Veterans Administration Optometric Surgery Debate Fades
THE VETERANS HEALTH ADMINistration rescinded a controversial directive that had allowed laser eye surgery to be performed at VA facilities by optometrists. A new directive, from Jonathan Perlin, MD, acting undersecretary, limits the performance of therapeutic laser surgery in the VA system to qualified ophthalmologists.
The Veterans Eye Treatment Safety Coalition, including the American Medical Association, American College of Surgeons, the American Osteopathic Association, the American Academy of Ophthalmology, the American Academy of Family Physicians and the American Society of Cataract & Refractive Surgery, had fought to reverse the earlier ruling permitting some ODs to perform laser surgery based on their state"s scope of practice, but under the supervision of an ophthalmologist. The controversy began in April 2003 when an Oklahoma-licensed optometrist in a Kansas VA facility had been privileged for laser eye surgery.
After the first ruling, a panel of VA optometrists and ophthalmologists was formed to define the supervision requirement. When the panel failed to reach an accord, the optometrists reportedly abandoned the issue.
"The VA"s directive is a victory for veterans," said Priscilla Arnold, MD, ASCRS president. "The laws of Oklahoma fly in the face of medical norms--all other states have laws protecting consumers from eye surgery by non-medical doctors, and at least 35 states expressly prohibit eye surgery by non-physicians."
Florida Stem Cell Research Targets Retinopathy
UNIVERSITY OF FLORIDA REsearchers reported in early January that they have prevented blindness in mice with simulated retinopathy. Writing in the Journal of Clinical Investigation, the researchers described their use of an antibody to block the formation of the protein SDF-1 in the eyeballs of mice with simulated retinopathy. The researchers effectively silenced SDF-1"s signal to activate normally helpful blood stem cells, which become too much of a good thing within the close confines of the eyeball.
|
|
|
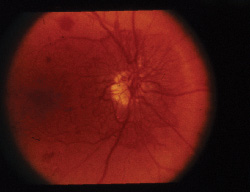
Florida researchers isolated a protein that contributes to retinopathy. |
"SDF-1 is the main thing that tells blood stem cells where to go," said Edward Scott, PhD, an associate professor of molecular genetics at the UF Shands Cancer Center and director of the Program in Stem Cell Biology and Regenerative Medicine at UF"s College of Medicine. "If you get a cut, the body makes SDF-1 at the injury site and the repair cells sniff it out. The concentration of SDF-1 is higher where the cut occurs and it quickly dissipates." In the vitreous, however, the SDF-1 doesn"t break down. It continues to recruit new blood vessels.
UF researchers analyzed samples of the vitreous gel taken from the eyes of 46 patients undergoing treatment for diabetic eye disease, including 24 patients with retinopathy. They found SDF-1 in each of the patients, with the highest amounts detected in patients with the worst cases. No traces of SDF-1 were found in the vitreous samples of eight nondiabetic patients who were treated for other ailments.
With the hypothesis that SDF-1 is at the heart of the problem, the scientists tested to see whether the addition of the protein would call stem cells and spur extraordinary blood vessel growth in the eyeballs of 10 laboratory mice. They succeeded, creating mice with retinopathy-like conditions. Then, as a treatment, scientists injected an SDF-1 antibody directly into the afflicted eyes. The antibody, another protein that binds to the SDF-1, disabled SDF-1"s ability to summon stem cells, effectively halting the growth of almost all new blood vessels.
They next plan to test the technique in monkeys, and if it continues to be successful, to test the therapy in human clinical trials.
Retinopathy Linked to Congestive Heart Failure
RETINOPATHY IS AN INDEPENDENT PREDICTOR of congestive heart failure, even in persons without preexisting coronary heart disease, diabetes or hypertension, according to a study published in January"s Journal of the American Medical Association.
The population-based, prospective seven-year cohort study in four communities in the United States used the Atherosclerosis Risk in Communities Study database. Participants numbered 11,612, aged 49 to 73 years. All had retinal photographs taken between 1993 and 1995. The photographs were graded according to a standardized protocol for the presence of retinopathy (e.g., microaneurysms, retinal hemorrhages, soft exudates), arteriovenous nicking, focal arteriolar narrowing, and generalized arteriolar narrowing.
The cumulative incidence of CHF was 5.4 percent (492 events). Participants with retinopathy had a higher incidence of CHF compared with those without retinopathy (15.1 percent vs. 4.8 percent, P<.001). After controlling for age, sex, race, preexisting coronary heart disease, mean arterial blood pressure, diabetes, glucose level, cholesterol level, smoking, body mass index and study site, the presence of retinopathy was associated with a twofold higher risk of CHF. Among participants without preexisting coronary heart disease, diabetes, or hypertension, retinopathy was associated with a threefold higher risk of CHF.
The authors say that microvascular disease may play an important role in the development of heart failure in the general population. Some asymptomatic persons with retinopathy on an ophthalmologic examination may benefit from further assessment of CHF risk.
1. JAMA 2005;293:63-69.
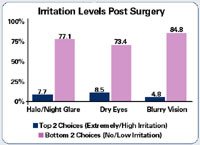
| Refractive Surgery Update | |
|