
Presentation
A 41-year-old African-American male presented to the Wills Eye Hospital Emergency Room complaining of a mild, dull pain behind his right eye for approximately two months. His symptoms began shortly after he started wearing his newly prescribed spectacles. During the previous two weeks, he felt the vision in his right eye was not as clear, describing it as "plastic over my eye." He denied any additional symptoms.
Medical History
The patient's medical history was significant for seasonal allergies and a herniated lumbar disc. His social history was significant for occasional alcohol use and a 15-year history of cigar smoking. Family history was significant for breast cancer. Review of systems was negative.
Examination
Ophthalmic examination revealed a best corrected visual acuity of 20/70 in the right eye and 20/20 in the left. Pupil exam revealed a right afferent pupillary defect. Visual fields were full to confrontation. Intraocular pressures were 19 mmHg in both eyes. During color-plate testing, only the test plate was seen by the right eye, with 10/10 appreciated by the left eye. The right eye demonstrated 15 percent red desaturation. Hertel exophthalmometry measured 22 mm on the right and 20 mm on the left. Amsler grid testing showed multiple scotomas on the right and was normal on the left. Exterior examination revealed possible mild proptosis on the right. Slit lamp examination was within normal limits. His dilated fundus exam was within normal limits except for a symmetric increase in the cup-to-disc ratio in both eyes.
Based on the history and examination, Humphrey visual field testing and orbital imaging was obtained. Visual field testing was within normal limits on the left and showed superior and inferior arcuate defects on the right. A non-contrast orbital CT was obtained (See Figures 1 and 2).
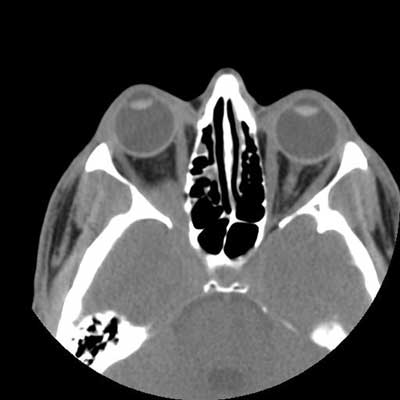
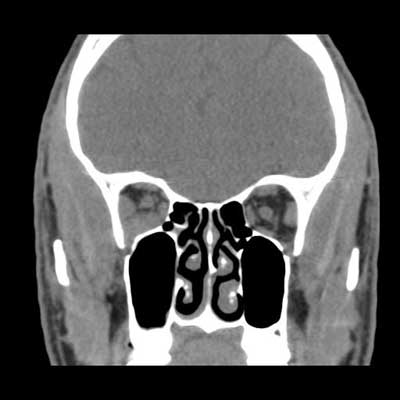
Figure 1.
Figure 2.
Diagnosis, Workup and Treatment
The CT scan shows an ill-defined right orbital apex lesion extending into the pterygopalatine fossa. To further evaluate the orbital mass, an MRI with gadolinium was obtained. This study revealed an enhancing lesion that extended not only into the pterygopalatine fossa but also into the cavernous sinus (See Figure 3).
The differential diagnosis of an orbital apex lesion with these characteristics includes lymphoma, sarcoidosis, idiopathic orbital inflammation, orbital metastases, Wegener's granulomatosis, tuberculosis and plasmacytoma. Prior to initiating further workup, more of the patient's history was elucidated as he admitted to a previous diagnosis of asymptomatic pulmonary sarcoidosis. After conferring with his pulmonologist, a presumed diagnosis of orbital sarcoidosis was made. The patient was started on 80 mg of prednisone by mouth daily. A two week follow-up visit revealed remarkable clinical improvement, including a visual acuity of 20/20 in the right eye, normal color vision, and no afferent pupillary defect. Repeat imaging revealed that the lesion was smaller.
Discussion
Sarcoidosis is a chronic multi-system granulomatous inflammatory disease. Jonathan Hutchinson first described sarcoidosis in a man with multiple cutaneous lesions in 1877. Caesar Boeck coined the term "sarkoid" in 1899. The first case of orbital sarcoid was reported in 1949 by F. N. Knapp and William Knoll. The incidence of sarcoidosis is approximately six per 100,000 people in the United States. The prevalence in African Americans is about three times higher than that of Caucasians. The typical age range for diagnosis is between 20 and 40 years of age. A slight female predominance exists.
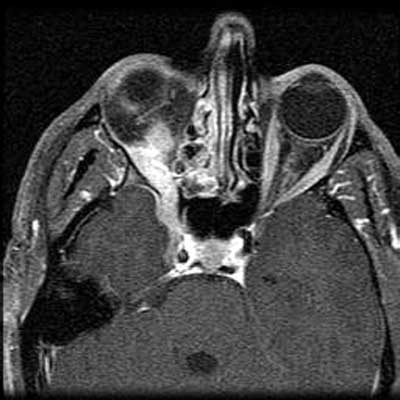
Figure 3. Axial T1 MRI with gadolinium.
There have been reports of spatial clustering of sarcoidosis leading to the theory of possible person-to-person transmission or common environmental exposure. In fact, transmission of sarcoidosis has occurred following organ transplantation. The disease's etiology remains unclear. Multiple infectious and environmental agents have been linked to the disease including the herpes virus, mycobacteria, talc and beryllium.
The clinical presentation of sarcoidosis is widely variable. Classic findings include bilateral hilar lymphadenopathy and noncaseating granulomas. The lungs are involved in 90 percent of patients. The next most frequently involved organ systems are the liver (50 percent), eye (25 to 60 percent), skin (25 percent) and CNS (10 percent).
An ophthalmologist makes the initial diagnosis of sarcoidosis in 10 to 20 percent of the cases. Multiple ophthalmic manifestations have been reported. In the lid and orbit, granulomas and lacrimal gland enlargement can be seen. Granulomas of the conjunctiva can be excellent sources for biopsy material when the diagnosis is in doubt. Uveitis is one of the more common manifestations of sarcoidosis. Retinal involvement can include vasculitis and focal retinitis. Choroidal granulomas are occasionally seen, and the optic nerve can be affected by compression or infiltration. Visual loss in sarcoidosis is most commonly due to cystoid macular edema, chronic secondary glaucoma and optic-nerve damage.
This case represents one of the more rare manifestations of sarcoidosis. The reported incidence of orbital sarcoid tumors is <0.5 percent. Orbital processes are thought to be more common in patients with systemic manifestations. Symptoms include decreased vision, diplopia and proptosis. Imaging can be quite helpful. MRI often reveals an infiltrating mass with homogenous enhancement and can help narrow the differential.
Diagnosis involves imaging, blood work and tissue confirmation. Eighty percent of patients with ocular sarcoid show thoracic abnormalities on chest X-ray or CT. In patients with orbital disease, MRI is the study of choice because of its soft tissue resolution. Gallium scanning has a high sensitivity but poor specificity. The classic "panda pattern" is highly suggestive for sarcoid showing increased uptake in the thorax, parotid, and lacrimal glands.
Angiotensin converting enzyme (ACE) levels may be elevated in 60 to 90 percent of patients and is thought to represent overall systemic disease activity. Biopsy shows noncaseating granulomas without evidence of specific infectious or environmental cause.
Corticosteroids are first-line therapy for ocular sarcoidosis. Depending on the severity, both topical and systemic steroids may be used. The incidence of severe systemic side effects makes steroid-sparing agents appealing. Methotrexate is often used for disease suppression and may be more effective in neurosarcoid than other agents. Additional immunosuppressives, such as azathioprine and cyclophosphamide, may be used in refractory cases.




