Alicante,
Sometimes a cure is worse than the disease, and sometimes the cure causes the disease, as is often the case when we lift a LASIK flap to clean out epithelial ingrowth; we may wind up creating the very conditions the cells need to infiltrate the flap interface again. In an effort to avoid flap lifting for the treatment of epithelial ingrowth, I looked to a familiar device, the YAG laser, to provide a conservative, less-invasive option. Here's how my YAG technique works and the results I've achieved with it in my practice.
The Technique
When I considered the problem of finding an ingrowth treatment that didn't involve lifting the flap, I gravitated toward the YAG. I thought the YAG might be useful because the manner in which it delivers its laser energy is very focal and localized, which minimizes any collateral damage to surrounding tissue.
My first successful cases with the YAG technique were isolated islands of epithelial ingrowth, which proved that the device could destroy the cells precisely with low-energy shots. I also found that the YAG induced apoptotic changes in the surrounding unwanted epithelial cells due to the shock wave from the impact, even if the cells weren't directly hit. We found that, due to the focal nature of the YAG, it could destroy targeted cells precisely and, in addition, once the cells disappeared, the topography changes disappeared as well. We also found that if we treated ingrowth as soon as it was visible we could even close the fistula, the area of the flap connecting the epithelium to the interface from which most of the cells migrate. This gave us confidence that we could treat the ingrowth cases that had already relapsed several times, without having to relift the LASIK flap.

The technique involves first anesthetizing the eye with a topical drop, then focusing the YAG laser slit lamp on an area of epithelial ingrowth. We set the laser at an energy level that's as weak as possible but which still creates a bubble when applied to the cornea.
We found this level to be, on average, about 0.6 mJ. The spot size is 8 µm or the minimum size the given YAG laser can create, focused at the nest of the epithelium.
Also, you don't need to make another impact confluent with the first. Instead, start in the center of the ingrowth and then move the laser spot a little farther away. Initially, we used a confluent treatment pattern with the bubbles, but we've since found that the epithelial cells disappear without having to connect the bubbles, possibly due to the effects of the laser's shockwave from the individual impacts. This is actually an advantage, since fewer spots mean less of a wound-healing reaction, and even though this reaction was mild when we did more spots, fewer spots are even better for the patient. Also, we'll apply some spots to the fistula where we believe the cells are gaining entrance to the interface in an effort to seal it off. In cases of previous relapses of ingrowth in which the patient was treated with a flap lift, we'll apply the YAG about five days later at the level of the fistula that we identified prior to lifting the flap, in an attempt to seal off the route the cells were taking to gain access to the interface.
Postop, we send the patients home with a mild steroid, such as FML, that they take t.i.d. or q.i.d. for three days to modulate the minor inflammatory reaction that may occur at the interface. It takes about three weeks for the cells to disappear, and we schedule the patient for a visit every three to five weeks. We treat any remaining cells with slightly less energy and fewer treatment spots.
The Results
In a small study of the technique, we used the YAG on 30 eyes of 20 patients with epithelial ingrowth.1 Three of the eyes' ingrowth occurred after a primary LASIK, while the rest developed it following a retreatment. The ingrowth was central in 10 of the eyes and peripheral in the rest. In the latter group, it was causing glare, halo and some irregular astigmatism on topography. Forty percent of the cases (12 eyes) required two or more additional YAG treatments.
Post-treatment, the corneal topography and subjective visual symptoms improved in all cases. The opacities caused by the ingrowth resolved in 80 percent of the cases (24 eyes). In the remaining 20 percent, a small opacity remained in the treatment area, though it was different from haze or epithelial ingrowth. No one lost any lines of vision and, in 60 percent (18 eyes), acuity improved by at least a line. Even in the cases in which acuity didn't improve, the patients reported an improvement in visual quality and we observed an improvement in corneal regularity.
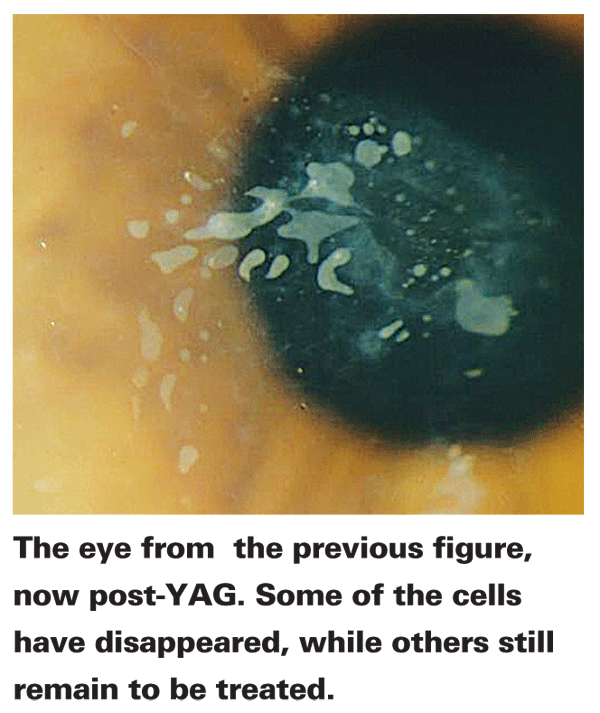
Currently, we feel that the results from using this treatment in our everyday practice may be better than those we achieved in the study because that paper included almost every case of epithelial ingrowth we received at our office, including some that already had corneal scarring due to ingrowth and that had already been through several rounds of flap relifts. The YAG procedure won't treat this scarring and can, in fact, cause the scarring to worsen. However, in the study, even though these patients' acuities didn't improve, their cells disappeared. Now, we don't include such cases in our YAG treatment group. In fact, we hope catch them early in the first place before they get that bad. Such cases are very few in number, however, and we wonder if they might be amenable to some other form of treatment, since the YAG treated them with anatomic success but didn't enjoy equal success in improving their vision.
We have yet to encounter a complication from the YAG treatment for ingrowth, though some patients experience a few hours of photophobia afterward.
The cases that are referred to us are usually for the first recurrence of ingrowth. These actually do the best with the technique, since we can treat the ingrowth without lifting the flap and thus we avoid setting up the conditions amenable to another recurrence.
The occasional case that, in the past, required a flap elevation is now treatable without sutures by ablating the fistula a few days after the relift.
We now use the YAG technique for virtually all of the instances of epithelial ingrowth that we see, and it's a very flexible method for improving outcomes in these patients without lifting their flaps. Patients like it because they don't feel anything and don't need to go to the operating room, and we, as surgeons, like it because it doesn't cost us anything extra, since it's just a new use for an existing piece of equipment. If you decide to try the YAG technique for your cases of epithelial ingrowth, we hope you meet with as much success as we have.
Dr. Alio is a professor and chairman of ophthalmology at
1. Ayala MJ, Alio JL, Mulet ME, De la Hoz F. Treatment of laser in situ keratomileusis interface epithelial ingrowth with neodymium:yttrium-aluminum-garnet laser. Amer J Ophthalmol 2008;145:4:630-634.