AS PROCEDURES BECOME MORE COMPLEX AND PATIENT expectations increase, the need for more detailed and accurate clinical information about the eye continues to grow. One of the new generation of instruments designed to meet that need is the Pentacam, from Oculus. Now approved in the United States for more than a year, the Pentacam provides both familiar and new measurements of the cornea and anterior chamber.
The Pentacam is the first instrument to use a rotating Scheimpflug camera to take multiple images of the anterior segment and use these to generate three-dimensional images and calculate measurements of the eye. It provides:
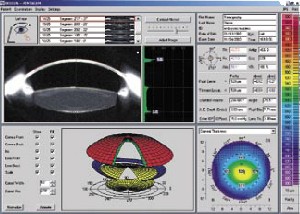
• Detailed Scheimpflug images of the anterior segment from the posterior surface of the crystalline lens to the anterior corneal surface.
• Three-dimensional visualization and animation of the anterior segment.
• Measurements of anterior chamber angle, chamber volume, chamber depth, pupil diameter and corneal characteristics such as eccentricity, central radius and astigmatism.
• Pachymetry (limbus to limbus, accurate to ±5 µm). You can locate any point on the cornea manually, onscreen, and see the thickness at that point. The map notes the thinnest region.
• Densitometry data for the cornea and the crystalline lens, including the subcapsular layer, shown both graphically and quantitatively. The quantitative data make it easy to identify a developing cataract, categorize existing cataracts, and document their development.
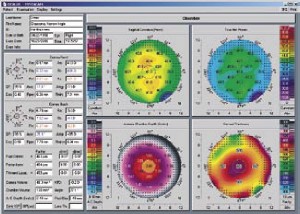
• Topographic maps of the anterior and posterior corneal surfaces, based on measurement of 25,000 elevation points (when using the two-second scan), including tangential and sagittal (axial) curvature and limbus-to-limbus elevation, with freely selectable reference bodies.
• A "true net power map" that shows the refractive power of the cornea at any given point. (The instrument calculates the refractive power of both surfaces and adds them together.)
 |
  |
Because the Pentacam only measures to the posterior capsule of the crystalline lens, it can't provide a measure of axial length. Also, because it's optically based, it can't measure from sulcus to sulcus. However, it can usually capture data behind an opacity because the camera images the eye from so many angles.
Using the Technology
The data is acquired—without touching the eye—using one of three scan modes, based on 12, 25 or 50 images (requiring half a second, one second, or two seconds to acquire, respectively). While scanning, the instrument monitors and corrects for eye movement and reports on the quality of each measurement. Doctors report that the data compare well with data from other instruments and show high reproducibility.
Users can view any four maps at once onscreen, or select a single one for closer examination; a comparison screen allows evaluation of serial scans. Users can zoom in and adjust Scheimpflug image contrast to examine details.
A key advantage of this technology is that because the measurements are made by a rotating source, the central measurements are based on a much greater number of data point scans than those provided by a linear scanner. (Some topographers don't measure the central cornea at all; they extrapolate the central measurements.)
In addition to conventional uses, the Pentacam can calculate corrected intraocular pressure, taking corneal thickness into account; image and measure a filtration bleb; document the extent of posterior capsule opacification; help to fit orthokeratology contact lenses; and evaluate corneal striae in post-LASIK eyes. Jack Holladay, MD, clinical professor of ophthalmology at Baylor College of Medicine in Houston, is currently determining whether the Pentacam's true net power map can be used to calculate accurate post-LASIK intraocular lens power.
The Clinical Perspective
Daniel S. Durrie, MD, owner of Durrie Vision, in Overland Park, Kan., says that the Pentacam has been very valuable in his practice. "Now that we have the option of refractive lensectomy and lenses like ReStor and Crystalens, we have to decide whether the patient should have a corneal procedure or a lens procedure," he explains. "The Pentacam has helped us determine which optical problems are in the cornea and which are in the lens. We use it for preop evaluation of every patient.
"Until now, we really haven't had a good way to analyze the lens in the eye," he explains. "We've looked at it with the slit lamp and tried to remember it from the previous visit to determine whether it's changed. But the Pentacam can measure the density of a cataract, and make it clear whether lens density is changing.
"It's also useful because we can show the patient his lens," he adds. "It gives him some idea of what we mean when we say he has an early cataract."
John E. Sutphin Jr., MD, director of the Refractive Corneal Surgery program in the Department of Ophthalmology and Visual Sciences at the University of Iowa, says the technicians in his office like the instrument. "It's much easier to use than most of our instruments," he notes. "It's also easy for patients; they just sit and look straight ahead.
"I think anybody doing refractive surgery should measure the posterior curve, not only as part of the screening, but as part of the evaluation for retreatment, because of the issue of ectasia," he adds.
Marc Michelson, MD, who performs refractive surgery in Birmingham, Ala., says that Pentacam data has allowed him to perform LASIK on many patients that he would otherwise have rejected because of abnormal topography. "Evaluating the pachymetry and anterior and posterior elevation data showed that the cornea was not really abnormal," he explains.
"I don't charge a separate fee for using the Pentacam," he notes, "but I did return a pachymeter and saved $5,000."
Ectasia: A Measurement Artifact?
Michael Belin, MD, medical director of TLC Laser Eye Center in Albany, N.Y., and professor and director of cornea & refractive surgery at Albany Medical College, notes a difference in the way the Pentacam and Orbscan measure post-LASIK or abnormal corneas. "It's well-documented in the literature that while the Orbscan is reasonably accurate in normal corneas, it routinely underestimates thickness by 30 to 45 µm in postop or abnormal corneas."1,2 Dr. Belin believes that this may be contributing to erroneous assumptions about post-LASIK ectasia.
Dr. Belin examined one patient who's LASIK flap had become a buttonhole; the procedure had been aborted as a result. "The patient had a zero-thickness flap in the center and no treatment. Yet the Orbscan postop posterior topography showed a significant ectasia that did not exist preoperatively. We imaged the same patient using the Pentacam and found a completely normal posterior elevation," he says. "It may be that any opacity, even one that is barely visible on slit lamp such as the interface that a LASIK flap makes, is enough to throw the Orbscan off."
Dr. Belin has also noted the usefulness of the Pentacam's ability to rate lens transmissibility. "One patient was referred to us with unexplained induced myopia," he says. "On slit lamp examination his lenses looked very similar. However, the Pentacam showed a significant difference in transmissibility, accounting for the induced myopia."
To find out more about the Pentacam, call 1 (888) 284-8004, or visit OculusUSA.com.
1. Nawa Y, et al. Evaluation of apparent ectasia of the posterior surface of the cornea after keratorefractive surgery. J Cataract Refract Surg 2005; 31:571-573
2. Cairns G, et al. Assessing the accuracy of Orbscan II post-LASIK: Apparent keratectasia is paradoxically associated with anterior chamber depth reduction in successful procedures. Clin Exp Ophthalmology, April 2005;33:147-152.




