Though LASIK is still the most-performed refractive procedure, the specter of ectasia and the occasional fussy flap have helped nudge the pendulum back toward surface ablation. Now, everything old is new again as surgeons discuss the best ways to debride the epithelium and minimize PRK's Achilles' heel: a painful, slow visual recovery. In this article, several experts with a particular interest in surface ablation share their tips for getting the best results with this rejuvenated procedure.
Who Gets PRK?
Surgeons say surface ablation is fitting nicely into a niche between LASIK and phakic intraocular lenses.
"Patients on the borderline between corneal procedures and phakic lenses, and who aren't good LASIK candidates, are in the sweet spot for PRK," says
San Francisco
Debriding the Epithelium
This step of the procedure lies at the heart of both PRK's disadvantages and advantages when compared to LASIK. Removing the epithelium instead of cutting a flap results in more postop pain and a slower visual recovery, but it also means the surgeon has more tissue to work with.
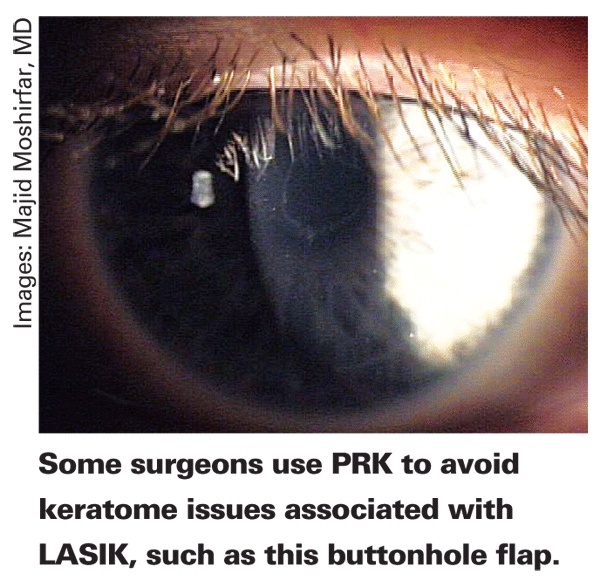
And since epithelial removal is such a key step to surface ablation, it's been the focus of attempts to modify the procedure, namely laser-assisted sub-epithelial keratomileusis and Epi-LASIK. In the former, the surgeon uses alcohol to loosen the epithelium, then moves it aside. He puts it back into place following the ablation. Epi-LASIK involves buying a new instrument, an epithelial separator, which operates similarly to a microkeratome, but instead of slicing through the stroma to create a flap, it creates a blunt dissection of epithelium from Bowman's membrane. In Epi-LASIK, as in LASEK, following dissection of the epithelium, the surgeon moves the sheet aside, does the ablation and replaces the sheet. Surgeons have also tried removing the epithelial sheet altogether.
Neither of these PRK variants has caught on with a large number of surgeons, and many people continue to discard the epithelial flap and essentially perform PRK with some slight modifications. However, to LASEK's credit, its legacy can be seen in the surface-ablation technique of those surgeons who prefer to use alcohol to loosen the epithelium.
"We primarily remove the epithelium with 18% alcohol, applied to cornea with a special trephine," says
With regard to epithelial removal, Dr. Moshirfar says it may represent an advantage of PRK over LASIK in some instances. "We've actually noticed that sometimes our iris registration capture ability is much higher with surface ablation than it is with IntraLase LASIK with the 60 KHz femtosecond laser," he says. "Sometimes the IntraLase flap creation process doesn't allow us to get a good iris registration, which can be due to the oblique bubble layer. When you have that, there are so many little reflections that the iris can't be registered properly. Sometimes with IntraLase LASIK our iris registration capture rate can go down from 100 percent to around 70 or 75 percent. With PRK, however, when you take off the epithelium and have a nice Bowman's, the image from the iris is so crisp that you can get a good iris registration."
For those wondering if there's a difference between techniques that leave the epithelium on afterward and those that completely remove it, Ottawa surgeon W. Bruce Jackson recently finished a large, retrospective study that may help. Though he can't share all the details since he's looking to publish the full study soon, Dr. Jackson says that, in 998 patients, he treated a number with Epi-LASIK with both flap on and flap off, and treated a similar number with LASEK, also removing the flap in some and leaving it on in others.
The preop refractions ranged from -1 D to -8 D. "The bottom line was we couldn't show a statistically significant difference in visual or refractive outcomes at six or 12 months," he says. "There may be some mild variations in the first week, though that's been controversial. Some people feel with the flap on, vision's a little better initially and there's a little less pain in the first day or two, but then they get more discomfort and the vision tends to drop a little bit. With the flap off afterward, they have a little bit more discomfort right up front, maybe the vision's not as good then, but they're more comfortable at day three or four and the epithelium tends to heal faster. All that's been said about leaving the epithelial flap on postop has really been questioned over time to the point that the majority has said there's probably no real difference."
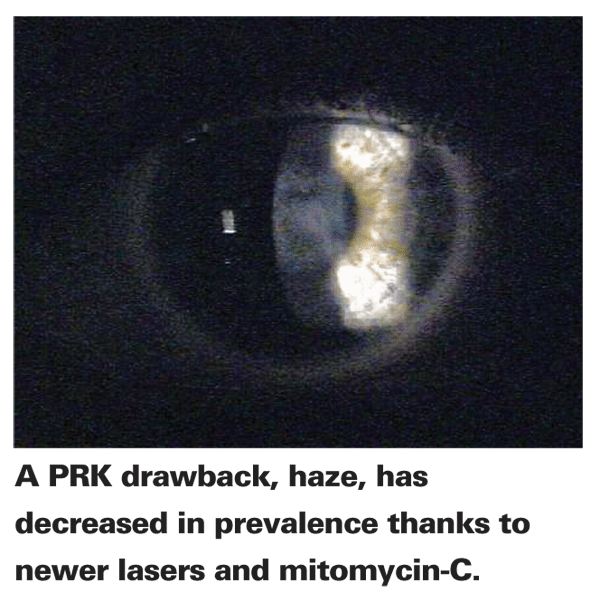
Recent studies of these surface ablation approaches have reached a similar conclusion. In one meta-analysis of seven articles encompassing 604 eyes with myopia up to -9 D, the researchers found that LASEK doesn't appear to have any advantage over PRK. The combined results showed comparable safety and efficacy between the two procedures from one to 12 months, and LASEK didn't relieve discomfort compared to PRK on day one postop or reduce corneal haze intensity at six and 12 months.1 A different study, double-masked and randomized, compared Epi-LASIK with the flap on in one eye and Epi-LASIK with flap removal in the fellow eye of 56 patients. The subjective pain score was lower in flap-off eyes at two hours postop, but then was comparable at later time points. There was no significant difference in spherical equivalent, line gain or loss, haze score or higher-order aberrations.2
How to Use Mitomycin
Another development that's boosted surface ablation's effectiveness and safety since the procedure's early days is the use of mitomycin. Surgeons say this helpful adjunct, in conjunction with better lasers and ablations, has reduced haze and regression.
The duration of Dr. Majmudar's mitomycin-C protocol has gradually decreased over the years, from two minutes to 12 seconds. "I'll use mitomycin-C for ablations deeper than 75 µm," he says. "Right now we use 0.02% on a sponge for 12 seconds on virgin corneas, followed by irrigation with copious amounts of BSS to make sure there's no residual drug on the surface of the eye. I think that, when used judiciously, mitomycin works very well." Other surgeons have a similar ablation depth criterion beyond which they'll use mitomycin, usually between 60 and 80 µm.
"At our center, we think anyone whose ablation is deeper than 60 µm should get mitomycin," says Dr. Moshirfar. "For depths shallower than 60 µm, we usually won't use it. This is because today's lasers, including the Visx and the Allegretto, have such smooth ablations that things are not at all like the olden days where second and third-generation lasers gave us haze." Dr. Moshirfar alters his protocol slightly as the ablation depth increases. "The duration has gone down to 20 seconds for most of our patients between 60 and 80 µm," he says. "For anyone between 80 and 100 µm we usually use 30 seconds of mitomycin-C. After the mitomycin application, we irrigate the area with two 5-cc bottles of chilled BSS."
Easing the Pain
The other aspect of surface ablation that's lent itself to experimentation is postop pain management. Here is the conventional approach, accompanied by a discussion of novel techniques.
"Once the contact lens is placed postop, we instill a drop of Acular LS," says Dr. Moshirfar. "It's important to note that the drop is instilled after the contact lens is in place. We speculate that you may increase the risk of melt if you place the drop directly on the stromal bed that was just ablated. We usually send the patients home with Acular LS, along with a fourth-generation fluoroquinolone and 1% prednisolone drops. We recommend they continue taking the Acular through the next day, for 48 hours total, including the day of surgery. For the steroid, our nomogram is based on the use of Pred Forte, though I think any prednisolone would be fine. We like to keep things the same with the nomogram to make sure we don't inadvertently change our re-epithelialization parameters. Our patients stay on the prednisone for a month, at which point we switch them to 0.1% fluorometholone drops t.i.d. for a month, dropping to b.i.d. for a third month and then, in some cases, continuing at q.d. for a fourth month.
"We use the topical antibiotic until the day of epithelialization and discarding of the contact lens," continues Dr. Moshirfar. "This is usually between the fourth and the eighth day."
Some surgeons like to add what have become known as comfort drops to the postop regimen. These are small, 1-ml bottles of artificial tears to which three or four drops of proparacaine have been added. They're intended for use when the pain is not well-controlled by the other agents. "I'm not using the so-called comfort drops," says Dr. Majmudar, "though I think they probably work well. You always worry about anesthetic being used indiscriminately, but most of the time the preparation is so dilute that they don't really have an anesthetic effect, but rather an analgesic one. So, they're cutting down the pain but not necessarily creating a situation where you can get corneal melting.
One big discussion point though, is who makes up the comfort drops? If you make them in your office and there's not a perfect sterile technique and an infection results, you could be liable. If I were to do it, I'd use a good compounding pharmacy."
Some other novel pain control approaches that surgeons are employing include:
• Oral Lyrica (pregabalin) and oral Neurontin (gabapentin). "Lyrica is an agent neurologists use for nerve pain elsewhere in the body," explains Dr. Majmudar, who uses the drug in his patients. "There's some anecdotal reports that Lyrica and Neurontin could potentially have some impact on PRK pain. I don't think it works by itself, but as a supplement in a short course, it seems to be effective. I use Lyrica 75 mg b.i.d. starting on the day of surgery and going for four days altogether. This is supplemented as needed with either Vicodin or Tylenol with codeine.
• Topical morphine. "Pain management is one of my areas of research," says Dr. Faktorovich. "I'm not a fan of topical anesthetics postop, even in dilute form, as there are reports of delayed epithelial healing and misuse by patients. I also don't use topical NSAIDs because of possible delayed healing issues. We've done studies, though, on topical morphine and found it relieves pain compared to placebo control, reducing pain as much as 50 percent with no effect on corneal re-epithelialization. This is because opiates target specific nerve receptors only, unlike other agents such as anesthetics and NSAIDs, which are non-specific and can bind to epithelial cells and interfere with healing."
• Topical Imitrex (sumitriptan). This migraine drug may have some application for post-PRK pain in a topical form. Dr. Faktorovich is currently studying this formulation. "We get it through Leiter's Pharmacy," she says. "They dilute it from a nasal spray. We did one study on 30 patients with 30 controls with a drug concentration of 1.2%, and found it doesn't impair corneal healing at all, with no statistically significant difference from placebo. Since that safety study was good, we intend to increase the concentration."
A tip surgeons offer for dealing with patients in pain is simple: Change the contact lens.
"Most of the time patient discomfort arises from a bad lens fit on the first day," says Dr. Moshirfar. "You can often relieve the pain by immediately changing the lens."
Even though PRK is enjoying another moment in the sun, surgeons still think it can get even better. "There's always room for improvement," says Dr. Majmudar. "We're OK at this point, but if we were to achieve a surface treatment that was pain-free, I think most surgeons would recommend a surface treatment over LASIK."
1. Cui M, Chen XM, Lü P. Comparison of laser epithelial keratomileusis and photorefractive keratectomy for the correction of myopia: A meta-analysis. Chin Med J (Engl) 2008;121:22:2331-5.
2. Kalyvianaki MI, Kymionis GD, Kounis GA, et al. Comparison of Epi-LASIK and off-flap Epi-LASIK for the treatment of low and moderate myopia. Ophthalmology 2008;115:12:2174-80.