A 45-year-old Caucasian male presented to the Wills Eye Neuro-Ophthalmology clinic after he noticed a change in his eye appearance approximately one month prior. He had noticed his right eye had a more “wide-open” appearance. He also reported some difficulty looking up, but denied diplopia. He reported minor head trauma seven months ago and described bumping his head on a steel beam. He denied any loss of consciousness.
 |
||
 |
 |
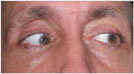 |
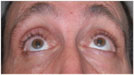
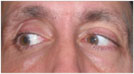
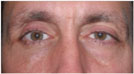
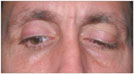
| Figure 1. External photographs of the patient's extraocular movements. |
 |
The patient had no history of any ocular conditions or sinus disease. Review of systems was negative. He was not on any medications and denied any allergies. He denied tobacco or alcohol use. His family history was significant for diabetes mellitus and hypertension.
Examination
Visual acuity with his spectacles was 20/50 in the right eye, improving to 20/20 with pinhole, and 20/25 in the left eye. Pupils were equal and without evidence of an afferent pupillary defect. Eyelid position showed a MRD1 of 5 on the right and 3 on the left. A deep superior sulcus and high lid crease were noted on the right. Orbicularis oculi strength was normal. Hertel exophthalmometry was 18 on the right and 21 on the left with a base of 105. No hypoglobus was noted. There was no palpable step-off of the orbital rim or periorbital hypoesthesia. Extraocular motility showed an upgaze limitation in the right eye (See Figure 1). Alignment measurements did not illustrate a pattern consistent with any cranial nerve palsy. Intraocular pressure was 14 mmHg in the right and 13 mmHg in the left. Confrontational field testing was normal. Color vision was 10/10 in both eyes. Slit-lamp and dilated fundoscopic examinations were unremarkable.
Visual acuity with his spectacles was 20/50 in the right eye, improving to 20/20 with pinhole, and 20/25 in the left eye. Pupils were equal and without evidence of an afferent pupillary defect. Eyelid position showed a MRD1 of 5 on the right and 3 on the left. A deep superior sulcus and high lid crease were noted on the right. Orbicularis oculi strength was normal. Hertel exophthalmometry was 18 on the right and 21 on the left with a base of 105. No hypoglobus was noted. There was no palpable step-off of the orbital rim or periorbital hypoesthesia. Extraocular motility showed an upgaze limitation in the right eye (See Figure 1). Alignment measurements did not illustrate a pattern consistent with any cranial nerve palsy. Intraocular pressure was 14 mmHg in the right and 13 mmHg in the left. Confrontational field testing was normal. Color vision was 10/10 in both eyes. Slit-lamp and dilated fundoscopic examinations were unremarkable.
What is your differential diagnosis? What further workup would you pursue?



