In science and medicine, research-ers are always looking for ways to visualize ever tinier pieces of the world. Now ophthalmic researchers are developing new technology to enhance our ability to see individual cells in the retina in 3-D, in vivo, more clearly than ever before.
John S. Werner, PhD, a professor at the
Enhancing Lateral Resolution
Dr. Werner explains that the idea of combining adaptive optics and OCT resulted from the need to make OCT's lateral resolution as detailed as its axial/depth resolution. "OCT has great depth resolution, depending on the light source you use," he explains. "The broader the bandwidth of the light—that is, the greater the range of wavelengths it contains—the better the depth resolution. However, lateral resolution is a separate issue; it's determined by the optical system you use and the aberrations of the eye, which can vary over time and space. For example, every time you blink, your tear film is spread across your cornea—but not necessarily evenly. When your blood rushes through the retina with your pulse, the retina moves ever so slightly, changing the focus for capturing an image. Eye movement and accommodation also change the aberrations.
"The purpose of adaptive optics," he continues, "is to detect these aberrations using a wavefront sensor and correct them in real time using a wavefront corrector—usually a deformable mirror. Basically, we create a closed loop between the system used for imaging and the optics of the eye. This allows us to create lateral resolution that rivals OCT's axial resolution.
"Unfortunately, the broader wavelength spectrum that enhances axial resolution can undermine lateral resolution by creating chromatic aberrations," he says. "However, we've designed a special lens to correct for that, allowing us to refine the lateral resolution in spite of this obstacle. The bottom line is that we have to fight for every micron of improvement because solving one problem often creates a new one."
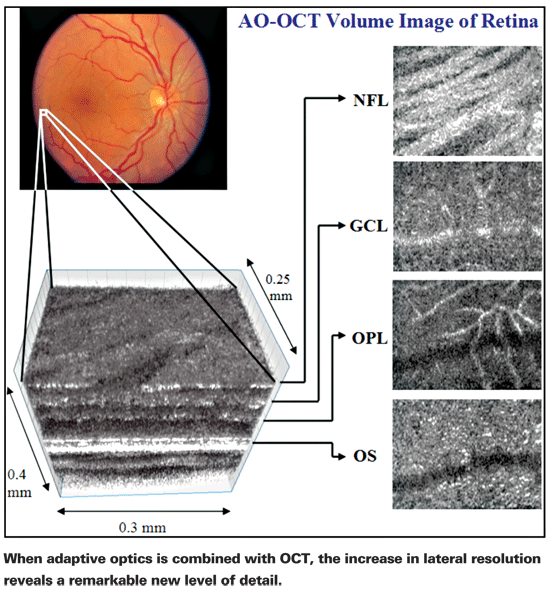
Dr. Werner says that none of the OCT instruments that are widely available incorporate this technology—yet. "It's technically challenging to package something like this for a commercial device," he observes. "People get a little gun-shy when they see our equipment because it's laid out on a rather large optical bench, about four feet by five feet. However, the technology can be scaled down; we just don't bother because for us it's a moving target. One of the challenges, for example, is the quality of the deformable mirror. The scale of our instrument allows us to easily evaluate new components. Once the technology is finalized it can be made small and manageable for a doctor's office; we've created one prototype that's similar in size to a standard OCT instrument."
Making the Invisible Visible
Dr. Werner explains that their current challenge is increasing contrast in the images.
"Contrast is separate from resolution," he notes. "Resolution refers to the smallest detail you can see, while contrast involves the ratio of light to dark. We currently have enough resolution to see ganglion cells, for example, but visualizing them is difficult because they lie in front of the photoreceptors and are almost invisible. As a result, we have to use other image-processing techniques to enhance their contrast. We're incorporating some of the techniques astronomers use to enhance the visibility of distant planets, as well as algorithms that locate edges. In fact, one of the advantages we've had here at UC Davis is that some of our colleagues in computer science have been working on these digital processing techniques for the last 30 years."
Other approaches are also under investigation. "One of our partners—Don Miller at
Dr. Werner notes that being able to visualize individual cells in high-resolution 3-D could have multiple advantages. "Disease begins at the cellular level, and presumably therapy begins there, too," he says. "So as a research tool, this has tremendous implications. It may also be advantageous for doctors in the field, allowing them to evaluate progress in treating patients. It could also benefit surgeons as part of an operating microscope.
Physicians in our clinic have been able to see things using our devices that have changed what they decided to do in surgery. And right now, other researchers are using this technology in endoscopes—scaled down in size, of course. That can help them work in other parts of the body, evaluating a cancerous tumor, for example.
"Beyond that," he adds, "our technology has plenty of other potential uses. For example, we can now visualize blood flow in the very tiny capillaries in the retina using this technology combined with Doppler—work that's being pioneered by our colleague Joseph Izatt at Duke University. Sometimes monitoring functional changes can be more diagnostic than just looking at structures."
Coming Soon?
"This is new technology, so it will take a while to see where it's useful and where it's not," says Dr. Werner. In terms of when it might be available in a commercial instrument, he says it's difficult to be sure. "I wouldn't be surprised if a manufacturer developed this in the near future," he says, "but it still could take a long time to reach the end user." Whatever the timeline, it seems clear that this technology has the potential to take ophthalmic research, diagnosis and treatment to an even higher level.



