The Need to Enhance
Surgeons say the need for precision stems from both the characteristics of these lenses, and the type of patients who get them.
"Certainly, with multifocal lenses and these patients who desire a good refractive outcome, it's more important that the refractive outcome be more or less precisely on target," says Minneapolis surgeon Elizabeth Davis. "Both the vision with the multifocal implant and the patient are less forgiving of a slight refractive error. This is because with multifocal implants there is a little bit of a compromise in the quality of vision. If you compound that compromise with some refractive error, it makes it that much worse than a monofocal lens in which the quality of vision is very good and which doesn't induce a loss in contrast sensitivity. But then, additionally, if you have a patient who is paying extra money and expecting a particular refractive outcome, he's probably going to be less forgiving of a slight refractive error than someone with a standard monofocal IOL."
Surgeons who enhance patients after they receive presbyopic lenses say it's a decision that originates from a patient's complaint.
"There has to be a patient complaint," says Dr. Davis. "If they're unhappy, and you feel it's due to some myopia or hyperopia, even if it's 0.5 D, I'd consider it. In terms of astigmatism, anything 0.75 D or greater could have an impact, and I'd consider it then. But it would be a correlation between what I found on the refraction and the patient complaint."
Planning the Procedure
Dr. Davis says that she has implanted about 50 ReStor lenses, 50 of the ReZoom and between 150 and 200 Crystalens implants. If a patient is going to need his refraction honed postop, she usually is aware of it ahead of time.
"Between 10 and 20 percent of presbyopic lens patients need some type of enhancement," she says. "The majority of these are known beforehand, and consist of significant preop astigmatism of around 3 D or the like. I let the patient know ahead of time that we'll need to come back and do some correction afterward." Dr. Davis' procedure of choice is LASIK for these enhancements. She says she feels LASIK is more precise than incisional surgery, and can handle under- and overcorrections, as well as cylinder.
Michael Colvard, MD, of Fresno, Calif., also implants presbyopic lenses, and plans for their acuity enhancements similarly.
"Generally, the goal with the multifocal lenses ReStor and ReZoom is to aim for a slightly hyperopic result in the range of +.25 D to +.50 D," says Dr. Colvard. "With the Crystalens, the goal is generally to produce a plano or slightly myopic result."
Dr. Davis' goals are similar, though she feels the ReZoom's near point is in a good enough place to shoot for emmetropia with it. For the ReStor, she targets +.25 D or +.50 D in order to push the near point out a bit, and she shoots for -.50 D to -.75 D with the Crystalens.
Though Dr. Colvard thinks LASIK is a good procedure, he doesn't limit himself to that postop. "If we discover that the patient's refractive outcome with any of these presbyopic lenses is less than optimal, we have three options," he says. "We can remove the IOL and replace it with a lens of corrected power, we can use a 'piggyback' posterior chamber lens in the sulcus, or we can perform LASIK. I prefer LASIK when patients have residual astigmatic errors. When the refractive error is entirely spherical, either a lens exchange or a piggyback lens is a good option. The placement of a new lens of a corrected power or a piggyback is generally very successful in correcting refractive errors, since the refractive outcome of the first procedure can be precisely measured."
As for the timing of the enhancement procedures, Dr. Colvard says that, if you make the decision to do a lens replacement, it's usually best to do it sooner rather than later in order to avoid capsular fibrosis. "Lens exchange is much simpler and safer if performed before there's much capsular fibrosis," he notes.
He says a piggyback implantation can be performed virtually any time in the postop course. As a good rule of thumb with secondary implants, Dr. Colvard says that you obtain approximately 0.7 D of correction for every diopter implanted. Therefore, a +3 D secondary lens would give approximately +2.1 D of correction. He explains that, according to Texas surgeon Jack Holladay and others who have researched this, the reduction in power occurs because you're implanting the lens more anteriorly, which diminishes its effective power.
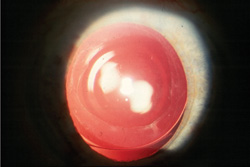 |
| The results of presbyopic IOLs such as the ReZoom can be honed by LASIK postop. Elizabeth Davis, MD |
Both he and Dr. Davis agree that if the presbyopic-lens patient is going to undergo LASIK, it's best to wait three months. "This is because I want the incision to be well-healed before I increase the intraocular pressure during the creation of the flap," Dr. Colvard says.
Though the LASIK procedure follows the normal course in these patients, there are a few differences or concerns when compared to LASIK on a phakic eye.
"With multifocal lenses, don't use wavefront-guided procedures," warns Dr. Davis, "because you don't want to negate the effect of the multifocal lens by negating all the desired aberrations it induces. Do a standard enhancement instead. With an accommodative lens, though, you can do a wavefront enhancement."
Since cataract patients are usually older, they may have ocular surface issues such as dry eye that need to be managed before they can undergo LASIK. If Dr. Colvard has an older patient with dry-eye symptoms and significant astigmatism, he'll place him on Restasis preop, and continue the treatment for several months before proceeding with LASIK. He'll use long-acting collagen punctal plugs for patients with very mild dry-eye symptoms.
Finally, if you use an excimer laser that requires dilation for its eye tracker to work, there's a chance that the tracker may be confused by the presence of the IOL and not work properly.
"We have both the Visx S4 and the LadarVision systems, and use them interchangeably for different corrections," explains Rom Kandavel, MD, Dr. Colvard's associate. "The LadarVision system is excellent, and the tracking system is wonderful when it does work, but one of the drawbacks is if a dilated, pseudophakic patient is brought under the system, it may not track, and you can't do the procedure. This is a difficult situation, because you can't then just use the Visx laser on the patient, because the Visx system requires the pupil to be undilated."
There are some tricks you can use to get the tracker to work in some cases, though.
"Sometimes, turning down the lights helps," explains Dr. Kandavel. "If that doesn't work, you can try lifting the patient up toward the tracker so he's actually out of focus for the laser. The tracker may lock on, and then you can put the patient back down in the preset position and the tracking will continue. Other times, you can hydrate the stromal bed, which can eliminate the rough appearance of the corneal bed and improve the quality of the image the tracker receives, enabling it to track the eye. But, if you do this, you have to make sure to dry the bed well before starting the procedure to avoid problems with over-hydration."



