Presentation
A 24-year-old woman presented to a local emergency department complaining of visual loss in the right eye over the previous couple hours with associated mild pain. She reported having had a similar episode six years ago in the same eye that spontaneously resolved.
Medical History
She denied any past medical history, had no known drug allergies and took no medications.
She did not smoke, drink alcohol or use intravenous drugs. She was born in Mexico and had no significant family history of ophthalmic or medical disease. Review of systems was significant for a recent viral upper respiratory tract infection.
|
Examination
Her ophthalmic exam in the emergency department revealed an uncorrected near visual acuity of 20/70 OD and 20/20 OS. Her pupils were round, equal, briskly reactive and without a relative afferent pupillary defect. Extraocular motility and confrontational visual fields were full in both eyes. Intraocular pressures were 17 mmHg OD and 16 mmHg OS. Color plate testing was full, and there was no subjective color or light desaturation. Amsler grid testing elicited an inferonasal field defect OD.
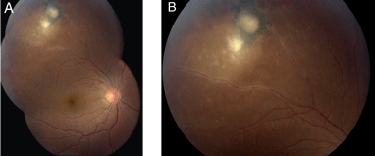
Slit-lamp biomicroscopy revealed trace conjunctival injection, fine keratic precipitates and 1+ anterior chamber white blood cells and flare OD. The left eye was white and quiet anteriorly. Her dilated fundus examination OD revealed a healthy optic nerve and macula. However, there were fine precipitates along the posterior hyaloid face OD with lesions in the superotemporal periphery (See Figures 1a and 1b). Fundus examination OS was unremarkable.
What is your differential diagnosis? What further workup would you pursue?