Since September 11, 2001, the
The Route to Walter Reed
Eye injuries sustained while in a combat zone are defined as "Combat Ocular Trauma." COT is categorized as non-penetrating and penetrating. Penetrating posterior segment COT associated with a retained intraocular foreign body (IOFB) is primarily repaired in
After closing an open globe with an IOFB, the deployed ophthalmologist will inject subconjunctival antibiotics and start the soldier on levofloxacin 500 mg every day PO or IV, a topical fourth generation fluoroquinolone q.i.d., atropine 1% b.i.d. and Pred Forte 1% q.i.d. The soldier is re-evaluated at LRMC to rule out endophthalmitis and retinal detachment and receives a multidisciplinary medical evaluation with comprehensive treatment of all injuries.1
Most soldiers with COT are sent to
Removal of an IOFB secondary to COT in the current medical evacuation process is, by definition, delayed more than 24 hours. A soldier with COT rarely arrives at
Preop Preparation
Upon the patient"s arrival at Walter Reed, we perform a complete examination followed by an B-scan ultrasound and a fine-cut computed tomography scan. We always ask for the thinnest CT cuts possible with axial and coronal views. The newest CT scanners can image in increments of 0.625 mm, which will identify most IOFBs. The examination gives us important information such as visual acuity, intraocular pressure, presence of an afferent papillary defect (suggestive of optic nerve or vascular injury and worse visual prognosis), evidence of angle recession, signs of endophthalmitis, entry and exit sites of the IOFB, and presence of traumatic cataract, vitreous hemorrhage, corneal edema, choroidal hemorrhage or retinal detachment.
Furthermore, the location and size of the IOFB on the CT scan or ultrasound gives valuable information needed for surgical planning of IOFB removal. IOFBs located in the anterior chamber, lens or vitreous cavity as well as those associated with small retina tears account for five of six IOFB cases and have an excellent prognosis. The proliferative vitreoretinopathy rate in these eyes is 5 percent, with final best corrected visual acuity ¡Ý20/40 in 50 percent of cases. IOFBs through the retina, subretinal space, suprachoroidal space, embedded in the sclera or perforating through the sclera carry a much worse prognosis. The PVR rates in these cases are up to 75 percent with final BCVA worse than 20/200 in 20 to 25 percent of cases.1
Numerous preoperative complications can develop secondary to IOFBs. Two scenarios that require urgent removal include post-traumatic endophthalmitis and retinal detachment. Within our consecutive series of approximately 90 IOFB removal cases, none has shown clinical signs of endophthalmitis even with numerous IOFBs consisting of stone, sand and concrete. A meta-analysis of 2,540 consecutive IOFB cases published in the literature found 230 (8.7 percent) cases of IOFB-related endophthalmitis. Likewise, retinal detachments associated with IOFBs are usually repaired within 24 hours of presentation.2,3,4 Other common preoperative complications include corneal lacerations, traumatic cataract, vitreous hemorrhage, choroidal hemorrhage, retinal tears, posterior scleral perforating wounds, macular holes, traumatic optic neuropathy and retinal vascular injury (BRVO/BRAO) secondary to the impact of the IOFB.1,5 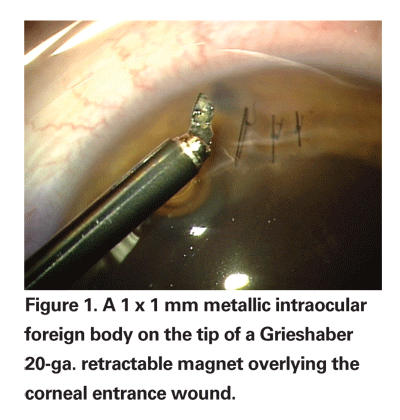
IOFB removal cases are very complicated compared to other vitreoretinal procedures. Surgical efficiency and speed are critical to successful IOFB removal. Corneal clarity is limited following traumatic injury and will worsen with increased intraoperative surgical time. Although most IOFB removal cases are straightforward, a large IOFB that is embedded in the sclera through a dense vitreous hemorrhage with an associated retinal detachment and corneal laceration/edema will challenge even the most experienced OR technician or nurse. Any significant intraoperative delay may cost valuable time as the cornea becomes more edematous and the view worsens, necessitating a temporary keratoprosthesis followed by a penetrating keratoplasty. The graft failure rate in these young patients generally exceeds 50 percent, and grafts are therefore avoided whenever possible.6
Given the potential deleterious consequences of intraoperative delays secondary to operating room support staff, we schedule IOFB removal on days when we have our most experienced and qualified operating room support staff rather than operating after hours. In order to decrease the risk of endophthalmitis, we keep all IOFB patients on levofloxacin 500 mg
Operative Technique
We employ a standard three port, 20-ga. pars plana vitrectomy usually with a 6-mm infusion cannula secondary to traumatic cataract with or without choroidal hemorrhage. We use the Alcon Accurus vitrectomy system with the high brightness illuminator. The core vitrectomy is performed using the 3D vitrectomy settings, and we shave the vitreous base with mobile retina settings of 2,500 cpm/30 mmHg vacuum. We avoid a prophylactic scleral buckle encircling band if a complete vitreous base shave is performed.
Approximately 70 percent of our IOFB cases are associated with a traumatic cataract. The vitrector is used to perform a pars plana lensectomy leaving as much anterior capsule as possible to support a sulcus intraocular lens in the future. We have moved away from performing a combined cataract extraction with sulcus IOL insertion during the IOFB removal. These cases frequently developed synechiae to the anterior IOL surface or optic capture/dislocation secondary to postoperative gas tamponade treatment. Most commonly, the IOFB will damage less than 180 degrees of anterior capsule support and patients who are left surgically aphakic have a secondary intraocular lens placed three months after IOFB removal. The secondary IOL options are a sulcus posterior chamber IOL such as an Alcon MA60 or MA50, or a sulcus-fixated posterior IOL such as the Alcon CZ70. We avoid an anterior chamber IOL in our young patients. It is not uncommon for us to insert one CZ70 haptic into the sulcus and suture the other haptic to the sclera when anterior capsule support is less than 180 degrees.
One of the most important aspects of vitreoretinal surgery for IOFB is good visualization of the retina, vitreous and IOFB itself. Visualization of the IOFB and retina is critical to achieve a low PVR rate and improved postoperative visual acuity. The high brightness xenon light source illuminator is crucial in visualizing IOFBs and treating retinal pathology through corneal edema. The xenon light source used with a chandelier light such as the Tornambe Torpedo is an excellent method for bimanual manipulation or removal of an IOFB. The xenon light source attached to a lighted 20-ga. curved endolaser probe provides the best illumination to perform laser retinopexy to the retinal periphery. Intraoperative triamcinolone is also useful in these cases in identifying residual cortical vitreous or creating a posterior vitreous detachment.
Use of the BIOM wide-angle non-contact viewing system has revolutionized our ability to visualize the retina through small clear windows in the cornea. The non-contact system avoids opening recently repaired corneal lacerations, and the wide-field viewing provides efficient localization of the IOFB prior to removal. The BIOM combined with the xenon light source allows adequate visualization of IOFBs through corneal edema and laceration repairs to minimize the need for temporary keratoprosthesis and penetrating keratoplasty. If the small area of clear cornea is too far peripheral, we use iris retractors to stretch the pupil and improve intraoperative visualization during vitrectomy.
Surgical incision placement is dictated by the location and size of the IOFB. IOFBs greater than 4 x 4 x 4 mm should be removed through a limbal incision necessitating a pars plana lensectomy. Larger IOFBs are difficult to remove through a pars plana incision due to globe collapse (with infusion pressure of 60 mmHg) and poor view during IOFB removal. 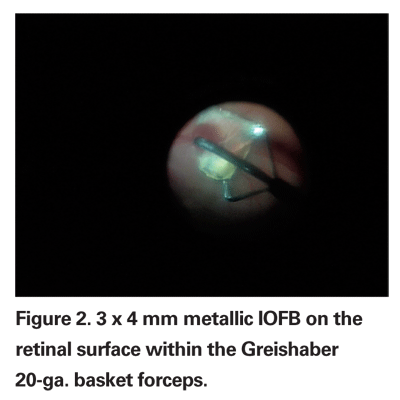
We use three commercially available IOFB forceps from Grieshaber. External magnets are not used for IOFB removal at our institution. The retractable 20 gauge magnet used in 20 percent of cases is an excellent choice for metallic magnetic IOFBs less than 1 mm in diameter (See Figure 1). The 20-ga. basket forceps is used in 60 percent of cases for IOFBs between 1.0 and 4.0 mm (See Figure 2). This instrument is particularly useful to prevent IOFBs from catching on the edge of the sclerotomy incision and falling back into the vitreous cavity. The diamond coated 20-ga. IOFB forceps are useful for IOFBs with an edge less than 5 mm in width and are used in 20 percent of our cases (See Figure 3). With large IOFBs, two 20-ga. IOFB forceps are needed to perform a scleral tunnel incision removal, similar to removing a dislocated IOL.
Postoperative complications include corneal astigmatism and scarring, which may require a penetrating keratoplasty at six months post-IOFB removal. Other common complications include traumatic optic neuropathy with visual field defects, secondary glaucoma requiring a tube shunt, and sensory exotropia/esotropia requiring strabismus surgery.
Outcomes
Primary outcome measures for IOFB cases include final BCVA and PVR. Our predecessor at Walter Reed waited an average of 21 days prior to IOFB removal. After reviewing these 79 cases, we found only one case of preoperative PVR. However, a spontaneous PVD only occurred in 25 percent of cases (average patient age of 27 years) with the average time to PVD formation being 30 days in these cases.1 Our overall PVR rate was 20 percent and is consistent with the average published IOFB PVR rates of 20 to 25 percent.8 The PVR rate definitely depends on the extent of intraocular damage from the IOFB. Those IOFBs that penetrate deeper than the retina have a much higher rate of PVR formation and subsequent worse visual outcome than IOFBs that remain in the vitreous cavity. Fortunately, approximately five out of six IOFBs do not penetrate deeper than the retina in our experience.
Risk factors for poor visual outcome are multifactorial. The most important criteria are the formation of PVR and penetration level of the IOFB as discussed above. Traumatic optic neuropathy also plays a contributing role in decreased visual acuity. We have been able to use a mfERG and mfVEP to assist in the postoperative elucidation of retinal versus optic nerve pathology. Other contributing factors to poor postoperative visual acuity include corneal scarring and secondary glaucoma from severe trabecular meshwork damage. Analyzing all cases of IOFB removal, our final BCVA >20/40 is 53 percent and BCVA <20/200 is 22 percent.1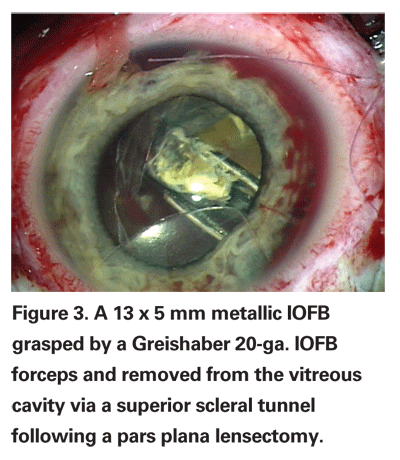
Since statistically reviewing our patients, we are focused on reducing the PVR rates in the cases where IOFBs penetrated deeper than the retina. We have moved in the direction of localized choroidectomy in these cases to prevent postoperative PVR and phthisis.9 We currently have encouraging results on a limited number of cases with at least six months of follow-up. Comparing similar groups of severe IOFB injuries at our institution, choroidectomy has reduced the incidence of PVR from 89 percent to 33 percent (p=0.12) and phthisis from 53 percent to 13 percent(p=0.13). In theory, a choroidectomy debrides necrotic RPE and choroid in these severe injuries, and this may contribute to less postoperative formation of PVR and phthisis.
In summary, despite severe COT referred for treatment, most treated soldiers retain good vision. Moreover, a delayed IOFB removal approach necessitated by our evacuation system appears not to have led to complication rates higher than those found in the literature describing more immediate IOFB removal.
Drs. Weichel and Colyer are in the Department of Surgery/Ophthalmology Service at
1. Colyer MH WE, Weichel ED et al. Delayed Intraocular Foreign Body Removal without Endophthalmitis during Operations Iraqi Freedom and Enduring Freedom. Ophthalmology 2007; In press.
2. Williams DF, Mieler WF, Abrams GW, Lewis H. Results and prognostic factors in penetrating ocular injuries with retained intraocular foreign bodies. Ophthalmology 1988;95:911-6.
3. Brinton GS, Topping TM, Hyndiuk RA, et al. Posttraumatic endophthalmitis. Arch Ophthalmol 1984; 102:547-50.
4. Parver LM, Dannenberg AL, Blacklow B, et al. Characteristics and causes of penetrating eye injuries reported to the National Eye Trauma System Registry, 1985-91. Public Health Rep 1993;108(5):625-32.
5. Nguyen QD, Kruger EF, Kim AJ, et al. Combat eye trauma: intraocular foreign body injuries during the Iran-Iraq war (1980-1988). Int Ophthalmol Clin 2002; 42(3):167-77.
6. Garcia-Valenzuela E, Blair NP, Shapiro MJ, et al. Outcome of vitreoretinal surgery and penetrating keratoplasty using temporary keratoprosthesis. Retina 1999;19:424-9.
7. Woodcock MG, Scott RA, Huntbach J, Kirkby GR. Mass and shape as factors in intraocular foreign body injuries. Ophthalmology 2006;113:2262-9.
8. Jonas JB, Budde WM. Early versus late removal of retained intraocular foreign bodies. Retina 1999;19: 193-7.
9. Kuhn F, Mester V, Morris R. A proactive treatment approach for eyes with perforating injury. Klin Monatsbl Augenheilkd 2004;221(8):622-8.



