For an ocular surgeon, performing a flawless surgery is always the top priority. But another important issue that's attracting increasing attention is making sure the cornea is as healthy as possible before any surgery takes place. Here, five surgeons share their experience: What should surgeons be looking for before ocular surgery? What tests will most effectively reveal existing problems? If a problem is present, how much time is required to treat it? Does it make sense to pre-treat all patients to maximize outcomes? And if so, what protocol is most effective?
Evaluating the Cornea
"I think physicians in general are doing a much better job of evaluating the ocular surface before cataract and refractive surgery today than they were just a few years ago," says Eric D. Donnenfeld, MD, clinical professor of ophthalmology at New York University Medical Center and a partner at Ophthalmic Consultants of Long Island. "However, there's still a great deal we can do on a regular basis to dramatically improve our surgical results by improving the ocular surface—specifically, the tear film and meibomian gland orifices."
"With LASIK patients, surgeons know how important it is to prepare the ocular surface, temper expectations and treat dry eye afterwards," observes Parag A. Majmudar, MD, a cornea and refractive surgery specialist at Chicago Cornea Consultants Ltd., and associate professor of ophthalmology at Rush University in Chicago. "I think that's finally carrying over to cataract surgery."
William B. Trattler, MD, who practices at the Center for Excellence in Eye Care in
"Some patients who have no complaints at all may have blepharitis, dry eye or epithelial basement membrane disease.
"All of these can be problematic if they remain untreated before cataract surgery," he notes. "First, we need a good tear film to get accurate keratometry; dry eye or blepharitis can lead to placing the wrong power IOL or placing a toric IOL in a less-than-desirable axis. And anterior blepharitis is often associated with excess bacteria, a potential source of infection.
"A postoperative problem might not surface right away; it could appear two or three weeks or a month later," he continues. "The consequences of missing subtle corneal problems won't be so serious as to cause a disaster, but if our goal is to deliver the best care possible and make every patient as happy as possible, this is not ideal. You may have done a perfect surgery, but the patient will think you didn't."
"Unless you actively look for these issues, you're not going to find them," adds Dr. Majmudar. "And let's face it; we're all trying to see more patients in less time and make ends meet despite the economy. The reality is that nothing kills efficiency more than an unhappy patient sitting in your chair. That's a very practical reason to go out of your way to look for these problems ahead of time."
Dr. Trattler adds that on a few occasions, clearing up preop corneal surface problems has a dramatic effect by itself. "Occasionally I've addressed a patient's dry eye or blepharitis and then realized he didn't actually need surgery at that time because the dry eye or blepharitis was responsible for reducing his vision. It's not that common, but it has happened."
Comparing Preop Checklists
Dr. Donnenfeld describes his protocol for uncovering potential corneal health issues.
"We ask any patient who is going to have surgery for his ocular history, listening specifically for contact lens intolerance, visual fluctuations, dryness, tearing or burning—buzz words for dry eye. Once we have that history, we then do the physical examination. We start at the eyelid margins. If we see significant lid margin disease, we treat it. It's just as important as treating aqueous-deficiency dry eye because lipid or meibomian gland instability causes just as much trouble as aqueous deficiency does.
Once I get past the lid margins, I look at the tear film. Is it adequate? Is there debris in it?
"My gold standard is lissamine green staining of the conjunctiva and cornea before any type of surgery," he continues. "Interpalpebral staining suggests aqueous-deficiency dry eye. Inferior cornea and conjunctival staining suggests meibomian gland dysfunction and staph sensitivity problems. If the staining is interpalpebral but not in a V-shaped distribution, it suggests exposure keratitis. If it's superior staining it suggests superior limbic keratoconjunctivitis. You can also see things like lid imbrication syndrome and floppy eyelid syndrome.
"If the patient has mild staining, I'll treat aggressively before surgery," he concludes. "If the patient has significant staining, I'll have him come back to the office for another preop exam to make sure the problems are resolved before we go to surgery."
Dr. Donnenfeld says there's not much difference between what he looks for prior to LASIK or cataract surgery. "However, there's more corneal anesthesia after LASIK, and that loss of sensation causes more postop dry eye than patients experience after cataract surgery," he notes. "So, I try to optimize the ocular surface more for LASIK than cataract surgery. However, it's important to do this before either type of surgery."
Dr. Trattler agrees that fluores-cein staining is a key test to perform before ocular surgery. "We had a doctor who was doing his first Crystalens on a patient," he says.
"He did a perfect surgery, but the patient ended up 20/40 best-corrected. Then he put the dye in and discovered the patient had significant epithelial basement membrane dystrophy. I did a phototherapeutic keratectomy and that fixed the patient's vision. But the patient was obviously disappointed; he spent a lot of money and expected a wonderful result and ended up with not-so-great vision right after surgery.
"Also, check the eyelids for anterior blepharitis," he continues. "Even a LASIK surgeon can overlook the lids.Look at the eyelashes for scaling, little flecks of oil that have dried up on the lashes. You can also have the patient look down and press on the upper eyelids to see the quality of the oils. If you see a thick paste in the oil glands, that may indicate that they're clogged. We now have some very good treatments for this, including topical azythromycin."
Lisa B. Arbisser, MD, clinical adjunct associate professor at the University of Utah John A. Moran Eye Center, says her standard workup includes a slit-lamp exam and staining for all patients, plus topography and optical coherence tomography for premium-lens patients. She notes that you need to be careful about interpreting the corneal surface condition if you see the patient after drops have been inserted. "By the time I see a patient in my office, she's already dilated, which means she's had two kinds of drops," she explains. "For that reason, the corneal surface may not look pristine when I see it, and we may not be able to get a good measurement with topography. So I have to make sure it's not just a reaction to the drops. In that situation I'll have the patient use some artificial tears and come back again later."
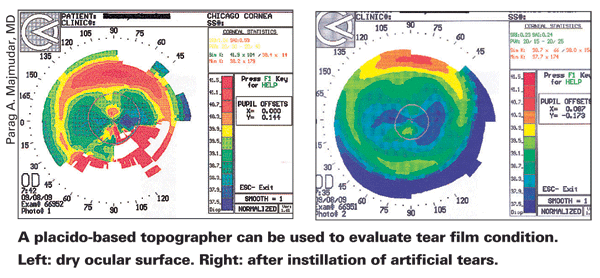
Dr. Majmudar says that in addition to irregularities of the ocular system and retinal issues, he looks for corneal scars and dystrophies like EBMD. "These need to be treated before doing any kind of surgery," he notes. "I also screen all patients for blepharitis because the number one source of postoperative endophthalmitis is the patient's own ocular surface flora. To check the quality of the tear film I use the slit lamp, as well as a placido topographer that reflects light off the tear film; if the patient's tear film isn't pristine, I see topographic abnormalities. (See scans, above.) In addition, I stain with fluorescein or lissamine green and look at tear breakup time.

Dr. Majmudar also looks at conjunctival chalasis. "I've found this to be a very sensitive indicator of tear-film dysfunction," he explains. "Dur-ing the slit-lamp exam, check the lateral border of the bulbar conjunctiva where it comes into contact with the lower lid; you may see a sort of redundancy or wrinkling of the conjunctiva. That's a pretty sensitive and specific indicator that the patient has mild to moderate dry eye."
"In terms of rosacea, blepharitis or dry eyes, the most problematic patient is usually a female," notes Karl Stonecipher, MD, medical director for TLC Laser Eye Centers in Greensboro, N.C. "Many patients will come in and not have any complaints, especially many peri- or postmenopausal females, even though their eyes may be very dry. You won't know there's a problem unless you look for it. In addition, many women come in wearing makeup, which can hide the signs of a problem. In this situation, you have to be more astute about listening to patient complaints. If I hear someone discussing fluctuating vision, or saying they wake up with poor vision in the morning or have poor vision in the afternoon, those are telltale signs that they're having dry eye—aqueous deficient or evaporative. In any case, we use lissamine green in the lane to look at patient's ocular surface and tear-film quality."
Treating Dry Eye
Once a specific problem turns up during the preop exam, appropriate treatment is essential to a good surgical outcome. Restasis has become a common part of most surgeons' treatment for preop dry eye—although its use raises issues regarding how much time is required for it to have a significant effect.
Dr. Stonecipher says that when it comes to treating dry eye, he's a fan of Restasis and omega-3. "In a series I published some time ago1 including about 10,000 patients, we saw an effect from the Restasis in more than two-thirds of the patients within three to five weeks," he notes. "So I find that if I put these patients on Restasis for a month preop, most of them do very well. In many instances I'll also jumpstart the patient with a steroid such as Lotemax." He adds that Restasis appears to have some effect even over a shorter period of time. "Most of the studies we've looked at say that within one to two weeks you're getting some effect," he notes. "In moderate to severe dry eye, I'd recommend two to four weeks, based on Ocular Surface Disease Index scores."
Dr. Donnenfeld agrees. "We usually start the medications two weeks before surgery—longer if possible," he says. "But even at two weeks we see a significant improvement in visual outcomes. In the FDA Restasis trial, some differences were statistically significant even at one month."
Dr. Arbisser says that rather than rely on Restasis, she favors a more traditional approach. "I have the patient use preservative-free tears every two hours," she says. "I do lid hygiene. I may use AzaSite, which has anti-in-flammatory properties, if there's any meibomitis or blepharitis component. If the dry eye doesn't have a big inflammatory component and is primarily aqueous-deficient, I may insert temporary collagen punctal plugs at the time of surgery."
Dr. Trattler says he treats dry eye with Restasis, topical steroids and punctal plugs. "I don't mind using all three at once, just to get things moving in the right direction," he notes.
Treating Dystrophy
"One of the major things that keeps patients from being a 'perfect 10' after cataract surgery is surface problems," says Dr. Arbisser. "Most of these problems are tear-film-related, but the next most common is some sort of anterior membrane dystrophy. What you see at the slit lamp is little whorls and dots and spots with either a flat surface—Cogan's map-dot-fingerprint dystrophy—or a lumpy surface—Salzmann's nodular dystrophy."
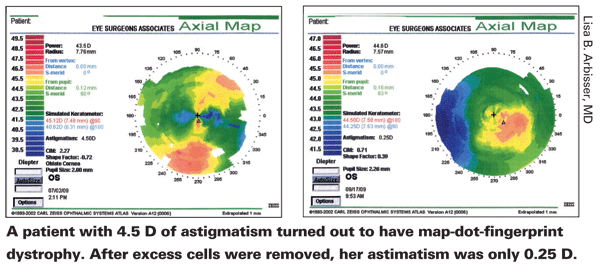
Dr. Arbisser believes dystrophy is far more common than most surgeons think. "You really have to look for it, because it's terribly important," she says. "For example, astigmatism may result from curvature of the stroma—or from cells heaped up on the surface because of dystrophy, which can easily be mistaken for a curvature issue. I recently had a patient who came in with 4.5 D of astigmatism on topography and a corresponding correction in her glasses. I realized she had map-dot-fingerprint dystrophy, and decided that rather than attempting to correct her astigmatism with a toric lens, I would first scrape off the excess cells. After I did so, she only had 0.25 D of astigmatism." (See scans, above.)
Dr. Stonecipher says that, being cornea trained, he's fairly aggressive about looking for basement membrane dystrophy. "If I find it, I don't change my regimen dramatically in most cases," he notes. "However, I may change my surgical approach. If someone with basement membrane dystrophy is having fluctuating vision, I may do a PRK or surface laser ablation instead of LASIK because there's less potential for complications."
Dr. Trattler notes that if you re-move the epithelium before surgery, you should wait about two months before going ahead with the cataract surgery. "I usually won't offer patients a presbyopic IOL unless I perform PTK and they achieve a smooth epithelial surface," he says. "Otherwise, these patients may end up with re- duced best-corrected visual acuity following cataract surgery."
Treating Blepharitis
"When we find that a patient has perioperative blepharitis, our current regimen is to use AzaSite and doxycycline preop," says Dr. Stonecipher. "The reasons for the doxycycline are obvious. We use AzaSite because we've found that it's potent in terms of reducing the bacterial load. It penetrates the tissues well, and it's persistent because of the vehicle that AzaSite is associated with—DuraSite.
"I don't think AzaSite is a great postop drug, but used preop to reduce any eyelid disease, it's been very successful for us in terms of postop day-one vision, as well as predictability and outcomes," he adds. "In addition, I have yet to have a premium IOL or LASIK infection postop, out of tens of thousands of cases."
Dr. Donnenfeld says his treatment for lid margin disease is hot compresses and oral nutritional supplements. "I'm also a big believer in topical azithromycin drops applied to the lid margin once a day for a month to improve the meibomian gland secretions and reduce inflammation," he says. "If a patient has really bad lid disease, I'll sometimes add oral doxycycline. Even really low-dose doxycycline, such as 50 mg a day, can be sufficient."
Dr. Arbisser notes that AzaSite has many advantages over previous treatment options for blepharitis, but the cost to the patient is a serious concern. "It's very convenient," she says. "It's used twice a day for two days, then once a day for a week. It doesn't blur vision. And it has an anti-inflammatory component to it, which is great. The problem is that it's not well-covered in formularies and it's expensive.
Other Management Concerns
Other issues to consider:
• Rosacea. "Rosacea can be easy to spot," says Dr. Donnenfeld. "Most ophthalmologists are aware of the combination of telangiectasia and pustules and rhinophyma. But in women it's less obvious and in African Americans it's more difficult to see the erythema and the pore sizes. To make sure you don't miss this, look carefully at the lid margins. I'll often see inspissated meibomian glands, erythema and scarification. If I see a lid-margin problem, it's a lot easier to make a systemic diagnosis."
Dr. Donnenfeld notes that rosacea has a significant impact on meibomian gland secretions. "It's one of the few situations in which I'll use oral doxycycline on a routine basis before surgery to improve the tear film," he says. "AzaSite also makes a big difference in improving meibomian gland secretions and stabilizing the tear film."
• Pterygium surgery. Dr. Majmudar notes that it's especially important to optimize the surface as much as possible before this type of surgery. "Pterygium surgery is a special case, because the surgery causes so much disruption of the ocular surface," he explains.
"The surgery can cause ocular surface inflammation for three to four weeks afterwards."
Dr. Trattler agrees. "Patients with dry eye are prone to thinning and drying following pterygium surgery," he points out. "You have to be aggressive in identifying and treating dry eye, both ahead of time and after surgery."
• Glaucoma patients. Dr. Arbisser notes that patients who have been using glaucoma drops for a significant period of time may have resulting damage to the corneal surface that requires special attention. She suggests that one way to improve the corneal surface before surgery is to reduce the patient's eyedrop load by performing selective laser trabeculoplasty. "This may enable the patient to reduce the number of meds he's using significantly," she says. "However, if you do this, you'll need to postpone further surgery for a while in order to avoid using steroids right away. The mechanism of SLT appears to be that the body cleans out the debris in the trabecular meshwork in response to the mild inflammation you create by using the laser; steroids might suppress the beneficial effect of the SLT."
A Universal Preop Regimen?
In addition to looking for specific corneal health issues, many surgeons have adopted a strategy of treating all pre-surgical corneas as a way to maximize the health of the surface and minimize any subclinical problems. This generally involves some combination of preop steroids, antibiotics and/or NSAIDs.
"For both cataract and LASIK surgery I have the patient use a steroid and antibiotic four times a day for three days preop," says Dr. Stonecipher. "When I'm implanting a premium IOL I also add an NSAID to the regimen. For LASIK patients I've been using a steroid and a fluoroquinolone preoperatively for quite some time; I believe it allows me to improve the tear film by reducing any mild blepharitis or meibomitis. When we test on the day of surgery—whether that means wavefront or a repeat manifest refraction—we get a more solid number. The predictability of our postop outcomes has been better.
"Initially, we thought we should just do this kind of preop regimen in the cataract arena for the diabetics and the high-risk inflammatory patients—post-iritis or uveitis patients," he continues. "And in the LASIK arena, we looked at it originally for the high-risk patients and health-care workers. But my philosophy from the beginning was, if it's going to help those people, then it's going to help others as well."
Dr. Stonecipher notes that once you decide there's a benefit to using a preop regimen, the question becomes: How early do you begin treating? "I ended up deciding that three days before surgery was most beneficial, based on observation and reviewing
the literature," he says. "I don't be-lieve that one day is enough to make the necessary beneficial changes to the tear film or eyelid margins."
Dr. Stonecipher takes one additional step for patients he believes are at high risk, including providers of medical care and individuals who work in the farm, poultry and dairy industries—adding Polytrim to the regimen, preop and postop. He notes that gentamicin is another possible choice, since both drugs reduced methicillin-resistant staph in the Ocular TRUST (Tracking Resistance in the United States Today) study.
Dr. Donnenfeld favors the routine use of Restasis before many types of surgery. "We've found, for example, that the routine use of Restasis before LASIK surgery reduces neurotrophic keratitis and improves visual outcomes," he says. "We've also found that patients who are having premium IOL surgery benefit greatly from the use of topical cyclosporine to improve the quality of the tear film."
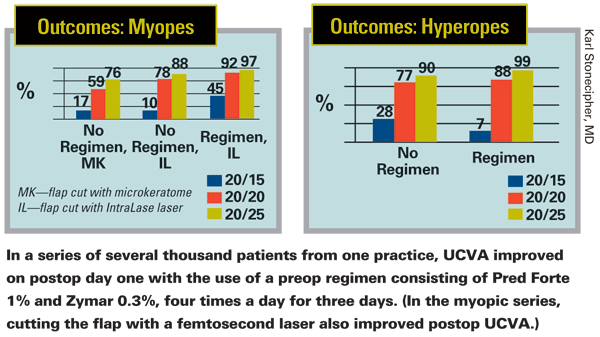
Of course, some surgeons are skeptical. "Eventually, somebody asked me to prove that my preop protocol works," says Dr. Stonecipher. "I realized that conducting a large, randomized, controlled study would be very costly, but we did look at a series of our patients and found that when myopes or hyperopes undergoing LASIK followed this preop regimen, postop day-one vision improved compared to the vision of those who didn't receive the regimen. (See charts, above.) In addition, a study that was recently published found that perioperative prophylaxis with an NSAID reduced macular edema postop.2 It's certainly possible that some patients have subclinical macular edema that we don't pick up; by treating these people aggressively pre- and postop, we're going to improve both the quality and quantity of vision attained."
It's worth noting that not everyone is impressed with Restasis as a pre-cataract surgery treatment. "I've tried Restasis before cataract surgery because others have said that pretreating improves outcomes," explains Dr. Arbisser. "That has not been my experience. In fact, I noted an increase in patient complaints of irritation."
The Coming Thing?
"More and more cataract surgeons are treating patients preop with NSAIDs or other regimens," notes Dr. Stonecipher. "But with LASIK, this is not yet commonplace. I think what's been holding us back is the cost factor and the lack of an overwhelming study with a large series proving that such a protocol reduces or eliminates postoperative infections. Unfortunately, I don't think we'll ever see that study performed because of the cost involved. Given that reality, at some point I believe we need to take a leap of faith and treat our patients.
"Of course, there are potential downsides to a more extensive preoperative regimen, such as cost and patient compliance," he admits. "But in our practice we haven't found that a three-day preop treatment adds to the patient's cost—it appears that there's enough medicine in the bottle for most patients to use them preop and complete the postop regimen without a refill. And in terms of compliance, once we explain the reasons for the protocol to the patient, it's been a pretty straightforward sell."
Dr. Donnenfeld summarizes the growing consensus. "Pay attention to the lid margin, the tear film and the corneal stain pattern," he advises. "If you take the time to improve the ocular surface, your surgical results will dramatically improve, and patient satisfaction will improve with them."
1. Stonecipher K, Perry HD, Gross RH, Kerney DL. The impact of topical cyclosporine A emulsion 0.05% on the outcomes of patients with keratoconjunctivitis sicca. Curr Med Res Opin 2005;21:7:1057-63.
2. Wittpenn JR, Silverstein S, Heier J, Kenyon KR, Hunkeler JD, Earl M; Acular LS for Cystoid Macular Edema (ACME) Study Group. A randomized, masked comparison of topical ketorolac 0.4% plus steroid vs. steroid alone in low-risk cataract surgery patients. Am J Ophthalmol 2008;146:4:554-560.



