specialists (44 percent) still said they would. (See chart, below.)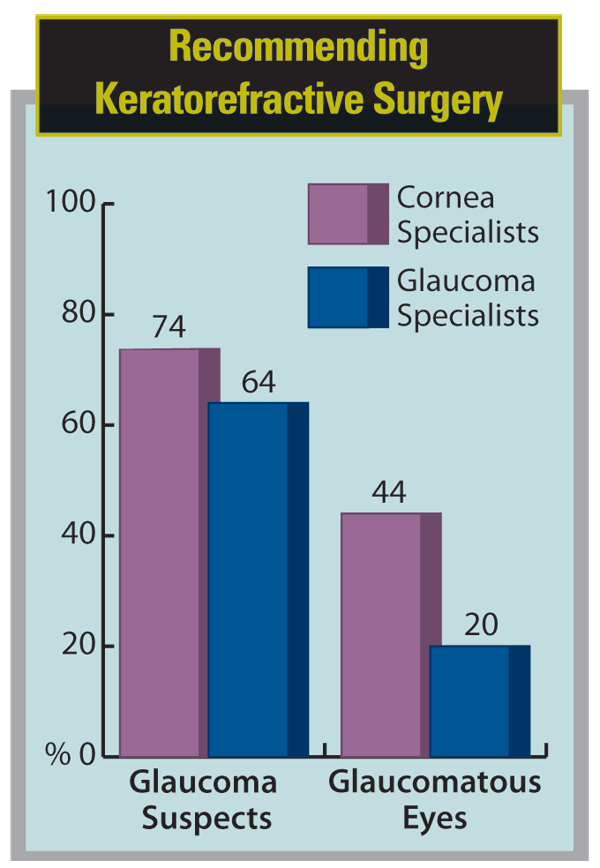
There's not much question that refractive surgery is a safe procedure when performed appropriately, despite the recent U.S. Food and Drug Administration panel convened to review this topic. Millions of individuals have undergone corneal refractive surgery, and 10 or 11 years of data has validated the safety of the procedure. In addition, the armed forces have recently begun to allow fighter pilots to have refractive surgery, and NASA has allowed astronauts to have LASIK. That's a powerful indicator that refractive surgery is considered safe even in situations where a problem would be completely unacceptable. But is it safe for glaucoma patients—and if so, under what circumstances?
Addressing Concerns
Performing refractive surgery on a glaucoma patient certainly raises issues that are not relevant with a healthy patient. Some issues are purely medical; others are medico-legal—for example, protecting yourself from informational ambiguities that could put you at risk of a lawsuit should a patient become unhappy later.
Here are some strategies that can help you manage a glaucoma patient who wants to undergo refractive surgery.
• Consider both the status of the disease and the patient's visual needs. Despite many glaucoma specialists' reservations, refractive surgery makes a lot of sense for some diagnosed glaucoma patients who are well-controlled on medications. If a patient eliminates the need to wear contact lenses, for example, his risk of ocular surface disease drops dramatically. (One in 2,000 daily contact lens wearers risk serious visual loss, compared to one in 10,000 LASIK patients.1) And of course, some patients may simply need more visual acuity than they can get with spectacles or contact lenses because of their occupations. For these individuals the benefits of refractive surgery outweigh the relatively small risks. On the other hand, a patient with uncontrolled glaucoma is probably not a good candidate because of risk factors such as the spike in intraocular pressure caused by the suction ring of a keratome, or the possibility of steroid-induced glaucoma following PRK.
• If a patient is having refractive surgery, make sure the patient's condition is stabilized and documented before the refractive procedure takes place. This is obviously important both to minimize risk during the surgery and to minimize both surgeons' liability afterwards.
• Make sure the refractive surgeon is fully aware of a patient's glaucoma status. Some of the mass market LASIK houses appear to do minimal screening, which puts them (and possibly you) at risk. Of course, the sensible thing to do if you're the refractive surgeon is to get the patient's complete history and do all of the appropriate preoperative tests.
• Reestablish key baselines following the refractive surgery. Certainly the biggest issue here is the change in corneal thickness produced by corneal surgery. As you know, corneal thickness affects IOP readings, and no one has yet come up with a simple fudge factor or formula that converts these measurements based on postop corneal thickness. That means the only alternative is to get a new baseline pressure after the surgery.
Refractive surgery may also affect contrast sensitivity and the patient's results on visual field testing. (In terms of visual fields, the functionality of the retina being measured may not have changed, but the patient's ability to see the stimulus could be improved by refractive surgery, especially if the patient initially had a high correction. That could cause a change in visual field results.) The nature and direction of these changes is impossible to accurately predict, so the only way to ensure accurate monitoring of the patient after refractive surgery is to reestablish the baselines once the patient recovers.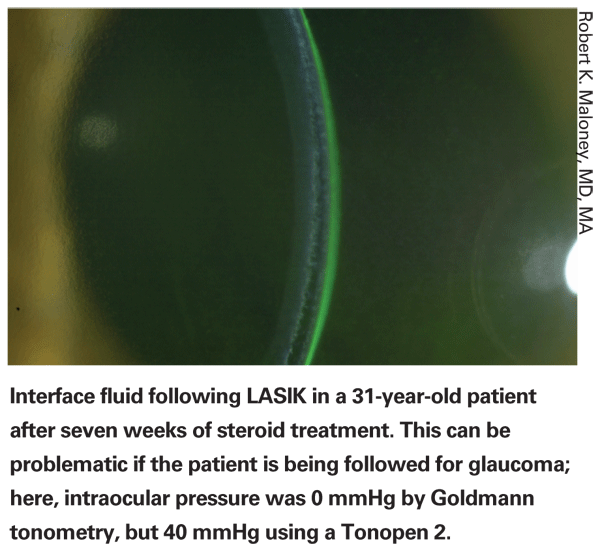
It may be worth noting that some data have suggested that readings made by the GDx scanning laser polarimetry device are affected by refractive surgery as well. However, reports on this have been mixed, and no specific effect of one type has been determined.2-4 Also, despite the apparent change in contrast sensitivity after LASIK, no significant changes in frequency doubling testing have been observed.
• Make sure the patient knows he or she will need to see you a few weeks after the refractive surgery. Explain to the patient that you need to reestablish baselines to ensure that you're able to stay on top of the glaucoma and help the patient avoid ultimately losing vision to the disease.
• Take a picture of the optic nerve after the surgery. This is largely for the legal protection of the refractive surgeon. Suppose a year after the surgery the optic nerve has changed for the worse; a lawyer could claim that the change was a side effect of the refractive surgery, when in fact the glaucoma may simply be progressing. A photograph of the optic nerve taken once the cornea is stable—say, a month after the refractive surgery—can show clearly that the optic nerve was not altered by the refractive procedure.
• If a pressure spike during LASIK could be an issue, a femtosecond laser may be preferable for making the flap. The suction device employed here appears to put less pressure on the eye than the type used with a microkeratome.
• Consider recommending PRK instead of LASIK. Since no flap is created with PRK, this avoids the issue of a pressure rise being generated by the suction ring. Of course, PRK has its own potential concerns centering around the use of steroids after surgery to reduce stromal haze, which can theoretically lead to steroid-induced glaucoma. However, this is becoming less of an issue as many surgeons are relying more on mitomycin-C to prevent haze, allowing a reduction in the overall dose of steroids after the surgery.
• Check for fluid under the LASIK flap post-surgery. This is relatively rare, but a few cases have been reported. Because the fluid can act as a damper, it may lead to falsely low IOP readings. (See image, above.)
• Don't minimize the patient's refractive concerns. Although the health of a patient's eye may be our primary focus, refractive error is a major issue for many patients. Don't avoid the subject, especially if the patient is not yet diagnosed with glaucoma, or if the patient's needs warrant it as a means to improve quality of life.
In any case, remember that the patient's wishes are an important part of the equation. If a patient is enthusiastic about the possibility of LASIK, for example, and you ignore it or fail to address the motivation behind it, the patient may well make his own decision regardless of your stated opinion. Let the patient see that you're taking his or her opinion into consideration and offer a thoughtful recommendation, with clear reasons for your opinion.
• Try to keep yourself informed about the latest options and issues surrounding refractive surgery advances. It's easy to fall behind in this area when your primary concern is protecting your patients from glaucomatous vision loss, but your ability to help a patient who wants to have refractive surgery can be compromised if you're not fully informed about the latest developments. Changes in technology and technique can make a big difference in the relative safety of refractive surgery for glaucoma patients.
The Jury Is Still Out
At this point, we still don't have a lot of clinical data regarding how refractive surgeries affect glaucoma patients. In fact, the interaction of glaucoma with many refractive options, including toric, multifocal and accommodative intraocular lenses, has not been studied extensively. However, if glaucoma was a true contraindication for refractive surgery, poor outcomes would probably have made that clear by now.
In any case, it's inevitable that some of our glaucoma patients will be interested in undergoing refractive surgery. I don't believe we should dismiss the possibility out of hand. Instead, I think it makes sense to take the patient's interest seriously and give advice based on a thorough understanding of the current state of refractive surgery alternatives and the patient's individual condition and needs.
Dr. Lewis is a cataract surgeon and glaucoma specialist in
1. Mathers W, Fraunfelder FW, Rich LF. Risk of LASIK surgery vs contact lenses. Arch Ophthalmol. 2006;124:1510-1511.
2. Choplin. Retinal nerve fiber layer measurements do not change after LASIK for high myopia as measured by scanning laser polarimetry. Ophthal 112:92-97.
3. Gurses-Ozden. Retinal nerve fiber layer thickness remains unchanged following laser-assisted in situ keratomileusis. Am J Ophthal 132:512-516.
4. Lester M, Tizte P, Mermoud A. Retinal nerve fiber layer thickness changes after an acute increase in IOP. J Catarct Refract Surg 2002;28:2117-2122.