
Presentation
A 26-year-old Caucasian male presented to the Wills Eye Emergency room complaining of blurred vision in his left eye for two weeks. He described one day of fevers and chills soon after his release from prison four weeks previously. He developed throbbing pain and floaters with progressively worsening vision in his left eye.
Medical History
The patient denied past medical problems, medication use or family history of disease. He admitted to heroin and alcohol abuse.
Examination
Emergency room visual acuity was 20/30 in the right eye and 20/400 in the left. Intraocular pressures were 13 mmHg in both eyes. Pupils were brisk, without a relative afferent pupillary defect.
Confrontational fields were full with the exception of a central scotoma in the left eye. Slit-lamp examination of the anterior segment was normal in both eyes, as was the dilated fundus examination in the right eye. The left posterior segment revealed a mild to moderate vitritis. A raised white chorioretinal lesion was located within the fovea (See Figure 1); fluorescein angiography demonstrated late staining (See Figure 2).
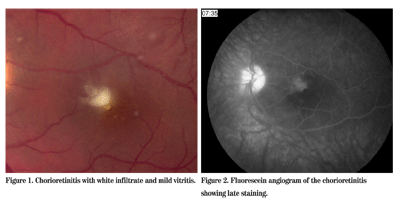
Diagnosis and Workup
The differential diagnosis for a white chorioretinal lesion with an associated vitritis includes candida, toxoplasma, bacteria (e.g., staph), tuberculosis, syphilis, Lyme disease, HIV, sarcoid and toxocara. Pertinent details of this case included intravenous drug abuse, recent incarceration, and transient fevers and chills. The Wills ER doctors performed the appropriate laboratory and imaging tests to pursue the differential diagnosis. These tests included a toxoplasma IgG and IgM, complete blood count with differential, PPD and chest X-ray, RPR, Lyme titers, HIV, ACE and toxocara IgG. All tests, including four blood cultures, urine culture and echocardiogram, were negative.
The patient was admitted with a presumptive clinical diagnosis of candida chorioretinitis secondary to intravenous drug abuse. After consulting infectious disease, the patient was given two doses of intravenous voriconazole, and then subsequently switched to oral voriconazole. Within two days, his symptoms and visual acuity improved significantly.
He was discharged on oral voriconazole, with follow-up arranged with Wills Eye Institute, infectious disease and drug rehabilitation. Despite numerous phone calls, he was lost to follow-up for three weeks and discontinued his oral voriconazole treatment. He returned with decreased vision to counting fingers at 2 feet. Fundus examination revealed a denser vitritis, epiretinal membrane and macular pseudohole (See Figure 3). 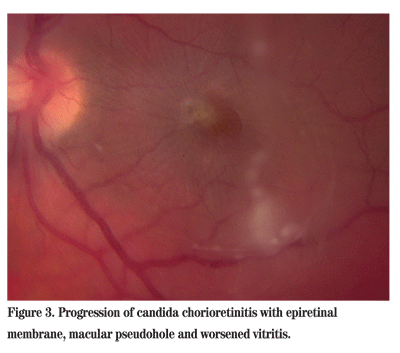
Symptoms began to improve after one week with improved access to medications and compliant follow-up.
Discussion
Ocular candidiasis defines a disease spectrum from chorioretinitis to endophthalmitis. Candida chorioretinitis manifests as white infiltrates associated with minimal to no vitritis. These infiltrates may progress to endophthalmitis, marked by vitritis and vitreal snowballs. Patients with this degree of inflammation often describe floaters and decreased visual acuity. Complications of advanced disease include epiretinal membrane, subretinal abscess, macular hole, retinal necrosis and retinal detachment.
Ocular candidiasis may be endogenous or exogenous in etiology. Endogenous fungal endophthalmitis is spread hematologically, and can be introduced by intravenous drug abuse. Risk factors include indwelling catheters, broad spectrum antibiotics, parenteral hyperalimentation, immunocompromised state and debilitation. Other manifestations of candidemia include endocarditis, cystitis and meningitis. Exogenous fungal endophthalmitis involves direct inoculation of the eye, most often after cataract surgery with or without lens implantation.
For inpatients with candidemia, the prevalence of candida chorioretinitis is low, with recent studies reporting rates between 2 and 9 percent. Rates of endophthalmitis are even lower. Outpatients, on the other hand, tend to present with more advanced stages of disease. This disparity between inpatients and outpatients may be explained by differences in monitoring and timeliness of antifungal therapy.
The diagnosis of ocular candidiasis is largely clinical, as blood and urine cultures can be negative. In the setting of vitritis, a vitreous biopsy can confirm the diagnosis.
Treatment should be initiated promptly with close monitoring. Several medications and approaches can be considered. Chorioretinitis can be treated with systemic antifungals alone, including amphotericin B (with or without flucytosine), fluconazole or voriconazole. Amphotericin B obtains good concentration in the retina and choroid, but not in the vitreous. Fluconazole, a first-generation triazole, achieves higher vitreous concentration than amphotericin.
More recent evidence suggests voriconazole, a second generation triazole with 96 percent bioavailability, may be effective. With significant vitritis, consider adjunctive intravitreal amphotericin B. Endophthalmitis often requires vitrectomy with intravitreal amphotericin B.
Dr. Shah is a second-year resident at



