Concurrent with this discovery, Dr. Ambati’s laboratory developed two promising therapies for the prevention of the condition. This study also elaborates, for the first time, a disease-causing role for a large section of the human genome once regarded as non-coding “junk DNA.”
Geographic atrophy, which causes retinal cell death, occurs in the later stages of dry macular degeneration. There is currently no effective treatment for GA.
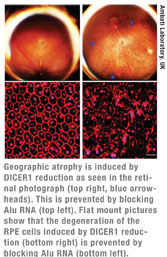 Dr. Ambati’s team discovered that an accumulation of a toxic type of RNA, called Alu RNA, causes retinal cells to die in patients with geographic atrophy. In a healthy eye, a “Dicer” enzyme degrades the Alu RNA particles.
Dr. Ambati’s team discovered that an accumulation of a toxic type of RNA, called Alu RNA, causes retinal cells to die in patients with geographic atrophy. In a healthy eye, a “Dicer” enzyme degrades the Alu RNA particles.
“We discovered that in patients with geographic atrophy, there is a dramatic reduction of the Dicer enzyme in the retina,” said Dr. Ambati, a professor and vice chair of the Department of Ophthalmology and Visual Sciences. “When the levels of Dicer decline, the control system is short-circuited and too much Alu RNA accumulates. This leads to death of the retina.”
Alu elements make up a surprisingly large portion—about 11 percent by weight—of the human genome, comprising more than 1 million sequences. However, their function has been unknown, so they have been called “junk” DNA or part of the “dark” genome. The discovery of Alu’s toxicity and its control by Dicer should prove of great interest to other researchers in the biological sciences, Dr. Ambati says.
The team developed two potential therapies aimed at preventing geographic atrophy and demonstrated the efficacy of both approaches using laboratory models. The first involves increasing Dicer levels in the retina by “over-expressing” the enzyme. The second involves blocking Alu RNA using an “anti-sense” drug that binds and degrades this toxic substance. UK has filed patent applications for both technologies, and Dr. Ambati’s group is preparing to start clinical trials by the end of this year.
“These findings provide important new clues on the biological basis of geographic atrophy and may provide avenues for intervention through preventing toxic accumulation of abnormal RNA products,” said Paul Sieving, MD, director of the National Eye Institute.
This work has “widespread implications” for future study, said Stephen J. Ryan, MD, president of the Doheny Eye Institute and member of the Institute of Medicine. “The authors have opened an important line of research with real possibilities for future therapeutic intervention for patients with geographic atrophy.”
 Free Radicals May Lead to Fuchs’
Free Radicals May Lead to Fuchs’
Scientists at Schepens Eye Research Institute have found that free radicals may cause the damage in the eyes of patients with Fuchs’ Endothelial Corneal Dystrophy, one of the most common reasons for corneal trans-plants worldwide.
The finding, published in the November 2010 American Journal of Pathology, holds promise for early and preventative treatments for this disease, which impacts nearly 4 percent of the population over age 60.
“Our discovery is significant, because it gives us the first hope for slowing the progression of the disease,” says Ula V. Jurkunas, MD, the principal investigator of the study and a corneal surgeon at Massachusetts Eye and Ear Infirmary in Boston. “If we can identify how free radicals are involved in this and what antioxidants can fight them, we can create a regimen that can help protect the cornea,” she adds.
Because corneal endothelial cells do not regenerate themselves, the only effective treatment for Fuchs’ has been corneal transplant. While scientists have made progress in identifying some genes that cause the disease, they have made little or no progress in defining the mechanisms at play.
Dr. Jurkunas began to believe that a free radical process might be part of what is happening within the Fuchs’ dystrophy-plagued cornea. Free radicals are unstable molecules released by the body, leading to oxidization, which causes cell death. Antioxidants are known to bind with and neutralize free radicals.
To test the theory, Dr. Jurkunas and her colleagues took numerous tissue samples from patients undergoing corneal transplants and tested them for evidence of free radical oxidation and subsequent tissue damage.
In the significant majority of specimens, the scientists found that the level of antioxidants was less than normal, or down-regulated. They also found evidence of high rates of damage to the cells’ DNA, which is particularly susceptible to free radicals.
Dr. Jurkunas says the next step is to identify the specific antioxidants that would neutralize the free radicals involved in the damage and possibly prevent or block their destructive action.
Osmolarity Best for Dry-Eye Diagnosis
Tear osmolarity is the best single metric both to diagnose and classify dry-eye disease, according to a prospective, multicenter, observational case series reported online on Feb. 8 by the American Journal of Ophthalmology. The Georgetown University-centered study included 314 consecutive subjects between 18 and 82 years of age. Bilateral tear osmolarity, tear-film breakup time, corneal staining, conjunctival staining, Schirmer test and meibomian gland grading were performed. Diagnostic performance was measured against a composite index of objective measurements that classified subjects as having normal, mild or moderate or severe dry eye. The main outcome measures were sensitivity, specificity, area under the receiver operating characteristic curve, and inter-eye variability.
Of the six tests, tear osmolarity was found to have superior diagnostic performance. The most sensitive threshold between normal and mild or moderate subjects was found to be 308 mOsms/L, whereas the most specific was found at 315 mOsms/L. At a cutoff of 312 mOsms/L, tear hyperosmolarity exhibited 73 percent sensitivity and 92 percent specificity. The other common tests exhibited either poor sensitivity (corneal staining, 54 percent; conjunctival staining, 60 percent; meibomian gland grading, 61 percent) or poor specificity (TBUT, 45 percent; Schirmer test, 51 percent). Intereye differences in osmolarity were found to correlate with increasing disease severity and are a characteristic of dry eye not seen in normal subjects.
Avastin May Offer ROP Treatment
The cancer drug Avastin (bevacizumab) was shown to be superior to laser treatment in premature infants with retinopathy of prematurity, a leading cause of childhood blindness worldwide. The findings, from a research team at the University of Texas Health Science Center at Houston, were reported in the New England Journal of Medicine on February 17, 2011.
Peripheral retinal ablation with conventional (confluent) laser therapy is destructive, causes complications and does not prevent all vision loss, especially in cases of retinopathy of prematurity affecting zone I of the eye. Case series in which patients were treated with vascular endothelial growth factor inhibitors suggest that these agents may be useful in treating retinopathy of prematurity.
The prospective, controlled, randomized, multicenter trial assessed intravitreal bevacizumab monotherapy for zone I or zone II posterior stage 3+ (i.e., stage 3 with plus disease) retinopathy of prematurity. Infants were randomly assigned to receive bevacizumab (0.625 mg in 0.025 ml of solution) or conventional laser therapy, bilaterally. The primary ocular outcome was recurrence of ROP in one or both eyes requiring retreatment before 54 weeks postmenstrual age.
The study enrolled 150 infants (total sample of 300 eyes); 143 infants survived to 54 weeks postmenstrual age, and the seven infants who died were not included in the primary-outcome analyses. ROP recurred in four infants in the bevacizumab group (six of 140 eyes [4 percent]) and 19 infants in the laser-therapy group (32 of 146 eyes [22 percent], p=0.002). A significant treatment effect was found for zone I retinopathy of prematurity (p=0.003) but not for zone II disease (p=0.27).
Intravitreal bevacizumab monotherapy, as compared with conventional laser therapy, in infants with stage 3+ retinopathy of prematurity showed a significant benefit for zone I but not zone II disease. Development of peripheral retinal vessels continued after treatment with intravitreal bevacizumab, but conventional laser therapy led to permanent destruction of the peripheral retina. This trial was too small to assess safety, the authors say.
Might Obese Women Have Less OAG?
Obesity may be associated with higher eye pressure and a decreased risk of open-angle glaucoma in women but not men, according to a report posted online that will appear in the May issue of Archives of Ophthalmology.
Wishal D. Ramdas, MD, M.Sc., of the Erasmus Medical Center, Rotterdam, the Netherlands, and colleagues examined data from 3,939 participants in the Rotterdam Study. This population-based study included participants 55 years of age and older who did not have OAG when the study began between 1991 and 1993.
Over an average of 9.7 years of follow-up, 108 participants (2.7 percent) developed OAG. Those who developed the condition were significantly older, more often had high myopia and were more often male, compared with those who did not. No statistically significant effect of socioeconomic status, smoking or alcohol intake was found on the development of OAG.
Among women, there was a significant association between increased body mass index and intraocular pressure. However, each one-unit increase in body mass index was associated with a 7-percent decreased risk of developing open-angle glaucoma. These associations were not present in men.
Excess fat tissue could place increasing pressure on the eye sockets, thereby increasing pressure within the eye, the authors note. The higher IOP among obese women should have resulted in an increased risk for glaucoma. “However, this effect was not observed and thus the multivariate analysis yielded a protective effect of body mass index on open-angle glaucoma incidence in women,” the authors write.
“Another explanation might be that high estrogen levels and hormone therapy might be protective to open-angle glaucoma, and obesity seems to be positively related with postmenopausal plasma estrogen levels.”
“Obesity appears to be associated with a higher intraocular pressure and a lower risk of developing open-angle glaucoma,” the authors conclude. “These associations were only present in women. Other lifestyle-related factors, such as socioeconomic status, smoking and alcohol consumption, were not associated with open-angle glaucoma.”



