Presentation
A 5-month-old male presented after his mother noted tearing of the left eye. The patient was initially thought to have a self-traumatized left eye, but the tearing persisted over several days and was accompanied with redness and photophobia. He was subsequently referred by his pediatrician for ophthalmologic evaluation.
Medical History
The patient was status post normal, full-term pregnancy and vaginal delivery without complications. There was a history of possible nasolacrimal duct obstruction that resolved on its own. The patient was otherwise healthy. His mother noted that people often remarked that the child had "beautiful big eyes."
Examination
Examination showed central, steady and maintained fixation in both eyes. Photophobia was present. Pupils were equal with no afferent pupillary defect. Eye movements were full with no strabismus. Tonopen intraocular pressures were 20 mmHg in the right eye and 50 to 60 mmHg in the left eye. These measurements were taken while the child was awake and restless.
Handheld slit-lamp examination showed corneal epithelial edema in the left eye (See Figure 1). Both corneal diameters were enlarged. The right cornea measured 14 mm and the left cornea measured 14.25 mm. Anterior chambers were deep and quiet, and iris morphology was normal in both eyes. Cup/disc ratios were approximately 0.5 in the right eye and 0.6 in the left eye. Retinal examination was otherwise unremarkable. Cycloplegic refraction of the right eye was +1.00 sphere and the left eye was
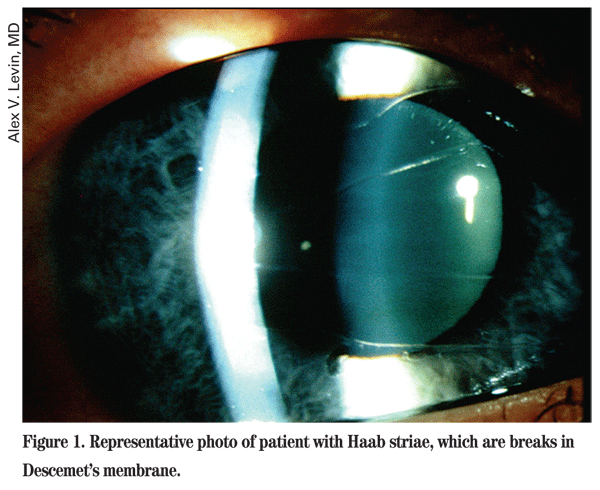
Diagnosis, Workup and Treatment
Epiphora in an infant can result from abnormalities in tear drainage, most commonly nasolacrimal duct obstruction (NLDO), or overproduction of tears, as in the setting of irritation (e.g., trichiasis, foreign body, corneal abrasion), infection and congenital glaucoma. On examination, NLDO typically presents with a white, normal-sized eye with mucoid discharge worse on waking, and this tends to be the predominant symptom in infancy rather than epiphora. The findings of congenital glaucoma include photophobia, corneal edema (epithelial and/or stromal), Haab striae (See Figure 1) and corneal enlargement secondary to stretching from elevated IOP. This may also cause increased axial length, resulting in myopia.
Based on the findings, this patient was diagnosed with primary congenital glaucoma. The patient was started on dorzolamide and timolol 0.25% ophthalmic drops twice daily, as well as oral acetazolamide (15 to 30 mg/kg/day divided into three or four doses daily), in an effort to clear the corneal edema in preparation for surgery. Prior to the procedure, an examination under anesthesia was conducted to confirm the diagnosis.
Tonopen intraocular pressures were 19 mmHg on the right and 14 mmHg on the left. Bilateral nasal goniotomy was performed, and the patient tolerated the procedures well with improvement in symptoms and signs postoperatively. The next examination under anesthesia will be conducted at four to six weeks postoperatively.
Discussion
Primary congenital and infantile glaucoma occurs in approximately one out of 10,000 births in
PCG is thought to be the result of a failure of trabecular meshwork differentiation from neural crest cells, and various structural abnormalities of the angle have been observed, including abnormally anterior insertion of the iris. PCG can also be associated with atrophy of the iris and thinning of anterior sclera (See Figure 2).
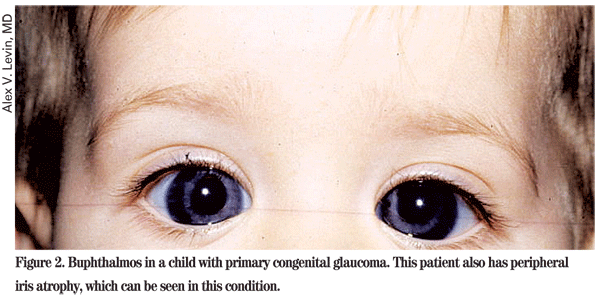
Goniotomy and trabeculotomy are considered first-line therapies of PCG. Both procedures involve opening the trabecular meshwork to establish communication between the anterior chamber and Schlemm's canal. Long-term outcomes of goniotomy and trabeculotomy for the treatment of PCG have been shown to be favorable, and approximately 80 percent of patients who undergo one or two angle surgeries within the first year of life have good IOP control with or without medication.
Traditional goniotomy requires visualization of the angle through a surgical gonioscopy lens and is not ideal in cases with a cloudy cornea. Medical management for two to three days prior to surgery may allow for sufficient corneal clearing to perform goniotomy. If not, one can either perform goniotomy endoscopically or do trabeculotomy, which involves a transcleral approach to cannulate Schlemm's canal. Modifications of trabeculotomy include passing a 6-0 Prolene suture or insertion of a microcatheter through 360 degrees of Schlemm's canal. Endoscopic goniotomy allows a direct view of the angle through an endoscope inserted into the anterior chamber.
Patients who have failed angle surgery can go on to trabeculectomy with or without antimetabolites (mitomycin-C), but this procedure is associated with serious long-term complications, including endophthalmitis. Glaucoma drainage implants have also been used in children with glaucoma refractory to goniosurgery. Adjunctive medical therapy is also often needed in these patients.
This patient had a successful goniotomy procedure, which is indicated as a first-line therapy, but will require close, long-term follow up to monitor IOP and disease control.
The author would like to thank Alex V. Levin, MD, chief of the Pediatric and Ocular Genetics Department at the Wills Eye Institute, for his time and assistance with this case.
1. Ho CL, Walton DS. Primary congenital glaucoma: 2004 update. J Pediatr Ophthalmol Strabismus 2004;41:271–288.
2. Barsoum-Homsy M, Chevrette L. Incidence and prognosis of childhood glaucoma. A study of 63 cases. Ophthalmology 1986;93:1323–1327.
3. Stoilov I, Akarsu AN, Sarfarazi M. Identification of three different truncating mutations in cytochrome P4501B1 (CYP1B1) as the principal cause of primary congenital glaucoma (Buphthalmos) in families linked to the GLC3A locus on chromosome 2p21. Hum Mol Genet 1997;6:641–7.
4. Sarfarazi M, Stoilov I, Schenkman JB. Genetics and biochemistry of primary congenital glaucoma. Ophthalmol Clin North Am 2003;16:543–54, vi.
5. Shaffer RN. Prognosis of goniotomy in primary infantile glaucoma (trabeculodysgenesis). TransAmOphthalmol Soc 1982;80:321–5.
6. Mendicino ME, Lynch MG, Drack A, Beck AD,
7. Ikeda H, Ishigooka H, Muto T, et al. Long-term outcome of trabeculotomy for the treatment of developmental glaucoma. Surv Ophthalmol 2004;122:1122– 8.
8. Kulkarni SV, Damji KF, Fournier AV, Pan I, Hodge WG. Endoscopic Goniotomy: Early Clinical Experience in Congenital Glaucoma. J Glaucoma. 2009 Sep 2. [Epub ahead of print]



