
Presentation
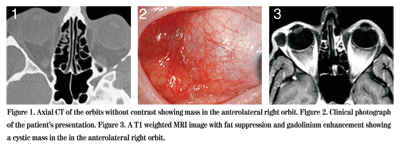
A 43-year-old woman noted swelling and pain around her right eye for two weeks. She denied trauma, visual change or diplopia. Following ophthalmic examination, she was placed on prednisolone acetate and gatifloxacin eye drops every two hours to the right eye. The following day she noted worsening swelling and pain and was started on prednisone 40 mg daily by mouth and amoxicillin/clavulanate three times daily for a potential diagnosis of pseudotumor. CT scan of the orbits, however, revealed a small extraconal mass in the lacrimal gland fossa of the right orbit. Upon follow-up one week later, her swelling had minimally improved. She was referred to the Wills Eye Institute Ocular Oncology Service for further evaluation and management.
Medical History
The patient denied related past ocular history. She had a past history of depression, and there was a family history of pancreatic cancer. She denied constitutional symptoms.
Examination
On examination at the Wills Eye Institute Ocular Oncology Service the visual acuity was 20/30 in the right eye and 20/25 in the left eye. Her pupils were round, equal, briskly reactive, and without a relative afferent pupillary defect. Extraocular motility and confrontational visual fields were full in both eyes. Intraocular pressures were 21 mmHg OD and 13 mmHg OS.
External examination of the right eye revealed a pink, temporal mass in the forniceal conjunctiva, measuring 2.5 x 2.5 x 2.0 cm. There were two components: a superior component which clinically appeared cystic, and an inferior component which appeared more solid. There was no proptosis. The remaining slit lamp and fundus examinations were unremarkable OU. There was no evidence of globe compression right eye. Following her visit with the Ocular Oncology team, an MRI of the orbits was obtained.
Diagnosis and Workup
The cystic mass was clinically suspected to represent a large inflamed dacryops, but adenoid cystic carcinoma of the lacrimal gland could not be excluded. Surgical excision was advised. The patient was taken to the operating room two days after her visit to the Ocular Oncology Service and complete excisional biopsy of the intact mass was performed. Frozen sections revealed benign lacrimal tissue with epithelial cyst and associated acute and chronic inflammation and hemosiderin deposition consistent with dacryops.
The patient was placed on Maxitrol ointment three times daily and her prednisone was decreased to 10 mg daily for four days and then stopped. The patient returned for follow-up two weeks later and was continuing to heal well after surgery. She is followed routinely.
Discussion
Important epithelial lesions of the lacrimal gland include dacryops, pleomorphic adenoma (benign mixed tumor), and malignant epithelial tumors including adenoid cystic carcinoma, mucoepidermoid carcinoma, and pleomorphic adenocarcinoma (malignant mixed tumor). In a histopathology review of 142 consecutive biopsies of lacrimal gland tumors, 22 percent were epithelial lesions and 78 percent were nonepithelial lesions, mainly inflammation and lymphoid tumors. Dacryops accounted for 6 percent of cases in this series. In a recent clinical series of 1,264 consecutive patients with orbital tumors, lacrimal gland lesions accounted for 114 (9 percent), and there were 19 cases of dacryops (2 percent of total).
Dacryops is a cyst of the lacrimal gland duct and presents typically in young adults and middle-aged patients with female predominance. Dacryops usually arises from the palpebral lobe of the lacrimal gland. It presents as a mass in the superotemporal conjunctival fornix, developing spontaneously, following an episode of dacryoadenitis, or more rarely following conjunctival inflammatory or scarring conditions such as trachoma, ocular cicatricial pemphigoid, or trauma.
Dacryops is usually painless, but can become inflamed and tender. Due to slowly progressive mass effect of the enlarging cyst, the globe can be displaced and motility can be restricted. The etiology of dacryops is unclear. One proposed mechanism is that inflammation around the tear ducts or trauma to the tear ducts might cause hypersecretion of tears, destroy the contractility of the duct, weaken the walls, constrict the forniceal opening, and lead to passive dilation of the duct with cyst formation.
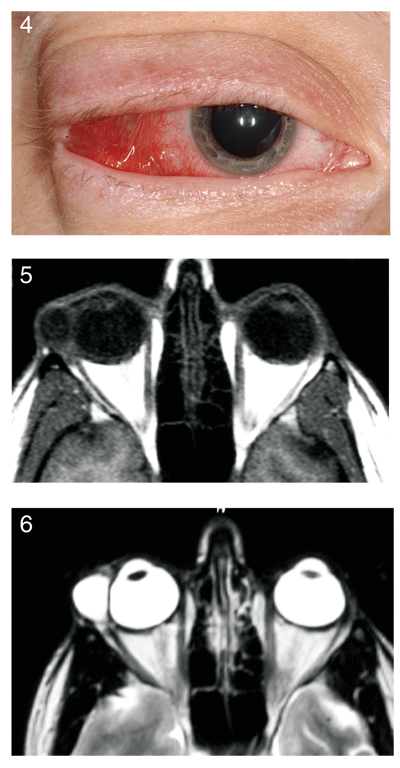
Figure 4. Another view of the patient"s presentation. Figure 5. T1 weighted MRI image with no fat suppression. Figure 6. A T2 weighted image.
The natural history of lacrimal dacryops is slow, progressive enlargement. Occasionally mild cases can show spontaneous resolution. Cases have been reported in which dacryops converted to mucoepidermoid carcinoma or squamous cell carcinoma. Dacryops can occasionally become infected as well, leading to painful enlargement.
Computed tomography (CT) or magnetic resonance imaging (MRI) of the orbits will typically reveal a cystic mass in the region of the lacrimal gland with absence of invasion of neighboring structures or bone. The definitive diagnosis is made histopathologically where a cyst is present with one or two layers of epithelium and a clear lumen.
Treatment for symptomatic dacryops often involves local resection through a superotemporal conjunctival forniceal approach as was done in this case. Care must be taken to avoid destruction of the remaining tear ducts that drain the palpebral lobe. Some dacryops will resolve with topical antibiotic/steroid ointment. Simple puncture and aspiration of the cyst can be performed to fistulize the cyst onto the conjunctival surface but closure and recurrence is a problem. Some authors have used blue-green argon laser to open and fistulize the cyst. Smaller cysts that are asymptomatic can be observed.
Dr. Fenton would like to thank Carol Shields, MD, of the Ocular Oncology Service at Wills Eye Institute, for her assistance with this case.
Shields JA, Shields CL, Scartozzi R. Survey of 1264 patients with orbital tumors and simulating lesions: The 2002 Montgomery Lecture, part 1. Ophthalmology 2004;111:997-1008.
Shields CL, Shields JA, Eagle RC Jr, Rathmell JP. Clinicopathologic review of 142 cases of lacrimal gland lesions. Ophthalmology 1989; 96:431-35.
Shields JA, Shields CL. Atlas of orbital tumors. Lippincott Williams and Wilkins, 1999: 174.
Betharia SM, Pushker N, Sharma V, Sen S. Simple dacryops: a case series and review of the literature. Ophthalmologica 2002;216:372-6.



