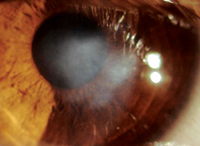
Presentation
A 67-year-old Caucasian male presented to a general ophthalmologist's office for a routine eye exam. He denied pain, visual loss or any other ocular complaints. He had never seen an ophthalmologist or optometrist for a complete eye exam.
Medical History
The patient's past medial history was noncontributory. He denied having diabetes, hypertension, or any other medical condition. He did not take any medicine on a regular basis except for a daily multivitamin, chromium supplements and vitamins A, C and E. He had no known drug allergies. Family history was negative for glaucoma or macular degeneration. He denied smoking and the use of alcohol or intravenous drugs. Review of systems was negative.
Examination
Office examination revealed an uncorrected visual acuity of 20/20 in the right eye and 20/20 in the left eye. Pupillary reactions were brisk in each eye with no relative afferent defect. Extraocular motility and confrontational visual fields were full in both eyes. Intraocular pressures by applanation tonometry were 15 mmHg in the right eye and 18 mmHg in the left eye. Slit-lamp biomicroscopy revealed quiet anterior segments bilaterally. His dilated fundus examination was normal with the exception of optic nerve rim thinning bilaterally. Central corneal thicknesses were obtained and measured 505 µm in the right eye and 511 µm in the left eye.
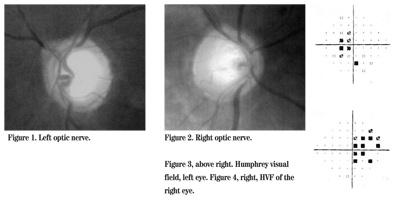
At that time, fundus photographs and 24-2 Humphrey visual fields (HVF) were obtained for both eyes (See Figures 1, 2, 3 and 4).
Diagnosis and Workup
The patient was diagnosed as a normal tension glaucoma suspect and subsequently referred to a glaucoma specialist for further evaluation and treatment. After discussing the risks and benefits of several options, it was decided that argon laser trabeculoplasty was the best treatment modality. As a result of this procedure, the IOP dropped by 3 mmHg in the right eye and 2 mmHg in the left. Despite close follow-up, stable optic nerve appearance, and good control of his intraocular pressures, the patient's visual fields showed gradual progression over the next four years.
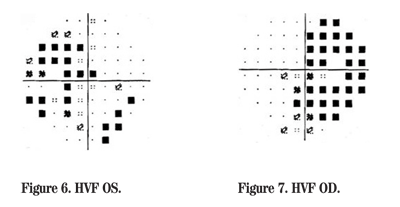
The patient was then lost to follow up for approximately two years. Toward the end of that two-year period, a syncopal workup was done following a Transurethral Resection of the Prostate procedure (TURP) and it revealed a pituitary adenoma on brain imaging (See Figure 5). Humphrey visual field testing was obtained shortly after the incident (See Figures 6 and 7), and demonstrated classic bitemporal field loss consistent with a chiasmal syndrome.
Discussion
Lesions producing a relative or absolute bitemporal hemianopia, without affecting central vision, can be localized to the mid or posterior optic chiasm, as this case illustrates. The differential diagnosis for lesions producing a chiasmal syndrome includes pituitary adenoma, parasellar meningioma, craniopharyngioma, parasellar internal carotid artery aneurysm, chiasmal glioma, abscess, and inflammatory, metastatic or demyelinating lesions.
In chiasmal syndromes, the optic discs may show no visible abnormalities initially, even if significant visual field changes are seen. There may be subtle signs of optic neuropathy such as mild disc pallor or peripapillary retinal nerve fiber layer dropout. Over time, the optic discs may show an increase in atrophy and subsequent cupping. Visual field defects may include bitemporal hemianopia, central scotoma, junctional scotoma and incongruous homonymous hemianopia.
Pituitary adenomas are the most common lesions to cause chiasmal compression and can occur at any age in the adult. Approximately one-third of all adenomas are clinically non-functioning, and may remain undetected until quite large. Unlike hormone-secreting tumors that are often detected at a smaller size, patients with these null cell adenomas often present with visual loss. Pituitary adenomas in men are usually prolactin-secreting and may present with decreased libido and impotence. In women, pituitary tumors may expand during pregnancy and produce chiasmal compression.
Pituitary apoplexy is a syndrome that occurs when acute hemorrhage occurs into a pituitary tumor with resultant severe headache, bitemporal hemianopia and diplopia if the third, fourth or sixth cranial nerves are affected.
Pituitary tumors may be treated with observation only, surgery (transsphenoidal or transfrontal), medical therapy (for secreting tumors), and irradiation. Visual recovery following surgical resection of the tumor is rapid, whereas progress following medical therapy is slow. Visual field and acuity testing should be performed two to three months following treatment and every six to 12 months thereafter. Follow-up neuroimaging should also be instituted.
Follow up and Conclusion
The patient underwent successful transsphenoidal removal of his pituitary macroadenoma. Follow-up visual field testing showed an improvement in his visual field defects that have since remained stable.
This case demonstrates that bilateral visual field loss, whether symmetric or asymmetric, should prompt the clinician to carefully evaluate the perimetry for defects that obey the vertical midline. A low threshold for neuroimaging should exist for any visual field changes consistent with chiasmal syndrome, especially in those patients being treated for glaucoma.
Dr. Shelsta is a second-year resident at Wills Eye Hospital.