Try as they might, researchers and laser companies alike can't seem to get the cornea to act like a plastic lens. You can cut a couple of different zones into it to create some multifocality, but it insists on healing itself and altering the final result. However,
Multifocality—Lost in Translation
Dr. Seiler says the reason multifocal and diffractive multifocal lenses have been more successful than multifocal laser surgery is because the lenses can incorporate subtle zone changes, while corneal surgery often cannot.
"The nice thing about multifocal and diffractive lenses is that their effect is independent of pupil size, since it's accomplished with small zonal areas, one-tenth of a millimeter in size," Dr. Seiler explains, referring to the near and far zones of a lens giving the brain a near and far image to choose from. "So, you always have the same mixture of near and distant foci for the brain to select, in zones that can be organized concentrically or in multiple zones. We could create something like this on the cornea, but if you do it after LASIK, you'll have a smoothing effect from the repositioning of the flap that smoothes down these zones that levels out the small differences needed for this multifocality. That's why the array design that we need for a true multifocal cornea doesn't work. We're unable to get the small areas for near and distance, and are instead stuck with larger areas that are 1-mm to 1.5-mm wide." Having to put these larger areas on the cornea, rather than the many small, subtle ones that appear on a diffractive lens, forces surgeons to organize them in such a way that they work with the normal pupil reaction. "For instance, if the zones are too large," says Dr. Seiler, "then all of a sudden if the pupil is small and the cornea had a central zone for distance, you'd have only the distance part to look through. Or, if the pupil got very large, you'd have the near part. If you don't have 0.1-mm areas, but instead 1-mm or 1.5-mm areas, which arise after epithelial healing, you must consider the pupil's role when selecting those areas. That's how the two current approaches to presby-LASIK have come about: You either ablate the center for near and the periphery for distance or vice versa."
Dr. Seiler subscribes to an increasingly popular school of thought: Plan for an ablation that leaves the central cornea set for near viewing and the outer cornea for distance.
"When asking if there is anything that speaks for one of the two approaches to presbyopic LASIK, we found the so-called near reflex, a process that takes place in the brain, does," Dr. Seiler says. "For example, if you look at something near, such as writing on a page, the brain does three things: First, it tries to accommodate with the crystalline lens to make the image sharp, a process that decreases with age until it's only around 1-D strong at around 45 years of age. Second, it converges the eyes, in which both eyes look at the same point and move inward to target it. And third is pupil miosis. Whenever you look at something nearby, the pupil automatically constricts. It might go from 5 mm to around 2.5 mm, for example. Therefore, it makes more sense to make a near zone centrally on the multifocal cornea."
A Smoother Transition?
In an effort to create an increased depth of field that enhances near vision in a way closer to a multifocal lens, Dr. Seiler has developed a new approach to multifocal corneas in a procedure he calls "advanced monovision."
Instead of dividing the cornea into zones as in other presbyopic LASIK approaches, Dr. Seiler uses a scanning spot laser to create a hyperprolate cornea on one eye, usually the non-dominant one. Instead of treating the non-dominant eye for -1.5 or -2 D as in normal monovision, he programs the laser to increase the Q-factor of the cornea, a measurement of its asphericity, to an unphysiologic level, usually -1 (normal procedures usually shoot for a postop Q-factor of -0.4). He says that any laser that allows you to aim for a certain asphericity value can do it, such as the WaveLight, the Schwind and the Carl Zeiss Meditec lasers. He also feels the Visx could do it, as well, with some minor reprogramming by the company's engineers.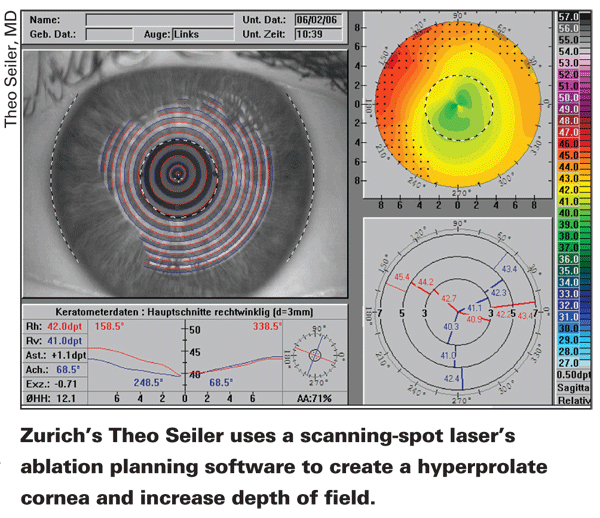
The effect of this hyperprolateness is a smooth transition from the central cornea out to the periphery in the presbyopic eye, with a power that steadily decreases outward, rather than the truncated zones used by other multifocal ablation approaches. "At the center, the eye is at -2 D or -1.5," Dr. Seiler says. "Then, 4 mm out, it's at -1 D; at 5 mm it's at -0.5 D. It's not like normal monovision where if the patient looks in the distance he's still at -2 D with the non-dominant eye. Instead, with this, due to the pupil size when looking at distance, he's only -0.5 D or -0.75 D, which can easily be tolerated; we've found that anisometropia of 1 D or less can be tolerated by nearly everyone. Only a few people, with other disorders such as latent strabismus, will suffer from the increased anisometropia." He tests the effect with contact lenses before treatment. "Once a patient shows he can tolerate it, and even likes it, he may just stay with the contact lens and forego the surgery," says Dr. Seiler. "That's one of the hazards of this!"
One of the drawbacks of the procedure is that increasing the corneal Q-factor from the usual target of -0.4 to -1 takes more tissue, approximately 30 extra microns, because the laser is, in effect, "doing a PTK procedure in the center and a hyperopic correction in the periphery," explains Dr. Seiler. The optical zone is 7 mm, but the ablation zone is 9 mm because there's blending at the edge.
He notes that this procedure isn't for every patient. "I wouldn't recommend it for 3 D or more of myopia because these patients are so used to seeing well at near that it's hard to convince them that -1.5 D is good," says Dr. Seiler. "Hyperopes are the greatest patients, and are very grateful for the treatment." However, there are a couple of limits with the hyperope: The central K reading shouldn't be higher than 48 D; otherwise the shape isn't stable in terms of the healing response, says Dr. Seiler. The surgeon shouldn't attempt more than +4 D of correction, because Dr. Seiler says the healing reaction of the cornea makes the optical zone shrink over the years, which can be a real problem if it shrinks and the initial ablation was a little decentered to begin with. Dr. Seiler also does scotopic, photopic and near-reflex pupil testing beforehand to ensure that the pupil size is large enough in bright conditions to allow the non-dominant eye to see well at distance, and that it comes down enough to get a good near effect.
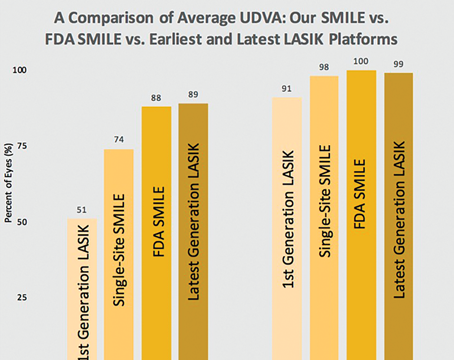
In his practice Dr. Seiler says the monocular near and distance acuities in the operated eye average about J3 and 20/30. He says this is better than monovision's usual results, which most often result in J1 or J2 at near but only 0.3 or 0.2 (around 20/40 or 20/32) at distance. He says the procedure also puts less of a hit on the patient's low-contrast acuity. "Whenever you do multifocal procedures, the low-contrast acuity usually drops," he says. "But it isn't the case with this procedure. With this ablation, it's pretty much unchanged."