Here, I’ll review some of the basic steps an ophthalmologist who is not a specialist in pediatric glaucoma can take to identify and manage a child who presents with possible signs of glaucoma. I’ll also share some of the latest thinking on how the different types of childhood glaucoma can be most effectively categorized and addressed.
Diagnosing the Problem
When you want to make a judgment about whether a child has glaucoma, you should follow these steps:
• Assess the child’s overall appearance and behavior. The first thing to do is step back and take a look at the child. Is there anything abnormal in the child’s appearance? Does the child seem to have a problem, or be entirely well?
• Check the child’s history. Has the child had a past problem with his eyes? If the child has had a cataract removed, that child is automatically at risk for getting glaucoma. The child might have been injured, which could trigger glaucoma. The child might have a form of childhood inflammation in the eye called juvenile idiopathic arthritis or uveitis, in which case joints could be involved as well.
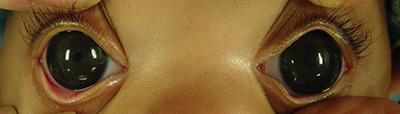 |
| This 4-month-old child presented with large, hazy corneas and was diagnosed with primary congenital glaucoma. The photograph was taken during examination under anesthesia, just prior to angle surgery that successfully reduced the elevated intraocular pressure and controlled the glaucoma. |
— Enlarged eyes. Early in life our eyes are still expandable and stretchy. As a result, elevated intraocular pressure from early onset of a condition such as primary congenital glaucoma can cause one or both eyes or corneas to become larger. (See example, above.) So, if a child’s cornea is larger than you would expect at that age, that should make you suspicious of the possibility of glaucoma. (You can estimate the cornea’s width by holding a ruler or a card with a ruler printed on it up to the eye.)
Ironically, these kids are often thought to have beautiful eyes, and they get compliments everywhere their parents take them. It may take some time for everybody to realize that the large eyes are the result of a disease.
— Hazy corneas. The haze could be the result of corneal edema or breaks in Descemet’s membrane caused by elevated pressure (Haab striae).
— Behavior indicating light sensitivity. Corneal changes in childhood glaucoma with onset in infancy can produce photophobia, so a very young child with primary congenital glaucoma will often be squinting, tearing or squeezing the eyelids to avoid bright light.
— Asymmetry between the eyes. If the glaucoma is affecting one eye more than the other, the affected eye may be larger or have more haze on the cornea. Generally, it’s the bilateral, symmetrical cases that get missed because both eyes look the same. If one eye starts getting bigger than the other, the parent, pediatrician or an eye-care provider will usually notice.
— Abnormal iris. The iris may be abnormal in Axenfeld-Rieger syndrome or in aniridia, where most of the iris is missing.
— Shaking eyes. Nystagmus in a young child is often a sign of poor vision and possible glaucoma.
• Try to assess vision. The most effective way to do this depends on the age of the child. An older child may be able to read the Snellen chart. If the child is younger, you may have to see if the child can fixate on a toy or an interesting object such as a face, and follow it. Myopia can sometimes result from the elevated pressure associated with glaucoma, since high pressure can stretch the eye; the stretching increases the eye’s axial length, making the child myopic in one or both eyes. (Most healthy children are actually hyperopic when they are very young.)
• Try to assess intraocular pressure. This can often be accomplished with the instruments you would use in adults, but you may need to use them in modified form. For example, we often attempt to check the pressure in the clinic with an iCare rebound tonometer, which can be done without an anesthetic.
One important note: Try to keep the child happy. A common mistake is to do something such as holding the child down to check the intraocular pressure. If the child is crying or doing a valsalva maneuver the pressure is going to be artificially elevated. So if the child is crying, the reading you get won’t mean much.
• Try to assess the condition of the optic nerve. Abnormal cupping can also be a sign of glaucoma. Most healthy children don’t have a lot of cupping, especially when they’re very young; they usually have a good rim, and good symmetry in the appearance of the optic nerve in both eyes. Of course, looking at the optic nerve may not be easy in some children, unless you’re an experienced pediatric ophthalmologist or pediatric glaucoma specialist.
It’s worth noting that some surgeons might expect us to put a child under anesthesia in order to conduct an exam. Certainly there are things you need to put a child to sleep for, but most pediatric glaucoma specialists won’t use anesthesia unless we’re already pretty sure that something is seriously wrong with the child. Furthermore, in that situation we wouldn’t be simply collecting data or doing gonioscopy, we’d be deciding what we need to do to address the problem: how severe it is; what type of problem is it; and what surgery would be most appropriate to treat the child, if surgery is indeed needed.
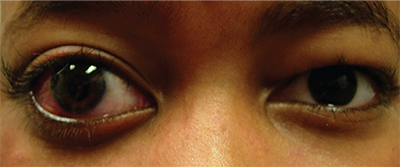 |
| This child was born with a port wine mark on the right side of his face involving his upper eyelid. He developed seizures and was noted to have an enlarged and often pink right eye. Glaucoma was diagnosed when he was 18 months old, and required medications as well as glaucoma drainage implant surgery to control. The left eye is unaffected and is normal. |
Pediatric glaucoma specialists often use medications to manage glaucoma in children, but many types of glaucoma in young children are primarily surgical diseases. In those cases, we only use medications as either a temporizing measure before we do surgery or as an adjunct to surgery postoperatively. For example, primary congenital glaucoma is a surgical disease; we do either a goniotomy or a trabeculotomy to open the drainage angle. Often, we don’t need any medicine long-term if the surgery works well enough.
On the other hand, some types of childhood glaucoma can be treated using medication as the first-line therapy. In those cases, surgery would be used only if the medications aren’t adequate to keep the pressure under control, pretty much as you would do with an adult. However, medications have to be used very judiciously in children; some children can be injured by giving them medication that isn’t appropriate. I recently saw a 10-week-old baby who was given both brimonidine 0.15% and timolol 0.5%; it put the baby in the hospital with bradycardia and lethargy. The beta-blocker was too strong for a baby, and the alpha-2 agonist brimonidine is absolutely contraindicated in babies. So medications can be used to treat some types of childhood glaucoma, but they must be used with care.
Defining Pediatric Glaucomas
Once a diagnosis is made, deciding how to proceed can be a challenge. The numerous types and sources of glaucoma found in children have contributed to a lack of agreement about how best to manage some of the variations.
The different disorders falling under the umbrella of “childhood glaucoma” have a variety of severities and prognoses—from mild to moderate to severe, in terms of the glaucoma itself and the impairment of the child’s vision—and each child’s response to therapy can be very different.
Because all of these diseases are relatively uncommon, the literature is sparse and sometimes confusing. If I’m treating one of the glaucomas that responds very well to treatment X, and you’re treating a much more difficult subgroup of patients that doesn’t respond so well to treatment X, what do we make of that? These circumstances have made it difficult to come up with any sort of optimal strategy for managing pediatric glaucoma, so the same type of childhood glaucoma may be treated very differently in different parts of the world.
My colleagues and I have at-tempted to reduce some of the confusion and improve diagnosis, treatment and outcomes by coming up with standardized guidelines for how to treat some types of childhood glaucoma. Allen Beck, MD, and I were both involved as pediatric glaucoma specialists in the Infant Aphakia Treatment Study, a randomized, con-trolled trial comparing the efficacy of implanting an intraocular lens vs. aphakia in babies with a unilateral cataract. One of the dreaded complications of removing a cataract from a baby’s eye is glaucoma, so we and the study’s lead investigator, Scott Lambert, MD, realized that we needed a consistent, specific definition of glaucoma and glaucoma suspect in these babies. (It may be very obvious if a child has full-blown glaucoma, but determining when or if a child is developing glaucoma can be very difficult.)
Once we developed clear criteria for that, we decided to use those definitions as a basis for a much larger project. The Childhood Glaucoma Research Network, a volunteer group of experts in pediatric glaucoma from all over the world, took on the task of agreeing upon a definition of childhood glaucoma and a consensus classification system of the types of childhood glaucoma, building upon much work that has already been done by many dedicated leaders in the field over many decades.
| If you’re not used to working with children, you should team up with someone who takes care of a lot of kids with this type of problem. |
The Four Most Common Types
If you’re a comprehensive ophthalmologist, it’s important to re-member that glaucoma in children is a group of diseases. In particular, you should recognize four categories of childhood glaucoma.
First, the most common primary glaucoma in children—meaning glaucoma that’s not caused by another problem—is primary congenital glaucoma. If you see a baby who is otherwise well but has a big eye, a teary eye or a cloudy eye, a diagnosis of primary congenital glaucoma will be correct most of the time. This is a surgically treated disease, and you need to get that child to a glaucoma specialist.
The second most common kind of childhood glaucoma is glaucoma that occurs following cataract removal. If a baby or young child has had a cataract removed, that child’s eye is at lifelong risk of glaucoma. The median age of onset is 5 years old, but some children will get much older before a problem develops. These individuals may even go off to college, by which time everybody thinks any risk of glaucoma has passed. They are done with amblyopia, they’ve had a lens implant or they’re wearing a contact lens; but then suddenly they present to a comprehensive ophthalmologist with glaucoma in that eye.
This is a secondary glaucoma, a type that would be treated first with medications. A comprehensive ophthalmologist could certainly begin the treatment in this situation, especially in the case of a child who is old enough to be able to sit at the slit lamp, get her pressure checked and get her optic nerve photographed.
The third kind of childhood glaucoma a comprehensive ophthalmologist should be aware of is any glaucoma caused by a separate problem—for example, an eye that has undergone trauma or has inflammation uveitis. These eyes are definitely at risk for glaucoma, so if you are the primary care provider you should be alert for any signs of glaucoma developing in a child who fits this description. These eyes would be treated first with medication, provided the angle configuration was open. (Angle closure requires surgical intervention.)
Finally, there’s an unusual type of primary glaucoma called juvenile open-angle glaucoma; this is very similar to the kind of open-angle glaucoma that the elderly get—the kind a comprehensive ophthalmologist treats all the time.
This type of pediatric glaucoma typically shows up in a school-age or early teenage child. Notably, this may be a child who comes in to get eyeglasses because of myopia. In fact, when you’re dealing with children, you should treat every myopia patient as a possible glaucoma suspect. If you routinely check the pressure and look at the nerve when a child comes in with myopia, you won’t miss one of these cases.
Most Important: Take Action
The good news for the comprehensive ophthalmologist is this: If you simply use common sense, most of the time you’ll see lots of clues that something is not right with a child who has glaucoma. The most important thing is to recognize that the child you’re seeing has a problem and not let it go past. I’ve seen really bad cases where a child has a cloudy, teary eye, and the pediatrician has been calling it a blocked tear duct. Or the child is thought to be shy because light sensitivity makes the child not want to look up at anybody. Sometimes it isn’t until the child develops nystagmus that the glaucoma is diagnosed.
If you’re a comprehensive ophthalmologist and you suspect glaucoma in a child, don’t hesitate to contact someone who has more expertise. In some areas where there is no pediatric glaucoma specialist, that might mean working with an adult glaucoma specialist. In other areas, a pediatric ophthalmologist can be the first line of defense. The pediatric ophthalmologist may then, in turn, pass the patient along to an adult glaucoma specialist if certain types of surgery are needed which are not in the armamentarium of the pediatric ophthalmologist.
If you’re a glaucoma specialist and you strongly suspect a child of having glaucoma, it’s OK to attempt to address the problem. However, if you’re not used to working with children, you should team up with someone who takes care of a lot of kids with this type of problem. It’s an unusual enough condition that there are tricks and tips an average glaucoma specialist may not be familiar with—things the average comprehensive ophthalmologist certainly won’t be familiar with. REVIEW
Dr. Freedman is a professor of ophthalmology and pediatrics and chief of the Pediatric Ophthalmology and Strabismus Service at Duke Eye Center in Durham, N.C.
1. Beck AD, Chang TCP, Freedman SF. Definition, classification, differential diagnosis. In: Weinreb RN, et al., eds. Childhood Glaucoma: Consensus Series 9. Amsterdam: Kugler; 2013:3-10.



