Presentation
A 35-year-old man presented to his ophthalmologist complaining of blurred vision in his left eye for one day. Of note, he denied any pain, redness, flashes, floaters or other ocular symptoms.
Medical History
His past ocular history was unremarkable. He denied any past medical history, medication use, smoking, alcohol or illicit drug use. He also denied any recent history of trauma, illnesses, travel or new exposures. Review of systems was negative.
Examination
On examination, his visual acuity was 20/20 OD and 20/25-2 OS. His pupils were equal, round and reactive to light with a trace relative afferent pupillary defect OS. Color plates were 10/10 and brisk OD and 9/10 and slow OS. Extraocular motility and confrontational visual fields were full in both eyes. Intraocular pressures were 16 mmHg OU. Slit-lamp exam of both eyes was unremarkable with no evidence of anterior chamber or anterior vitreous cell.
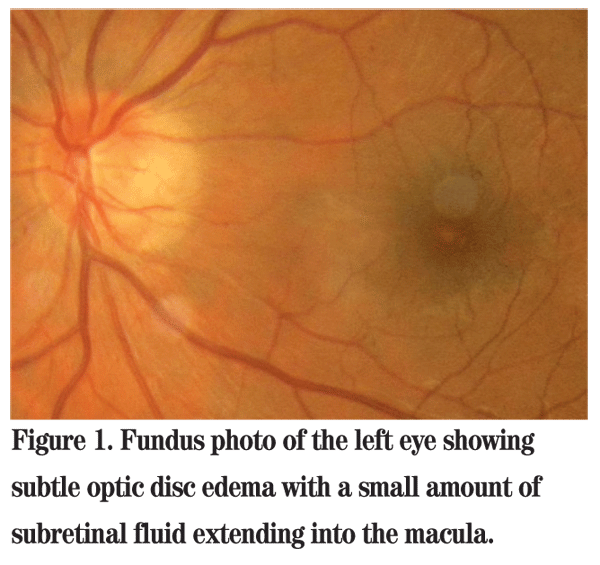
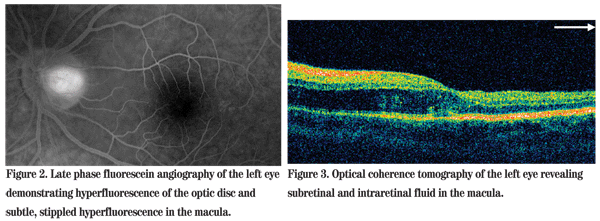
Dilated funduscopic exam of the left eye revealed subtle optic disc edema with a small amount of subretinal fluid extending into the macula (See Figure 1). The fundus of the right eye was unremarkable. Fluorescein angiography demonstrated hyperfluorescence of the temporal aspect of the optic disc (See Figure 2). Optical coherence tomography showed subretinal and intraretinal fluid in the macula extending under the fovea (See Figure 3). The patient was referred to the Wills Eye Institute Retina Service for further evaluation and management.
Diagnosis, Workup and Treatment
The differential diagnosis in this otherwise healthy patient with subtle optic disc edema and subretinal fluid includes both infectious and non-infectious entities. Non-infectious causes include optic neuritis, diabetic papillopathy, sarcoidosis, malignant hypertension, anterior ischemic optic neuropathy and retinal hemangioblastoma of the optic nerve.
Infectious etiologies include Bartonella henselae, syphilis, Lyme and herpes viruses.
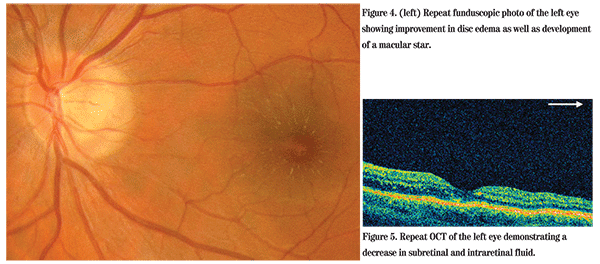
The patient's blood pressure was determined to be within normal limits. He denied any history of sexually transmitted disease, tick exposure, rash or herpetic infection. Given the patient's negative review of systems, he was initially observed without treatment. At follow-up five days later, his vision had improved to 20/25+1 in the left eye. Repeat funduscopic examination revealed improvement in the disc edema as well as development of a macular star (See Figure 4). A decrease in the subretinal and intraretinal fluid was also seen on OCT (See Figure 5). The clinical findings of optic disc edema coupled with subretinal fluid and a macular star were consistent with a diagnosis of neuroretinitis.
The differential diagnosis for neuroretinitis is extensive. Considerations include infectious etiologies, such as cocksackie virus, Epstein-Barr virus, hepatitis B, herpes simplex virus, influenza, mumps, parvovirus, Lyme, leptospirosis, syphilis, tuberculosis; as well as non-infectious causes, such as diabetic papillopathy, hypertension, inflammatory bowel disease, multiple sclerosis and sarcoidosis.
The patient was questioned further, which revealed that he had received a minor scratch from his pet kitten directly above his left eye. This incident occurred a few days prior to the onset of blurry vision. He did not initially offer this information because the scratch was so small and seemingly insignificant.
Given this clinical picture, the most likely cause of his neuroretinitis was B. henselae. A systemic workup revealed a positive B. henselae IgG titer of 1:2560 (neg <1:320). The patient was diagnosed with cat scratch disease and observation was continued. Of note, he never experienced prodromal symptoms, regional lymphadenopathy or conjunctivitis.
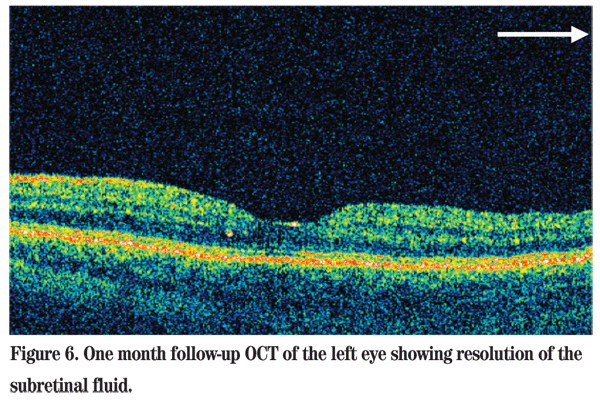
At one-month follow-up, his vision had recovered completely to 20/20 OS, with resolution of the subretinal fluid on OCT (See Figure 6).
Discussion
Cat scratch disease is caused by the gram-negative rod Bartonella henselae. Cats are the primary mammalian reservoir for the bacteria, which are spread through direct inoculation by scratches, bites or saliva into an open wound. Children and adolescents make up 80 percent of the reported cases in the
Though rare, patients who are immunocompromised may also present with encephalitis, osteomyelitis and hepatosplenic involvement.
The principal ocular manifestations of cat scratch disease consist of Parinaud oculoglandular syndrome and neuroretinitis. However, Bartonella henselae should be considered in the differential diagnosis of any of the multifocal white dot syndromes as well as cases of retinal choroiditis, branch retinal arteriole and venular obstructions, and serous retinal detachments. Parinaud oculoglandular syndrome occurs in approximately 5 percent of cat scratch cases and manifests as a granulomatous conjunctivitis with tender regional lymphadenopathy. Neuroretinitis, as in our patient, occurs in approximately 1 to 2 percent of cases and presents with disc edema and peripapillary subretinal fluid. The classic macular star typically does not appear until later in the disease course (about two to three weeks). The diagnosis is made through typical exam findings with a history of traumatic cat exposure and positive serologic testing for the anti-Bartonella IgG. Polymerase chain reaction testing is an emerging diagnostic tool, yet is not widely available. Traditional culture techniques for Bartonella are very difficult and not often used clinically.
Once the diagnosis is made, the disease is almost always self-limited and treatment is often unnecessary. In immunocompetent patients, antibiotics have no clear therapeutic benefit, despite the demonstrated in vitro susceptibility of B. henselae to multiple antibiotics. However, some cases with severe or persistent ocular or systemic complications and those in immunocompromised patients require systemic treatment with erythromycin or doxycycline.
The author would like to thank William Benson, MD, of the Retina Service at Wills Eye Institute for his assistance with this manuscript.
1. Cunninghang ET, Koehler JE. Ocular bartonellosis. Am J Ophthalmol 2000;130:340-9.
2. Ormerod LD, Skolnick KA, Menosky MM, et al. Retinal and choroidal manifestations of cat-scratch disease. Ophthalmology 1998;105:1024-31.
3. Reed JB, Scales DK, Wong MT, et al. Bartonella henselae neuroretinitis in cat scratch disease. Diagnosis, management, and sequelae. Ophthalmology 1998;105:459-66.