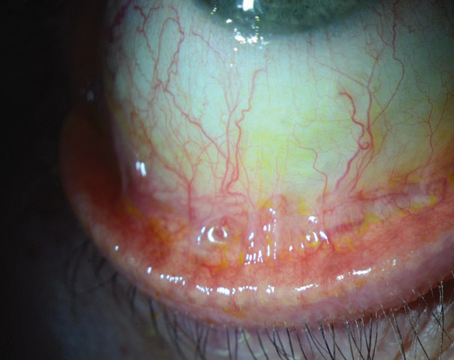
The use of anti-vascular endothelial growth factor drugs and endothelial keratoplasty techniques have been popular areas of corneal research for several years. With time and data, refinements and improvements highlight this year's cornea ARVO submissions. (Unless otherwise specified, these reports had no commercial support.)
Bevacizumab
Subconjunctival bevacizumab could potentially offer an alternative or adjunctive measure to conventional therapies in preventing graft rejection in vascularized high-risk corneal transplantation, according to researchers in
Prior to corneal transplant, the researchers placed intrastromal sutures for two weeks in the corneas of mice, causing intense angiogenesis. Following corneal transplant, topical bevacizumab (2.5%) was applied t.i.d. for three weeks in one treatment group, while 0.02 ml (0.5 mg) of bevacizumab was injected subconjunctivally the day of surgery and four, eight and 15 days post-transplant in the other treatment group. Control groups received either topical or subconjunctival phosphate buffered saline. Grafts were examined twice a week for eight weeks by slit-lamp, photographed once a week and scored for opacity as well as neovascularization.
All corneal transplants in the control groups were rejected by three weeks. All corneal grafts in the topical treatment group were also rejected, although not until four weeks post-transplantation. Interestingly, in the subconjunctival treatment group, 33 percent of corneal grafts survived out to eight weeks post-transplantation (p= 0.008).4966
Another group in
At final examination, the dexamethasone group showed a significant lowering in corneal opacity score as compared to both control (p=0.025) and bevacizumab 2.5 mg groups (p=0.007). On the new vessels size score, dexamethasone group showed a significant reduction as compared to all other groups (p=0.013). Surface of corneal neovascularization was significantly smaller in dexamethasone (p=0.043) and bevacizumab 5 mg (p=0.049) groups compared to control (p=0.016) and bevacizumab 2.5 mg (p=0.014). The study demonstrates the ability of a 5 mg/day bevacizumab subconjunctival injection to cause a short-term involution of corneal neovascularization after corneal alkali burn but with limited effects compared to steroids. Further studies using combinations of these treatments are needed.4969
Endothelial Keratoplasty
Surgeons in
A surgeon at UCLA attempted to quantitate the expected refractive shift following DSEK surgery to facilitate selection of the appropriate IOL power in patients undergoing combined DSEK/cataract surgery. The retrospective review looked at 16 combined surgeries to determine the difference between the stable postop refraction and the expected postop refractive error based on the preop IOL power calculation. In each case, either a one- or three-piece IOL was placed in the capsular bag. Reliable postop refraction was obtained in 13 of the 16 cases; two patients had less than one month follow-up and one patient had significantly limited visual acuity secondary to a submacular choroidal melanoma.
A hyperopic refractive shift was observed in 12 of the 13 eyes, with a mean hyperopic shift of +1.30 D (r: +0.2 D to +2.96 D (SD=0.88 D). One patient experienced a myopic refractive shift of -1.98 D, although as the BCVA was 20/70, the validity of the measured refractive error was questioned. Given the hyperopic shift of approximately +1.3 D, as well as the relatively large standard deviation of postop refractive errors, the researcher advises surgeons to select an IOL power that is predicted to result in a postop refractive error of -1.5 to -2 D when performing combined DSEK and cataract extraction.638
Still another group studied combined DSEK/cataract surgery, this one to compare outcomes of a simultaneous combined procedure versus consecutive staged procedures. 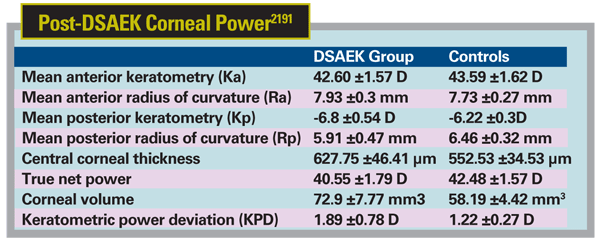
The retrospective analysis took place at the Univesity of Mississippi Medical Center, Jackson, and included 15 consecutive patients who underwent DSEK for corneal edema and guttatae from Fuchs' endothelial dystrophy and standard cataract surgery as a combined procedure (eight eyes) or staged procedure (seven eyes). The combined-procedure eyes had a median postop BCVA of 20/50 at one month, 20/40 at two months and 20/30 at four months compared to staged-procedure eyes, 20/100, 20/50 and 20/40 at the same times frame (p=0.29, p=0.007, p=0.082). The rate of endothelial graft detachment was three eyes (37 percent) in the combined procedure and 28 percent in the staged procedure. The postop SE refractive error was within 1 D of emmetropia in 83 percent and within 2 D of emmetropia in 100 percent of eyes.
The result was a statistically significant better visual acuity at one and two months postop when DSEK and cataract surgery were performed simultaneously. The four-month postop BCVA showed a marginally significant difference between the groups but they appeared to approach one another. Results suggest a more rapid VA rehabilitation when DSEK/cataract surgery are done simultaneously but eventual long-term VA may be the same between the two methods. It appears either method provides a predictable refractive outcome. There was a slightly higher rate of graft dislocation with the combined procedure that may be due to residual viscoelastic at the graft-donor interface.2217
The true net power of the cornea shows statistically significant lower values as compared to age-matched controls after DSAEK surgery, according to a study at the
The study involved 32 eyes of 28 patients who underwent DSAEK and were evaluated with a Pentacam Scheimpflug camera at three months postop. Researchers obtained: mean anterior keratometry (Ka); anterior astigmatism; mean anterior radius of curvature (Ra); mean posterior keratometry (Kp); posterior astigmatism; mean posterior radius of curvature (Rp); central corneal thickness; true net power; corneal volume; keratometric power deviation (KPD); and mean zonal equivalent K readings (EKR) at 2 mm, 4 mm and 6 mm. These values were compared with 32 non-surgical eyes of 32 age-matched controls.
The Ka, Rp and true net power were lower in DSAEK group as compared to controls. On the other hand, Ra, central pachymetry, cornea volume and KPD were higher in the DSAEK group as compared to the controls. The mean Kp had higher negative value in DSAEK eyes as compared to controls, suggesting increased posterior curvature due to the endothelial graft. EKR values increased towards the periphery in both groups and were lower in DSAEK group as compared to controls in all the zones. The difference was found to be statistically significant (p<0.01) for all the parameters except Ra and anterior surface astigmatism between the two groups.2191
A New York Eye and Ear Infirmary study documents a statistically significant improvement in visual acuity in patients who underwent DSAEK. The retrospective review of 125 consecutive eyes that underwent DSAEK included patient demographics, indication for surgery, prior surgeries, presence or absence of co-morbid diseases, pre- and postop refraction, and pre- and postop VA in both Snellen and logMAR forms.
Patients' mean age was 71.05 (r: 32 to 93). Most cases were performed for Fuchs' endothelial dystrophy (51) or pseudophakic bullous keratopathy (49); other indications included: aphakic bullous keratopathy, failed PK or DSAEK, unspecified corneal edema, corneal edema secondary to a glaucoma implant and Descemet's rupture. Preop vision (logMAR) was 1.152 ±0.580. The average month of BCVA was 5.735 with a mean BCVA of 0.562 ±0.449. In a statistical analysis with a paired sample t test, the mean difference was 0.5917 (95 percent CI=0.4840 to 0.6995) with a p-value <0.0001, indicating a statistically significant postop visual improvement.
At postop month two, patients had gained an average of 2.056 ±3.749 Snellen lines or 0.322 ±0.689 logMAR lines. At the month of BCVA, Snellen lines gained were 4.040 ±3.694 and logMAR lines gained were 0.581 ±0.644. Further analysis is currently under way to determine factors correlated with improvement in postoperative visual acuity.2211
A group at Doheny Eye Institute,
Most cases were due to Fuchs' dystrophy, bullous keratopathy or a failed PK. They were examined under a light microscope with H&E and PAS staining. Corneal transplantation failure was defined as corneal edema that did not resolve with maximum medical therapy or as a dislocation that could not be repositioned successfully.
The Descemet's membranes fell into one of two categories: clean and unclean (i.e., the presence of residual stroma or a retrocorneal membrane). Seventy-six samples were histologically clean, and 29 samples had either residual stroma (13) or a retrocorneal membrane (16). A total of 23 (21.9 percent) graft failures occurred from the 105 DSAEK surgeries performed. Seventeen out of the 23 patients (73.9 percent) who had DSAEK failures had a histologically unclean stripping of the Descemet's membrane. Thirteen patients of the 23 failed grafts (56.5 percent) had a retrocorneal membrane and four of the 23 (17.4 percent) had residual corneal stroma. The remaining six patients who had DSAEK failure had a clean Descemet's membrane. Three (50 percent) of these patients had a pre-existing anterior chamber intraocular lens and two (33.3 percent) of these patients had intraoperative complications requiring lenticule sutures for reinforcement.
Also, out of the 23 patients with DSAEK failures, seven of these patients underwent a regraft procedure. Out of these seven, six patients (85.7 percent) had a retrocorneal membrane on the original Descemet's membrane specimen submitted and also had a retrocorneal membrane on the second specimen submitted for histologic analysis. The remaining patient had residual stroma seen on both the original and second specimens.
This study shows increased risk of DSAEK failure when the patient has a histologically unclean stripping of Descemet's membrane. Other factors that may increase the likelihood of failure include the presence of a retrocorneal membrane, an ACIOL, or the need for use of sutures for lenticule positioning.636
An
An interventional, retrospective study of DSAEK cases performed in 2007 by a single surgeon included three methods of donor graft insertion: folding the donor graft in a 60/40 taco configuration with the endothelial side inward and inserting it with single-point fixation forceps that had relatively sharp tips; folding the graft in a similar manner and inserting it with rounded-tip, single-point fixation forceps with a stop that kept the tips 150-µm apart to help minimize tissue compression; and pulling the graft through a funnel glide that curled the graft into a cylindrical shape for insertion. A 5-mm incision width was used in all cases. Endothelial cell density was assessed one year after DSAEK using specular and confocal microscopy. The one-year postoperative cell density was compared with the donor cell density reported by the provider eye bank to determine one-year cell loss. Analysis of variance was used to compare the cell loss with the three insertion methods.
One-year endothelial cell density was assessed in 150 eyes. The three insertion groups had comparable patient demographics, including age (p=0.67), sex (p=.18) and reason for transplant (p=.19). The mean one-year endothelial cell loss was 27 ±19 percent when the graft was pulled into the eye through a funnel glide, 31 ±19 percent with the rounded-tip, single-point fixation forceps, and 37 ±21 percent with the sharper-tipped, single-point fixation forceps. The one-year endothelial cell loss in the three groups differed by a statistically significant amount (p=0.04).613
Surgeons at the Medical College of Wisconsin,
The combined procedure yields stable visual results, predictable spherical equivalent refractive outcomes, and has no observed effect on keratometric astigmatism through two years of follow up.606
Noting that DASEK patients receiving general anesthesia have more difficulty maintaining postoperative positioning due to nausea and disorientation, researchers at the Cleveland Clinic compared the incidence graft dislocation in patients receiving general versus local anesthesia. They reviewed charts of 101 patients (127 eyes) who had primary DSAEK performed by four surgeons at the Cole Eye Institute; 93 were performed with local anesthesia and 34 with general anesthesia. For the local anesthesia group, complications were reported in six patients (6.4 percent), including: graft dislocation in three patients (3.2 percent), formation of peripheral anterior synechiae requiring lysis of adhesions in two patients (2.1 percent), and vitreous in the AC requiring anterior vitrectomy in one patient (1.0 percent). For the general anesthesia group, complications were reported in nine patients (26.5 percent), including: graft dislocation in seven patients (20.6 percent), formation of peripheral anterior synechiae resulting in angle-closure glaucoma and requiring lysis of adhesions in two patients (5.9 percent), and inadvertent injection of air posteriorly requiring vitrectomy in one patient (3.0 percent).
The relative risk of all complications for the general anesthesia group was calculated to be 4.1; the relative risk of requiring re-bubbling in the general anesthesia group was 6.38.
Although other factors including surgical technique and experience may confound this data, the group recommends that ophthalmologists should be aware that general anesthesia may increase the risk of complications in patients undergoing DSAEK.2198
A group of researchers at
Their conclusions: Eyes with better BSCVA after DSEK tend to have thinner overall pachymetry as well as thinner donor grafts. Surgical modifications to reduce donor graft thickness may improve visual outcomes in the future. Eyes with worse BSCVA after DSEK tend to have higher surface and interface reflectivity which may be representative of interface haze and subepithelial haze from prior chronic corneal edema. They call for additional studies to assess the potential relative impact of corneal haze and donor graft thickness on VA outcomes after DSEK.619
Collagen Cross-linking
Collagen cross-linking using ultraviolet A and riboflavin to increase the biomechanical strength of the cornea to treat diseases such as keratoconus continues to draw interest from corneal researchers.
A group at the
They measured input pressure and the corresponding corneal apex displacement six times per minute over 10 minutes. A plot was obtained comparing the input pressure with the corresponding corneal apical displacement. Eight of the 10 corneas demonstrated less displacement over the pressure range after treatment when compared to before treatment. Additionally, the variation of displacement corresponding to a given pressure decreased after treatment. The fact that the corneas demonstrated decreased displacement after treatment and they were more likely to have a stable displacement for a given IOP indicates that they were more stiff after treatment with riboflavin and UVA than before, the group concludes, saying the results seem to correlate with the mounting evidence contributing to the promise of the use of riboflavin and UVA as a treatment for keratoconus.5480
Researchers in
Mean initial corneal thickness was 451.3 µm (r: 330 to 575). Mean epithelial thickness was 52.7 µm (r: 13 to 102). No differences in epithelial thicknesses were seen between KC and ectasia eyes. Following debridement, mean thickness was 383.2 µm (r: 269 to 505). After riboflavin 0.1% plus dextran for 30 minutes, mean thickness was 355.8 µm (ranging 228 to 510). The cornea thinned in 37 eyes (74 percent), swelled in 12 eyes (24 percent) and was unchanged in one eye (2 percent) during initial 30 minute administration of the riboflavin.
Thirty-nine of the 50 eyes (78 percent) required the use of hypotonic riboflavin to achieve the minimum corneal thickness of 400 µm for UV irradiance. For all eyes, mean thickness was 421 µm (r: 401 to 510) before UV irradiance and after hypotonic riboflavin 0.1% use, if it was necessary). Mean corneal thinning with 30 minute UV exposure was 129.5 µm (SD 41); cornea thinning was comparable in KC (133.2 µm, SD 41.8) and ectasia eyes (123.1 µm, SD 40.2). There was no difference between the hypotonic riboflavin (132 µm, SD 36.8) and no hypotonic needed groups (120.7 µm, SD 55.2). At the conclusion of UVX treatment, mean thickness was 291.4 µm (r: 209 to 391).
The optimal method of using hypotonic riboflavin or other methods to increase and maintain corneal thickness throughout cross-linking remains to be elucidated, they conclude.5490
Adjunctive treatment with UVA-induced cross-linking appears to be a safe and effective treatment to prevent ectasia in high-risk myopic patients undergoing photorefractive keratectomy.
Surgeons at NYU School of Medicine, New York City, performed PRK on 45 high-risk myopic patients with a WaveLight excimer laser. Following PRK, the eyes underwent UVA-induced CCL (370 nm, 7 mW/cm2 for 10 minutes) after the administration of 0.1% riboflavin drops. The mean follow-up was 1.6 years (r: one to four years). Mean UCVA improved from 20/100 (Snellen) to 20/15; BSCVA from 20/20 to 20/15; and the spherical equivalent from -6.25 D to +0.2 D. Mean K changed from 45.5 D to 39 D, pachymetry from 495 to 385 µm and endothelial cell count from 2,750 to 2,800. No cases developed signs of ectasia.5470
A combined team from
In their study, 13 eyes from five female and eight male patients (mean age: 42 ±8.2 years) with topographically documented progressive post-LASIK ectasia were treated with cross-linking. The standard treatment procedure was used, applying riboflavin 0.1% following epithelial abrasion. The cornea was then irradiated with UVA light. The eyes were monitored for a minimum of 12 months. At 12 months after cross-linking, mean BSCVA had significantly improved from 0.73 ±0.57 to 0.83 ±31 (decimal scale).
Topography maps showed examples of markedly reduced steepest points as early as four months following treatment, as well as stability of keratometry readings over six months and more. Mean central corneal thickness decreased significantly (p<0.05) from 425 ±26 µm before treatment to 402 ±24 µm at one year. Corneal volume also decreased significantly (p<0.05) from a preop 57.97 ±4.82 mm3 to 54.16 ±3.02 mm3 at 12 months postop.5475
Miscellaneous
Surgeons at the
Using a femtosecond laser, they create an eccentric posterior lamella of approximately 200 µm. Through a clear cornea incision this is rotated to bring peripheral endothelium to the visual axis and diseased endothelium to the periphery. They successfully performed what they call posterior endothelial rotational lamellar keratoplasty (PERL-K) in six cadaver eyes. Initial results indicate surgical feasibility and early promise in optical rehabilitation.611
The biomechanical properties of the cornea are altered in diabetes mellitus, say researchers at the University of Dresden, Germany. Corneal hysteresis and corneal resistance factor are significantly higher in poorly controlled diabetes and show a significant correlation to the current glycosylated hemoglobin values.
In the prospective clinical trial, one randomly chosen eye of 35 healthy subjects and 31 diabetic patients was examined. Diabetic patients comprised group 1 (n=14) with HbA1c <7 percent and group 2 (n=17) with HbA1c ≥7 percent. Hysteresis and resistance factor were measured by the Ocular Response Analyzer, and central corneal thickness by ultrasound pachymetry. IOP was evaluated using the Goldmann tonometer, the Pascal Dynamic Contour Tonometer as well as the ORA, and the HbA1c was measured. As hysteresis and resistance factor are dependent on IOP and CCT, the group devised a correction formula.
The mean HbA1c value of healthy subjects (n=35) was 5.44 ±0.46 percent, 6 ±0.78 percent in diabetes patients group 1, and 8.58 ±2.44 percent in diabetes patients group 2.
Healthy subjects were statistically significant lower compared to diabetic group 2 in hysteresis (p=0.031) and resistance factor (p=0.029). Additionally IOPs by Pascal DCT (p=0.012) and Goldmann (p=0.032), as well as HbA1c level (p=0.0001) were statistically significant different, but not age, sex and CCT. There was no statistically significant difference between the healthy subjects and the diabetes patients of group 1 in hysteresis (p=0.071) and resistance factor (p=0.067). Overall diabetic patients (n=31), hysteresis (p=0.012) and resistance factor (p=0.008) were dependent on HbA1c. In the healthy subjects hysteresis (p=0.931) and resistance factor (p=0.837) were not dependent on HbA1c.1761
A group at
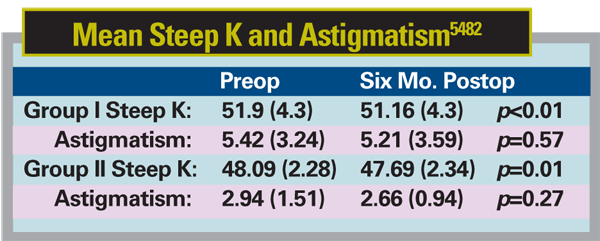
In the Ortho-K group, after one week of wearing the RVG lens but before cross-linking treatment there was minimal change in mean steep K: baseline: 48.09 D (2.28 SD), post-ortho-K 47.86 D (2.74), p=0.25; and astigmatism: baseline: 2.94 D (1.51), post-ortho-K 3.12 D (1.29), p=0.64) (See table below).
At six months post-cross-linking, steep K reduced significantly in both groups from baseline. Astigmatism also reduced but insignificantly from baseline.
There was no difference in effect in the two groups (steep K p=0.3, astigmatism p=0.79) even after correcting for baseline differences in steep K and astigmatism. The trial suggests that one week preop Ortho-K does not seem to work better than standard cross-linking in improving the corneal shape and reducing astigmatism in patients with keratoconus.5482
Physicians are under-treating pain in the case of acute corneal injury, a condition that is known to be extremely painful, according to a small study at
Dr. Afshari is an associate professor of ophthalmology at the