One report by Dr. Ambati, an associate professor and vice chair of the university"s Department of Ophthalmology and Visual Sciences, dealt with the composition of drusen, the earliest clinical indicator of macular degeneration and a known risk factor for the development of late-stage AMD. Until now, it has been unclear whether or how drusen can provoke the development of neovascular AMD.
Drusen in AMD patients contain complement proteins C3 and C5. Dr. Ambati"s lab has identified that bioactive fragments of these components, known as C3a and C5a, are present in patients whose AMD progresses beyond dry AMD and into neovascular AMD. The C3a and C5a components in drusen, according to Dr. Ambati, are not only markers of AMD that will develop into the late-stage form of the disease, but they are, in fact, causal. The presence of these components stimulates the progression of AMD. In the future, patients with early-stage AMD may be screened to determine if these effectors exist in their drusen. If they are present, then these patients could be considered at "high risk" for progression to advanced AMD.
The next step for Dr. Ambati"s research is to develop a substance that can block the effectors, halting the progression of AMD from the dry to wet stages. His lab is already testing such substances that could potentially be used in patients with "high-risk" drusen. The work was reported in the Feb. 14 Proceedings of the National Academy of Sciences (pnas.org).
The second area centered on vascular endothelial growth factor, a promoter of angiogenesis. Turning off the source of VEGF to halt angiogenesis and disease progression is a major area of research and drug development. Dr. Ambati"s lab found that while withdrawing VEGF could halt angiogenesis in some areas, it actually encouraged it in others. Dr. Ambati found that this previously undiscovered anti-angiogenic effect of VEGF was mediated via activating VEGFR-1 (VEGF receptor 1) and deactivating VEGFR-2 (VEGF receptor 2).
Additionally, his lab found that a compound known as SPARC (secreted protein, acidic and rich in cysteine) could influence and switch the routing of VEGF away from VEGFR-1. Thus, controlling SPARC levels appears to be key to controlling angiogenesis in macular degeneration.
The findings may have far-reaching implications beyond ophthalmology as angiogenesis contributes to disease progression elsewhere in the body, including malignant tumors. This work appeared in the February issue of the Journal of Clinical Investigation (jci.org).
Correction
Accord Forestalls Medicare Cuts
On February 1, 2006, the House of Representatives voted to approve the amended Budget Reconciliation Agreement. The legislation included a one-year freeze in Medicare physician payment rates at the 2005 levels, which halted the 4.4-percent reduction in 2006 Medicare physician payments that went into effect January 1, 2006. The originally scheduled 4.4-percent reduction went into effect January 1, 2006, because the Senate modified the reconciliation agreement originally approved by the House on December 19. The legislation had to go back to the House for reconsideration before it could be enacted.
The Center for Medicare & Medicaid Services and its contractors were to begin paying claims at the new rates within days of the legislation"s enactment. In addition, because the legislation stated that the freeze in physician payments at the 2005 levels was effective as of January 1, 2006, CMS was automatically reprocessing claims with dates of service between January 1, 2006, and the date of enactment. Providers do not need to resubmit claims already processed with the 4.4-percent reduction. Providers can expect to begin receiving aggregated payments for the difference between the new and previous rates over a period of approximately five months. The aggregated payments will include the usual remittance advice, or Explanation of Medicare Benefits. In light of the change in reimbursement, CMS is offer a second enrollment period for physicians to reconsider their participation status for 2006. The enrollment period will run for an additional 45 days. Should a provider decide to revise his or her participation election during the new enrollment period, the participation election will be retroactive to January 1, 2006.
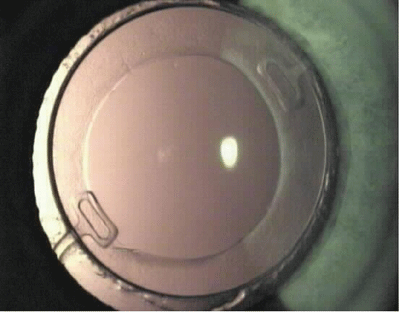
FDA Clears Anterior Segment OCT
Heidelberg Engineering last month received Food and Drug Administration clearance for its SL-OCT commercial optical coherence tomography device used for cross-sectional anterior segment imaging. This is the first commercial application of OCT for anterior segment imaging. The SL-OCT provides noncontact, cross-sectional scans of the anterior segment. Chamber angle, pachymetry, flap thickness, corneal curvature and comprehensive biometric measurements are possible with the instrument, as well as pre- and post-surgical comparisons.
Dry-Eye Drop Shows Positive Early Results
Ista Pharmaceuticals announced positive preliminary results from its randomized, three-arm (placebo, 3.0% and 3.9%) Phase IIb clinical study of ecabet sodium, a prescription eye drop being evaluated for the treatment of keratoconjunctivitis sicca. Ecabet sodium is a new class of molecules that increase the quantity and quality of mucin produced by conjunctival goblet cells and corneal epithelia.
The preliminary results of the study demonstrated a strong trend in efficacy for the lower (3%) dose with respect to ecabet sodium"s ability to address two objective signs of dry eye syndrome, corneal staining and blink rate. In addition, patients treated with the lower dose of ecabet sodium reported positive trends for reductions in symptomatology as measured by ocular surface disease index and most bothersome symptom. In the preliminary results, no efficacy trends versus placebo were observed with respect to the higher (3.9%) dose. Further analyses of the Phase IIb results are ongoing.
ISTA"s Phase IIb study was designed to identify the appropriate sign and symptom and time course for future studies. Generally, improvement in one sign and one symptom in Phase III studies is considered acceptable by the FDA for approval of a prescription dry eye product. Therefore, a total of 162 patients were enrolled in the U.S., randomized, three-arm Phase IIb trial and were randomly assigned to receive placebo, 3.0% or 3.9% ecabet sodium in the study eye four times a day for 90 days. Patients were evaluated for signs and symptoms four times during the trial both prior to and following exposure to a controlled adverse environment chamber. The trial evaluated ocular signs, including corneal and conjunctival staining, tear-film breakup time and blink rate, and ocular symptoms, including burning or stinging, itchiness or scratchiness, grittiness or sandiness, foreign body sensation, haziness and blurriness. In addition, the preliminary findings suggest a favorable safety profile.
Ista plans to complete its analyses of these results to confirm the preliminary findings and move quickly into a smaller, short-term confirmatory study designed to further define the subpopulation of patients to enroll and other elements of its Phase III studies. Assuming timely and successful completion of this confirmatory study, its plan is to initiate a Phase III study during 2007.
Study Gives Good Grades for Cataract Patient Satisfaction
Pre-procedure processing of patients, staffing and purchasing practices, scheduling, and billing and collection methods are key factors in the efficiency of ambulatory health-care centers performing the most common outpatient surgical procedure: cataract extraction with lens insertion. Overall, patient satisfaction was high across all centers.
These are among the findings from the first non-clinical study of cataract surgery in ambulatory health care centers conducted by the AAAHC Institute for Quality Improvement, a subsidiary of the Accreditation Association for Ambulatory Health Care. The study assessed performance measures on key non-clinical aspects of cataract surgery performed in ambulatory health-care centers, including administrative and financial processes and patient satisfaction outcomes. The study results are intended for quality improvement purposes, but they are inappropriate for use in setting reimbursement rates. The key findings include:
* Staff costs per procedure ranged from $26 to $220 (median $110). Efficiencies related to lower staff costs included using part-time staff, cross-training staff and preparing paperwork/charts in advance.
* Supply costs per procedure ranged from $95 to $1,347 (median $310). Practices associated with lower costs included standardizing supplies, consolidating vendor contracts, reviewing vendor performance/pricing and streamlining supply packs used for procedures.
In general, patient satisfaction was high regardless of how ambulatory health-care centers ranked on the non-clinical outcomes measured:
* More than 99 percent of patients rated their overall experience as positive and less than 1 percent rated it as negative or neutral.
* 93 percent of patients indicated their procedures were scheduled as soon as they wanted.
* 30 percent of patients said they had to wait past their scheduled procedure time. Of those, 8 percent said the wait was shorter than expected; 38 percent said the wait time was as expected and 54 percent said they waited longer than expected.
* 96 percent said health care providers showed concern for their comfort.
The AAAHC Institute Cataract Extraction with Lens Insertion Non-Clinical Study was conducted between July and September 2004, and included 33 organizations that together perform nearly 117,000 cataract surgeries per year. Real-time data on factors including scheduling, patient processing, staffing, facility time, billing, collection and other costs associated with cataract surgery were gathered. Data from organizations that completed study questionnaires for 15 or more procedures were used in the benchmark analyses. Included in the final analyses were 625 cataract cases from 25 ambulatory organizations.