
Presentation
A 56-year-old woman presents with the complaint of progressively decreasing vision in both eyes over the past three years. She had LASIK surgery performed in both eyes seven years ago for refractive errors of -10.5 D in each eye, and saw well in subsequent years. She now finds it increasingly difficult to read and watch television. Her past medical and family histories are noncontributory, and a review of systems is negative.
Medical History
Visual acuity with spectacles (-1.00 -0.75 x 180° O.D. and -2.00 -1.00 x 65° O.S.) is 20/60 in each eye. A +2.00 add O.U. allows her to read Jaeger 1 O.D. and Jaeger 3 O.S. Pupillary examination, extraocular movements, visual fields, and intraocular pressures are normal in each eye. Slit-lamp biomicroscopy reveals quiet anterior segments bilaterally. The LASIK flaps are well-positioned with pristine interfaces. There are moderate nuclear sclerotic changes in both eyes, left eye worse than the right. The dilated fundus examination is normal in both eyes.
Examination
After the risks, benefits and alternatives are discussed, phacoemulsification and intraocular lens (IOL) implantation, beginning with the left eye, is agreed upon. Her corneal power is estimated using the clinical history method.1,2 Prior to LASIK the spherical equivalent of her refractive error was -10.5 D with an average keratometry measurement of 45.00 D. Following LASIK and prior to the development of cataracts her refraction was stable at -1.00 D. Using the formula: Kp + Rp – Ra = Ka, where Kp is the average keratometry power prior to LASIK, Rp the spherical equivalent of the refractive error prior to LASIK, and Ra the spherical equivalent after LASIK, the estimated central corneal power after LASIK, or Ka, is 35.5 D. Axial length is 30.10 mm by immersion A-scan ultrasonography. The SRK/T formula is used to determine the appropriate IOL power, with the goal of zero refractive error.
Course
She undergoes uneventful cataract extraction with implantation of an SI40NB +13.00 D lens (AMO, Santa Ana, Calif.). She experiences a normal postoperative course. The IOL is well-centered within the capsular bag, and her visual acuity is 20/30. However, her refractive error is now +4.00.
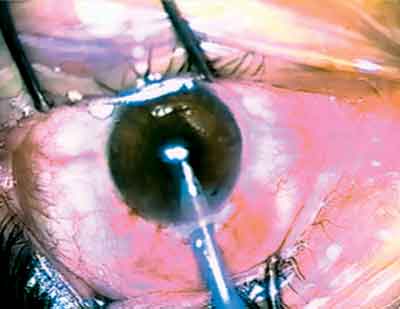
What went wrong? What is the most accurate way to determine intraocular lens power in post-photorefractive patients? Please turn to p. 110
Discussion
The patient experienced a "refractive surprise" due to a miscalculation of IOL power. Unfortunately, this is not uncommon due to the limitations of keratometry and IOL calculation formulas in post-LASIK eyes.
Keratometry assumes the posterior radius of curvature is 80% the anterior radius of curvature. This ratio changes after LASIK, since only the anterior radius of curvature is altered during photoablation.3 Also, keratometry measures the power of the cornea in the paracentral area, not the visual axis. In normal eyes the cornea is relatively spherical and this off-axis measurement is of little consequence. However, this approximation is less accurate after LASIK due to the flattened central cornea. These keratometric assumptions overestimate the true corneal power and result in implantation of an IOL of insufficient power.
When historical data is available, the clinical history method may be used to estimate true corneal power as in this case.1,2 Refractions are converted for the corneal plane, although some surgeons (as in this case) choose not to, in order to allow extra buffer for the prevention of hyperopia. The IOL power adjustment method also uses historical data.4 Other methods that do not rely on historical data have been described in the literature.5-7 Each of these formulas increases the accuracy of IOL calculation, but are still limited. Since the true central corneal power cannot be directly measured it may be best to apply several formulas and choose the one with the lowest corneal power measurement. This too will help prevent a hyperopic surprise. The Pentacam by Oculus Inc. (Lynnwood, WA, oculususa.com) and similar technologies may more accurately determine corneal power since they are able to measure both the front and back radii of curvatures. Hopefully, these technologies will help reduce the guesswork for determining corneal power.
The third generation formulas such as the SRK/T, Hoffer Q and Holladay 1 use only two variables for calculating IOL power. Based on regression analysis they assume the anterior and posterior segments of the eye are proportional and a relatively accurate effective lens position (ELP) is calculated. However, the flattened cornea of the post-LASIK eye results in a calculated ELP that is more anterior than the actual ELP. Unless the formula is adapted to better predict the actual ELP this will also result in hyperopia.8 The "Double K" method is one such adaptation, but was not used in this case. Had it been used the refractive error would have still been hyperopic although not as much (+2.50 D instead of +4.00 D). Alternatively, the Holladay 2 formula may be used. It employs more variables such as horizontal corneal diameter, lens thickness, preoperative refraction and patient age, in addition to keratometry and axial length to achieve a more accurate ELP in post-LASIK eyes. However, for this eye the Holladay 2 formula would have also suggested a +13.00 IOL.
In post-LASIK cases as with any case it is important to obtain accurate biometry. Our patient had an unusually long axial length by immersion A-scan ultrasonography. This may have been the measure of the anatomic axial length rather than the refractive axial length which are not always equal.3 If so, this could also contribute to a hyperopic refractive error if the refractive axial length is indeed shorter. For example, if the refractive axial length of this patient was 27.6 mm instead of 30.10 mm, the suggested IOL power by SRK/T would have been +19.00 D instead of +13.00 D. Optical coherence biometry (IOLMaster, Carl Zeiss Meditec, Jena, Germany) may help solve this problem since it depends on foveal fixation and has greater accuracy for determining axial length.
Another option for cases with difficult IOL calculations is to bypass the keratometry, biometry, and IOL calculation formulas altogether. This method involves extracting the cataract then refracting the eye in the same surgical setting to determine the IOL power needed to correct for the aphakia.9 The patient is then reprepped and draped and the calculated IOL implanted.
In cases more likely to require a secondary procedure (i.e., IOL exchange or piggyback IOL), the surgeon should consider using a silicone lens implanted in the capsular bag during the initial cataract extraction. A silicone lens is more easily exchanged than a lens made of acrylic material.10 Moreover, should a piggyback IOL be considered, either a silicone or acrylic lens may be used over the primary silicone lens. This will help lessen the risk of interlenticular opacification, which has been observed when an acrylic lens is piggybacked over a lens of the same material.11
Follow-up and Conclusion
Management options of refractive surprises include spectacles, contact lenses, repeat LASIK, conductive keratoplasty, photorefractive keratectomy, IOL exchange, or a piggyback IOL. After a thorough discussion of the advantages and disadvantages of each procedure it was decided to exchange the intraocular lens. To correct for +4.00 D of hyperopia, the error was multiplied by 1.5.3 The +13.00 D lens was removed from the capsular bag and replaced with an SI40NB +19.00 D lens. Her post operative visual acuity was 20/25 with zero refractive error.
Accurate IOL calculation in patients with previous keratorefractive surgery is a growing problem. A number of formulas have been developed, and have been successful to a degree. However, refractive surprises still occur despite best efforts. This necessitates more study in this area before consistent results can be obtained in these challenging patients. This case illustrates the importance of proper patient counseling regarding the difficulty of calculating IOL power after LASIK, the anticipation of requiring an additional procedure, and the proper management of the refractive surprise.
Dr. Smith, a former Wills resident, is a retina fellow at Barnes Retina Institute, St. Louis. Dr. Hannush is an attending surgeon on the Cornea Service at Wills, an assistant professor of ophthalmology at Thomas Jefferson University and in private practice in Langhorne, Pa.
1. Holladay JT. Consultations in refractive surgery. Refract Corneal Surg 1989; 5:203.
2. Hoffer KJ. Intraocular lens power calculation for eyes after refractive keratotomy. J Refract Surg 1995;11:490- 493.
3. Hill WE, Byrne SF. Complex Axial Length Measurements and Unusual IOL Power Calculations. Focal Points: Clinical Modules for Ophthalmologists. 2004;22:1-18.
4. Feiz V., Mannis M.J. Garcia-Ferrer F. Intraocular lens power calculation after laser in situ keratomileusis for myopia and hyperopia a standardized approach. Cornea 2001;20:792-797.
5. Koch, D., Wang I. Calculating IOL power in eyes that have had refractive surgery. J Cataract Refract Surg 2003;29:2039-2042.
6. Wang L, Booth MA, Koch DD. Comparison of intraocular lens power calculations methods in eyes that have undergone LASIK. Ophthalmology 2004;11110);1825-1831.
7. Haigis W. Corneal power after refractive surgery for myopia: contact lens method. J Cataract Refract Surg 2003;29:1397-1411.
8. Aramberri J. Intraocular lens power calculation after corneal refractive surgery: Double K method. J Cataract Refract Surg 2003;29:2063-2068.
9. Mackool RJ. The cataract extraction-refraction-implantation technique for IOL power calculation in difficult cases. J Cataract Refract Surg. 1998;24:434-5.
10. Voros GM, Strong NP. Exchange technique for opacified hydrophilic acrylic intraocular lenses. Eur J Ophthalmol. 2005;15:465-7.
11. Trivedi RH, Izak AM, Werner L, et al. Interlenticular opacification of piggyback intraocular lenses. Int Ophthalmol Clin. 200;41:47-62.



