No matter how long lasik endures, surgeons can still come up with ways to make it faster, safer or better. Here are 10 pearls to improve your LASIK from preop to postop from several experienced surgeons:
1. Preop medication. "I use a fourth-generation fluoroquinolone and steroid q.i.d. for the three days prior to surgery," says
To head off surface issues, Dr. Stonecipher uses Restasis one to two weeks preoperatively, and then starts it again the day after surgery and continues it for one to two months or longer depending on the patient's symptoms.
2. LADARVision ablation depth estimation. With Alcon's LADARVision system, the surgeon only really knows how much tissue the laser plans to remove on the day of surgery when the patient is dilated, his wavefront is imaged and that's fed into the surgical planning software. Unfortunately, if it estimates that it will remove too much, the surgeon may have to tell the patient, on the day of his surgery, that he can't have LASIK. Michael Taravella, MD, national medical director of Clearvision Laser Centers, says he's developed a way to estimate the depth before the day of surgery. "We take the total root mean square of the patient's higher-order aberrations and feed it into a regression formula we've developed [he will present a poster at the 2007 American Society of Cataract and Refractive Surgery meeting explaining the formula]," he says. "This always gives us the amount of tissue the laser will ablate, within 5 µm."
3. Mental preparation. Elizabeth Davis, MD, of
4. Avoid transcription errors. Dr. Taravella says that, for standard treatments, he always tells his residents and fellows to "work backward" when changing plus cylinder to minus cylinder notation to avoid transcription errors when planning an ablation. "You change the cylinder axis 90 degrees first," he explains. "Then change the sign of the cylinder. Last, you add the sphere and cylinder to come up with the sphere." For example, say the refraction is -1 +2 x 85. First, the surgeon changes the axis by adding 90 degrees, changing it to 175. He then changes the cylinder sign to minus. Then, when the sphere and cylinder are added, the sphere becomes +1. So, in minus cylinder, the refraction becomes +1 -2 x 175.
"If you're doing custom, you won't get a transcription error," says Dr. Taravella, "as long as you get the right floppy disk [or whatever medium the patient file is on] for the right patient."
5. Individualize monovision.
"First, I put the distance correction in both eyes, then try a mild amount of monovision in the left eye and then the right, letting the patients pick which way they prefer the monovision. If they hate it, then we don't go any further. If they think it's OK, I'll determine if they like the left eye for near or the right, and then will try different strengths of monovision. For these tests, they put on trial frames and walk around the office, then come back and tell me what they prefer the most. We encourage them to look far and near. It's very individualized—some people like the non-dominant eye to be for distance.
"I've found this system works very well. If the patient has tried all the possibilities, he will feel that he has all the options to choose from, and understands a topic that can be confusing." Dr. Caster handles the testing. "Time spent in the chair in advance will save countless hours of trying to help disappointed patients afterward," he avers. "It's rare that we have a disappointed patient."
6. Proper positioning. "Make sure the patient's chin and brow are even," says Dr. Taravella. "The chin shouldn't be tilted too far up or down. This really becomes important when you're dealing with trackers and iris registration, because you don't want shadows that can confound these devices. A deep-set eye can also confuse both a tracker and registration in some instances."
7. Managing the microkeratome. When Dr. Davis is ready to make the flap cut, she steps on the foot pedal for a moment, advancing the blade, then releases the pedal before the blade engages the cornea. "What this often does is cause the patient to jump from the initial buzz," she says. "I can then proceed forward with the cut without him jumping while I've engaged cornea." When the flap's made, she removes suction on the reverse pass to help decrease the frictional forces on the flap, with the goal of minimizing epithelial defects.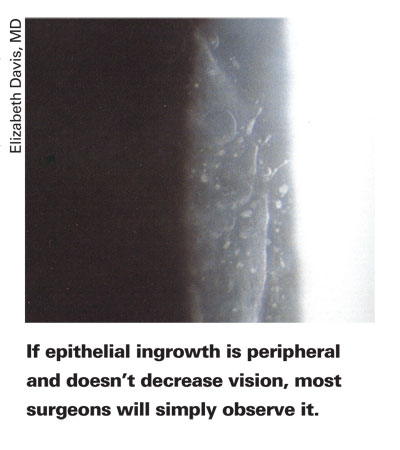
8. Take intraoperative pachymetry. Dr. Taravella uses a DGH pachymeter intraoperatively, and his staff calibrates the device each day. "If the first flap is thinner than we anticipated, we switch blades before doing the second eye," he says. "For instance, if we use a 140-µm depth plate but the first flap is 120-µm thick or less, we'll change blades for the next eye, because the next flap, if we use the first blade, will be 10 to 15 µm thinner. I personally don't like to deal with 100- or 90-µm flaps, because they're more prone to striae."
9. Epithelial issues. "If I have an issue with epithelial defects or loose epithelium, I'll put the patient in an extended-wear contact lens and leave it in as long as he can tolerate it," says Dr. Stonecipher. "This is effective because usually the reason for the problem is subclinical Bowman's membrane dystrophy, recurrent erosion or some type of previous trauma in that location of the cornea. I'll even leave the lens in place for longer than the typical day or two, sometimes leaving it there for four to five days to let the epithelium heal." He will also put in 60-day collagen plugs to ensure that the eye stays moist even after he removes the contact lens.
10. Preventing DLK. Dr. Taravella has a protocol and cleaning regimen his staff uses to prevent cases of diffuse lamellar keratitis. "We use sterile distilled water in our StatIM steam sterilizer rather than just distilled water," he says. "Unsterilized distilled water can have bacteria. Even though these bacteria die in the sterilizer, if you have a lot of dead bacteria floating around in the water, and it creates a biofilm that coats your instruments and the insides of your cannulas, that can certainly be a cause of DLK.
"The other thing we do is vacuum out and air dry our sterilizer once a week to make sure it's perfectly dry, which removes the water-loving bugs. We also use disposable cannulas to avoid any risk of biofilm buildup inside cannulas we're using. Last but not least, we filter any fluid that goes under the cap with a micropore filter that filters down to 0.022 µm, which should get rid of any dead bacteria."
1. Dougherty PJ. The thin-flap LASIK technique. J Refract Surg 2005;21:5:S650-4.